NEW YORK — Researchers at Rockefeller University have uncovered a sophisticated “gene-shredding” tactic used by Trypanosoma brucei, the lethal parasite responsible for African sleeping sickness. In a study that redefines our understanding of chronic infection, scientists found that the parasite deliberately breaks its own DNA to trigger a rapid change in its “molecular disguise,” allowing it to stay one step ahead of the human immune system. By inducing double-strand breaks in specific genetic regions, the parasite increases its ability to swap surface proteins by 250-fold, effectively rendering the host’s previous immune response obsolete.
The Ultimate Game of Hide-and-Seek
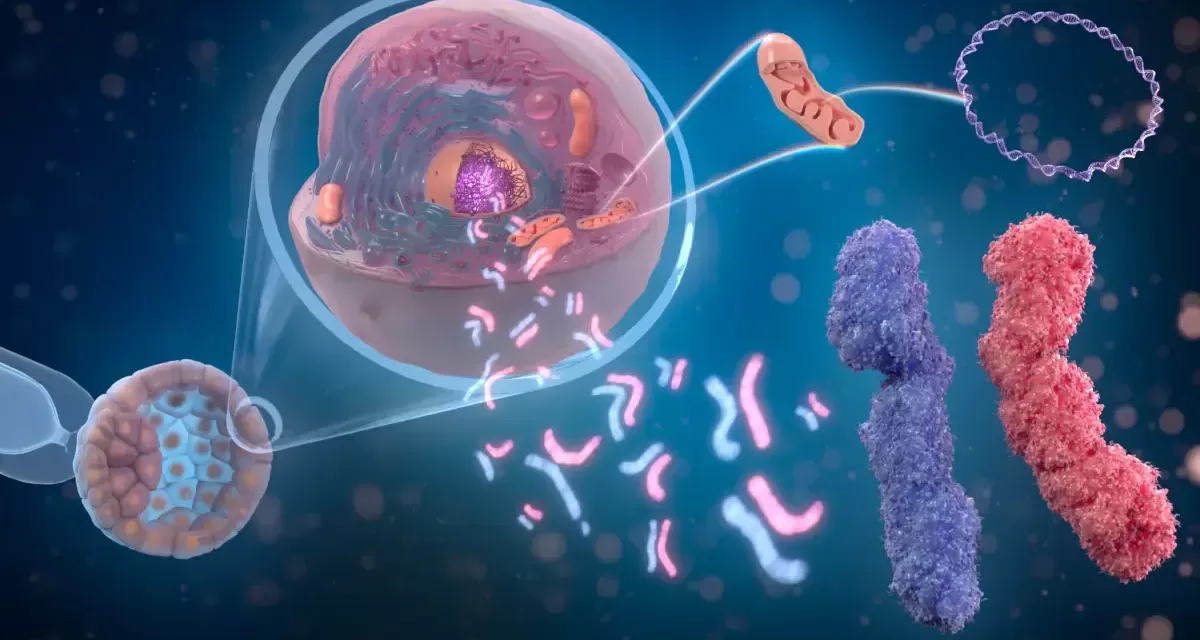
For decades, scientists have known that Trypanosoma brucei is a master of disguise. The parasite, which is transmitted through the bite of the tsetse fly in sub-Saharan Africa, lives in the bloodstream and is covered by a dense “coat” of Variant Surface Glycoproteins (VSGs).
When the human immune system recognizes a specific VSG coat, it produces antibodies to destroy the invaders. However, just as the immune system begins to win the battle, a small sub-population of parasites “switches” its coat to a different VSG type. The immune system, blindsided by this new appearance, must start the recognition process all over again.
The new research, published in the journal Nature, pinpoints exactly how this switch is initiated. Led by George A.M. Cross, head of the Laboratory of Molecular Parasitology at Rockefeller, the team discovered that the parasite doesn’t wait for a random mutation. Instead, it actively cleaves both strands of its DNA at a specific site upstream of the active VSG gene.
“This reveals how the parasite initiates its getaway by cleaving both strands of its DNA,” says Dr. Cross. This self-inflicted damage serves as a biological signal to the cell’s repair machinery to replace the current gene with a different one from a library of over 1,000 silent VSG genes.
Breaking the Code: A 250-Fold Advantage
To prove that DNA breaks were the primary driver of this evasion, the Rockefeller team—including researchers from the Laboratory of Cell Biology—utilized a specialized DNA-cleaving enzyme from yeast. By introducing this enzyme into the parasite, they could simulate the natural break and observe the results.
The findings were staggering. When the DNA was intentionally broken, the frequency of “coat-switching” jumped by 250 times compared to spontaneous switching rates. This mechanism ensures that even in a massive population of parasites, enough individuals will successfully change their appearance to maintain a persistent, chronic infection.
“The 250-fold increase in switching via targeted breaks underscores evolutionary ingenuity,” notes Dr. Roberto Docampo, a parasitologist at the University of Georgia who was not involved in the study. “However, it also reveals a potential vulnerability for drug design.”
Public Health Implications: The Toll of Sleeping Sickness
African sleeping sickness, or Human African Trypanosomiasis (HAT), remains a significant public health challenge. While World Health Organization (WHO) initiatives have reduced cases by 97% since 2000 through rigorous surveillance and vector control, an estimated 50 to 70 million people remain at risk.
The disease typically progresses in two stages:
-
The Hemolymphatic Stage: Parasites multiply in subcutaneous tissues, blood, and lymph. Patients experience fever, headaches, and joint pain.
-
The Meningoencephalitic Stage: The parasite crosses the blood-brain barrier. This leads to the disease’s namesake symptom—disturbed sleep patterns—along with confusion, tremors, and eventually coma or death.
Current treatments are often difficult to administer. “Current drugs like melarsoprol are toxic, with high encephalopathy risk,” says Dr. F. Nina Papavasiliou, a collaborator on the study from Rockefeller’s Laboratory of Cellular and Structural Biology. “Understanding this DNA break mechanism could target therapies to block recombination, essentially trapping the parasite in one coat so the immune system can finish the job.”
Expert Perspectives and Future Challenges
The discovery has been met with excitement from the global parasitology community, though experts urge a balanced view of the timeline for new treatments.
Dr. David Horn of the University of Dundee, an expert in trypanosome genetic switches, believes this work is foundational. “This work advances our grasp of random genetic switches enabling immune escape in parasites like trypanosomes and malaria. It provides a blueprint for how complex organisms manage survival in hostile environments.”
However, translating this “gene-shredding” insight into a pill or injection is a long-term goal. The study primarily utilized in vitro (laboratory) models. Researchers still need to validate these mechanisms in vivo—within the tsetse fly and mammalian hosts—to ensure the process behaves identically in a natural environment. Furthermore, with the advent of newer tools like CRISPR-Cas9, scientists may soon be able to refine these 2009 findings to see if other, more subtle genetic triggers are also at play.
What This Means for Global Health
For travelers and aid workers in endemic regions, the primary defense remains prevention—using insect repellent, wearing protective clothing, and avoiding tsetse fly habitats. For the scientific community, the focus shifts toward “trapping” the parasite. If a drug can be developed to inhibit the specific enzymes the parasite uses to repair its DNA during a switch, the parasite would be stuck with its “old” coat, making it an easy target for a healthy immune system.
As we move toward the goal of eliminating sleeping sickness by 2030, understanding the “how” behind the parasite’s survival is the first step toward making its “disappearing act” a thing of the past.
References
- https://scitechdaily.com/this-deadly-parasite-stays-invisible-by-shredding-its-own-genes/
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.