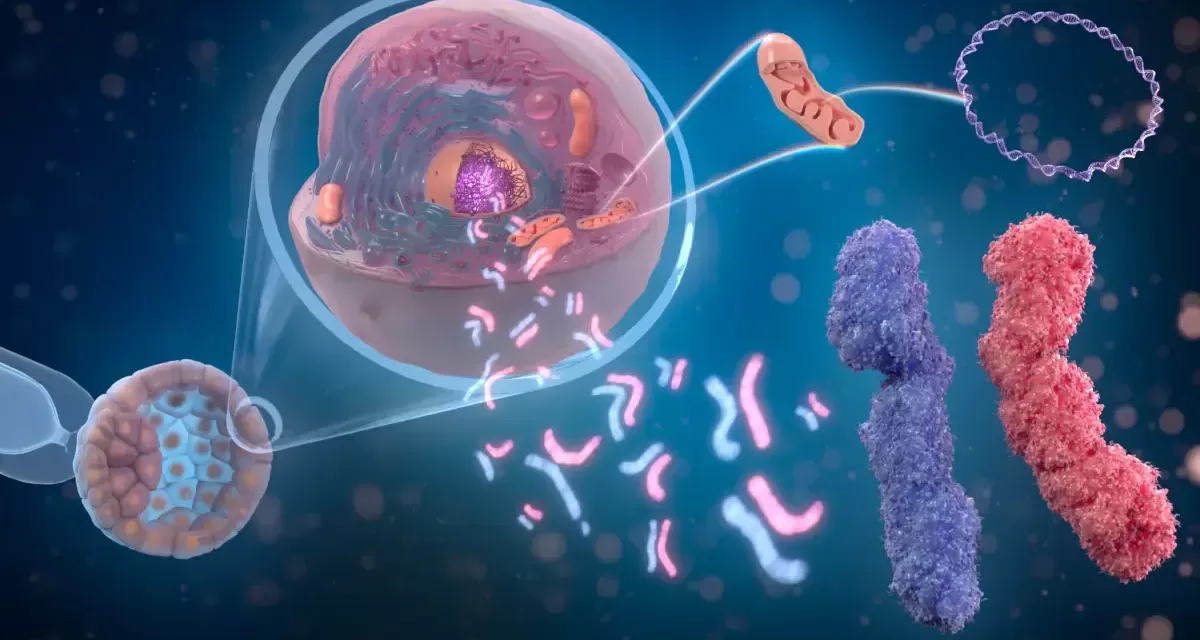
NEW DELHI — In a landmark shift for precision medicine in South Asia, a nationwide genomic analysis from the GenomeIndia initiative has revealed that Indian populations carry a vast array of genetic variants entirely absent from Western databases. The study, released this week, finds that many of tribal and regional groups across the country exhibit concentrated risks for inherited diseases that have previously gone undetected by global screening standards.
The findings challenge a long-standing assumption in modern medicine: that disease-risk models and treatment predictions developed using data from Europe and North America can be reliably “copy-pasted” onto Indian patients. Researchers warn that relying on these Euro-centric models may lead to misdiagnoses and ineffective treatment plans for one-sixth of the world’s population.
Uncovering the “Missing” Genetic Map
The GenomeIndia project, a government-funded multi-institutional effort, successfully sequenced the whole genomes of approximately 10,000 individuals representing 83 distinct population groups. The data, now archived at the Indian Biological Data Centre, serves as a high-resolution map of the country’s staggering biological diversity.
The scale of the discovery is significant. Investigators reported nearly 1.5 million protein-coding variants that had never been seen in existing global databases.
“This is a major milestone,” says Dr. Mohammed Faruq, a scientist at the CSIR-Institute of Genomics and Integrative Biology (IGIB) and a key contributor to the project. “The study surfaces novel findings from different Indian populations and highlights the vital importance of studying tribal genomic structures to inform better healthcare strategies.”
A striking revelation from the data is the high degree of “population structure.” Due to historical endogamy (marrying within specific communities), several tribal populations show elevated frequencies of variants associated with inherited disorders. In some instances, these rates are higher than those found in well-studied “founder” populations like Ashkenazi Jews or Finns, who are often the primary focus of genetic research in the West.
The Problem with “Western” Risk Scores
For years, clinicians have used Polygenic Risk Scores (PRS)—a mathematical estimate of a person’s genetic predisposition to diseases like diabetes or heart disease—derived almost exclusively from European-ancestry cohorts.
However, the GenomeIndia authors warn that these scores have limited predictive accuracy for Indians. Because the underlying variant frequencies and genetic “architecture” differ so substantially, a high-risk marker for a Londoner might be irrelevant for someone in Mumbai, while a critical risk factor for an Indian patient might not even be on a Western doctor’s radar.
Analogy: Using a European-derived genetic risk score for an Indian patient is like using a weather forecast built for London to plan agriculture in Mumbai. While some broad patterns (like “rain comes from clouds”) might hold true, the local timing, intensity, and environmental factors are so different that the forecast becomes practically useless for local decision-making.
Public Health Implications: From Diagnosis to Pharmacy
The divergence between Indian and Western DNA has immediate consequences for public health in three key areas:
1. Diagnostic Accuracy
Many genetic tests currently used in Indian hospitals were designed based on Western data. The discovery of millions of India-specific variants means these tests may suffer from “blind spots,” missing clinically relevant mutations or misinterpreting harmless variations as dangerous. This can lead to “diagnostic odysseys,” where families with rare genetic disorders spend years seeking answers that existing tests cannot provide.
2. Precision Medicine and Drug Safety
The field of pharmacogenomics studies how genes affect a person’s response to drugs. For example, certain liver enzymes (cytochrome P450) determine how quickly a body breaks down medication.
-
If a dosing algorithm is based on Western allele frequencies, an Indian patient might receive a dose that is either toxic or ineffective.
-
Without India-specific data, the risk of adverse drug reactions remains significantly higher.
3. Newborn Screening and Counseling
The identified risks in specific tribal and regional groups suggest an urgent need for localized healthcare interventions. Experts are calling for expanded newborn screening and culturally sensitive genetic counseling to manage the high prevalence of inherited conditions in these “founder” populations.
Challenges to Implementation
Despite the excitement, independent experts urge a cautious approach to clinical rollout. While the data is groundbreaking, several hurdles remain:
-
The “Translation Gap”: Identifying a genetic variant is only the first step. “Discovering variants is not the same as proving they cause disease,” notes a review in Frontiers in Genetics. Significant investment is needed in functional studies to confirm which of these 1.5 million variants actually impact health.
-
Sample Representation: While 10,000 genomes is a massive leap forward, India’s diversity is so vast that some subgroups remain under-sampled.
-
Clinical Infrastructure: Translating these insights into the clinic requires a massive scale-up of the genetic counseling workforce—a resource currently in short supply across many Indian states.
What This Means for You
For the average person, daily medical care will not change tomorrow. However, as this data integrates into the healthcare system, the impact will become tangible.
-
Question Your “Ancestry” Tests: If you are using direct-to-consumer genetic kits or ancestry-based health reports, be aware that their risk estimates are likely built on Western datasets and may be misleading for those of Indian descent.
-
Consult Specialists: If you have a family history of a rare disease, seek out clinicians who have access to local genomic resources rather than relying solely on international databases.
-
Support Local Research: The success of precision medicine in India depends on continued participation in local clinical trials and genomic studies.
As India builds its own reference genome, the goal is clear: a future where a patient’s treatment is dictated by their own biology, not by a model built for a different population on a different continent.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://www.daijiworld.com/news/newsDisplay?newsID=1314351