May 14, 2026
In a landmark shift for women’s health and endocrinology, a global coalition of clinicians, researchers, and patient advocates has officially proposed renaming Polycystic Ovary Syndrome (PCOS) to Polyendocrine Metabolic Ovarian Syndrome (PMOS). The announcement, delivered in a comprehensive report timed with the European Congress of Endocrinology this month, marks the end of a decade-long debate over a name that many experts argue is both medically inaccurate and clinically limiting.
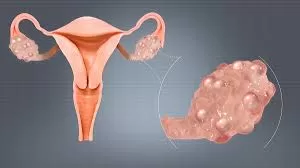
The move aims to modernize the approach to a condition that affects an estimated 170 million people worldwide. By moving away from a name that prioritizes “cysts” on the ovaries—which are often not present and are not the primary cause of the disorder—the new PMOS label highlights the systemic hormonal and metabolic disruptions that define the condition. This transition, which will phase in over the next three years, signals a major pivot toward earlier screening for life-altering risks like type 2 diabetes and cardiovascular disease.
Beyond the Ultrasound: Why the Name Is Changing
For nearly a century, the term “polycystic” has dominated the conversation. Historically, the condition was named for the appearance of ovaries on an ultrasound—specifically, the presence of many small, fluid-filled sacs. However, under the long-standing “Rotterdam criteria” used for diagnosis, many patients do not actually have these “cysts,” and many people with them do not have the syndrome.
The new name, Polyendocrine Metabolic Ovarian Syndrome (PMOS), was carefully chosen to reflect the three pillars of the disorder:
-
Polyendocrine: Acknowledging the multi-hormonal imbalances, including elevated androgens (male-pattern hormones).
-
Metabolic: Recognizing the central role of insulin resistance and its impact on long-term health.
-
Ovarian: Retaining the link to reproductive health and ovulatory dysfunction.
“The old label emphasized ovarian morphology rather than the broader endocrine and metabolic disruption that drives most long-term harms,” noted one clinician involved in the report. By rebranding as PMOS, proponents believe doctors will be more likely to look beyond the reproductive system and order essential metabolic screenings, such as glucose tolerance tests and lipid profiles.
A Global Burden: The Reality of PMOS
PMOS is the leading cause of anovulatory infertility globally, affecting roughly 1 in 8 women and people assigned female at birth. Despite its prevalence, it remains one of the most underdiagnosed and misunderstood conditions in modern medicine.
The symptoms are notoriously heterogeneous, making diagnosis a “puzzle” for many patients:
-
Reproductive: Irregular periods or a total lack of ovulation.
-
Physical: Acne, thinning scalp hair, or hirsutism (excessive facial or body hair).
-
Metabolic: Unexplained weight gain, high blood pressure, and insulin resistance.
The World Health Organization (WHO) has highlighted that early intervention is critical, yet many patients spend years visiting multiple specialists before receiving a correct diagnosis. Experts hope the PMOS label will streamline this process.
Expert Perspectives: Progress vs. Practicality
While the consensus for the name change was reached alongside patient representatives to ensure it remains “patient-centered,” independent specialists are weighing the logistical hurdles of such a massive shift.
“The new name better describes the systemic effects we see in our patients every day,” said one reproductive endocrinologist not involved in the consensus work. “However, renaming a well-known disorder carries risks. It will require coordinated updates to clinical guidelines, insurance coding systems (ICD codes), and patient education materials to avoid massive confusion during the transition.”
There are also concerns regarding the “brand recognition” of PCOS. Advocacy groups have spent decades building awareness under the old acronym. Some advocates worry that changing to PMOS might disrupt peer-support networks and complicate online searches for medical information in the short term.
Public Health and Practical Implications
The shift to PMOS is not just a semantic update; it is intended to be a clinical “re-calibration.” For the general public, this means a shift in how care is delivered:
1. Shift in Screening
Currently, many patients are only treated for the symptom that bothers them most—such as acne or difficulty conceiving. Under PMOS guidelines, clinicians are encouraged to treat the condition as a metabolic priority. This means earlier and more frequent monitoring for:
-
Impaired Glucose Tolerance: To prevent the progression to type 2 diabetes.
-
Dyslipidemia: Monitoring cholesterol levels to reduce cardiovascular risk.
-
Mental Health: Screening for anxiety and depression, which are significantly more common in those with this syndrome.
2. Fertility Care
For those seeking to conceive, the core issue remains ovulatory dysfunction. While the name change emphasizes metabolic health, the underlying fertility treatments—such as ovulation induction—remain evidence-based and effective. However, the PMOS framework encourages a “whole-body” approach to pregnancy, ensuring the person is metabolically healthy before and during gestation.
3. A Three-Year Transition
Medical institutions plan to phase in the PMOS terminology through 2029. During this time, patients will likely see both names used in medical records and educational pamphlets.
What Should Patients Do Now?
If you have been diagnosed with PCOS, your medical reality has not changed, but your care plan might. Experts suggest the following steps for those navigating the transition:
-
Don’t Panic: Your current treatment plan is still valid. The renaming is a tool for doctors to provide better, more comprehensive care.
-
Ask About Metabolism: If you haven’t had a recent fasting glucose or lipid panel, ask your provider if these are appropriate for you under the new PMOS framework.
-
Advocate for Holistic Care: Discuss how your hormonal health might be affecting your skin, hair, mood, and energy levels, not just your cycle.
As the medical community moves toward the PMOS era, the goal remains clear: to ensure that the millions of people living with this syndrome are seen not just as patients with “cysts,” but as individuals requiring comprehensive, life-long endocrine and metabolic support.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://health.economictimes.indiatimes.com/news/industry/a-new-name-for-pcos-the-most-common-cause-of-infertility/131057382?utm_source=top_story&utm_medium=homepage