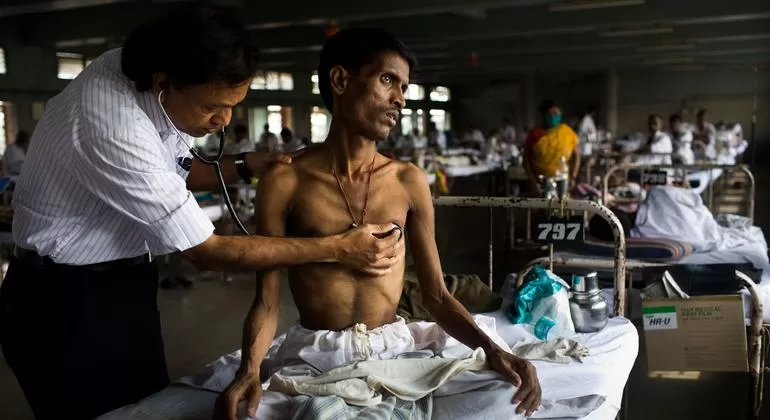
NEW DELHI — In a landmark shift for global health strategy, new research suggests that the most potent weapon against India’s tuberculosis (TB) epidemic might not be found only in a pharmacy, but in the pantry. A comprehensive modelling study published in The Lancet Global Health reveals that providing consistent nutritional support to TB patients across India could prevent approximately 120,000 deaths every year. This finding underscores a growing medical consensus: in the fight against TB, food is medicine.
The study comes at a critical juncture for India, which currently bears 26% of the world’s tuberculosis burden. By scaling up nutritional care to reach all 2.8 million TB patients in the country, public health experts believe the nation can achieve a massive reduction in mortality, illness, and community transmission.
The Weight of the Evidence: Key Findings
Tuberculosis has long been recognized as a “disease of poverty,” but the biological link between hunger and the bacteria Mycobacterium tuberculosis is now being quantified with surgical precision.
The latest modelling, led by researchers including C. Finn McQuaid and colleagues, indicates that undernutrition is perhaps the single greatest driver of the TB epidemic in India. According to the data:
-
Mortality: Universal nutritional support could save 120,000 lives annually.
-
Incidence: Proper nutrition for household contacts of TB patients could significantly reduce the number of new cases.
-
Global Context: With 10.8 million TB episodes globally in 2023, India’s 2.8 million cases represent a demographic where even modest nutritional gains yield exponential public health rewards.
“We have spent decades focusing almost exclusively on better diagnostics and faster drug regimens,” says Dr. Ananya Sharma, a public health consultant not involved in the study. “While those are vital, this research proves that if a patient is starving, the best drugs in the world face an uphill battle. You cannot heal a body that lacks the fuel to rebuild its immune system.”
Why Nutrition is a Clinical Necessity
The relationship between Body Mass Index (BMI) and TB risk is “log-linear,” meaning as BMI drops, the risk of developing active TB rises sharply.
When a person is undernourished, their immune system—specifically the T-cells responsible for sequestering TB bacteria—weakens. This allows a latent infection to become active or a new infection to take hold more easily.
The “RATIONS” Reality
The modelling study’s projections are anchored by real-world data from the RATIONS trial in Jharkhand. This field-based study showed that providing food rations and micronutrients to the household members of TB patients reduced the risk of them contracting the disease by nearly 39% to 48%.
For patients already diagnosed, the trial found that severe undernutrition at the start of treatment was a primary predictor of death. Conversely, those who were able to gain weight during their treatment cycle showed significantly higher survival rates and lower rates of relapse.
Moving Beyond the Clinic: Policy and Practice
India’s National Strategic Plan for TB has already begun integrating these insights. Current guidance supports “Nikshay Poshan Yojana,” a direct benefit transfer scheme that provides financial incentives for nutritional support. However, experts argue that the shift must move toward physical “food baskets” and community-based support.
“The goal is to treat the household, not just the patient,” notes the Ministry’s technical guidance. This involves:
-
Nutritional Screening: Assessing the BMI of every patient at the time of diagnosis.
-
Counselling: Educating families on high-protein, calorie-dense diets.
-
Direct Support: Providing rations like pulses, millets, and oil to ensure the financial incentive is translated into actual caloric intake.
Limitations and the “Modelling” Caveat
While the figure of 120,000 lives saved is a powerful motivator, researchers urge a balanced interpretation.
-
Assumption-Based: As a modelling study, these figures depend on “perfect world” scenarios where nutritional support reaches 100% of the population with high adherence.
-
The BMI Metric: Critics point out that BMI is a “blunt instrument.” A person might have a normal BMI but suffer from “hidden hunger”—severe micronutrient deficiencies in Vitamin A, D, or Zinc—which also impair immune function.
-
Implementation Gaps: In rural or highly impoverished areas, the logistics of delivering fresh, consistent food supplies remain a daunting challenge that models cannot fully account for.
What This Means for You
For the general public and those caring for loved ones with TB, the takeaway is clear: Nutrition is not an ‘extra’; it is a core component of the treatment.
-
For Patients: Focus on increasing protein intake and healthy fats. Weight gain during the first two months of treatment is a positive clinical sign.
-
For Families: If someone in your home has TB, the entire household is at risk. Ensuring everyone is well-nourished can act as a “biological shield” against the spread of the bacteria.
-
For Healthcare Providers: Nutrition status should be monitored as closely as sputum samples or X-rays.
As India pushes toward its ambitious goal of ending TB, the message from the scientific community is echoing louder than ever: to stop the bacteria, we must first feed the patient.
References
- https://health.economictimes.indiatimes.com/news/industry/nutritional-support-to-2-8-million-tb-patients-could-avert-120000-deaths-yearly-in-india-study/130825205?utm_source=top_story&utm_medium=homepage
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.