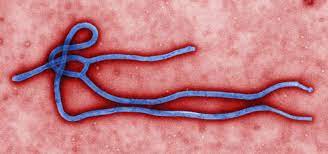
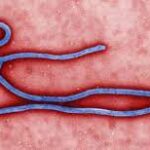
KINSHASA, Democratic Republic of the Congo — Health authorities in Africa have confirmed a new outbreak of Ebola virus disease in the eastern region of the Democratic Republic of the Congo (DRC). As of May 15, 2026, the Africa Centres for Disease Control and Prevention (Africa CDC) and local health ministries have reported 246 suspected cases and 65 deaths in Ituri province. The outbreak is currently concentrated in the Mongwalu and Rwampara health zones, with additional suspected cases under active investigation in the city of Bunia. In response to the rapid rise in cases, international health officials are moving swiftly to reinforce epidemiological surveillance across the DRC’s borders with Uganda and South Sudan to prevent regional transmission.
What Officials Know: Race to Identify the Strain
According to preliminary reports from the Africa CDC, initial laboratory testing detected the Ebola virus in 13 of 20 patient samples analyzed. Four of the recorded 65 deaths have been laboratory-confirmed.
In a rapid-response effort, the Africa CDC has convened emergency coordination meetings involving health officials from the DRC, Uganda, and South Sudan, alongside representatives from the World Health Organization (WHO) and international humanitarian partners.
A primary objective for laboratory investigators is characterizing the specific strain of the virus. Identifying the species of Ebola is critical because medical countermeasures, including vaccines and therapeutic treatments, vary significantly by strain.
The geographical location of the outbreak is causing particular concern among public health experts. Ituri province is characterized by porous borders, highly mobile populations, dense mining communities, and major trade routes. Officials warned that these factors, combined with localized insecurity and urban settings, could accelerate the spread of the virus. The current situation is viewed as a major test of regional outbreak readiness, highlighting how quickly Ebola can overwhelm fragile healthcare infrastructures when detection is delayed.
Why Ebola Matters: Transmission and Symptoms
Ebola virus disease is a severe, often fatal illness in humans. The virus is transmitted to people from wild animals and then spreads through human-to-human transmission via direct contact with:
-
Blood or bodily fluids (such as saliva, sweat, vomit, feces, and semen) of infected individuals.
-
Objects and surfaces (like bedding or clothing) contaminated with these fluids.
-
Burial practices that involve direct contact with the body of a deceased Ebola patient.
Key Fact: Individuals infected with Ebola do not transmit the virus before symptoms appear. However, once symptoms manifest, the risk of transmission increases sharply, particularly within households, poorly equipped healthcare facilities, and during traditional funeral practices.
According to the WHO, the illness typically begins with non-specific, flu-like symptoms, including:
-
Sudden fever and profound fatigue
-
Muscle pain and severe headache
-
Sore throat
As the disease progresses, patients may experience vomiting, diarrhea, abdominal pain, impaired kidney and liver function, and, in some cases, internal and external bleeding (e.g., oozing from the gums or blood in stools).
The Challenge of a Potential Non-Zaire Strain
Public health agencies emphasize that “Ebola” does not represent a single, uniform medical scenario. Disease severity and management depend heavily on the viral species involved, the speed of clinical intervention, and the robustness of the public health response.
Initial field reports suggest that a non-Zaire strain may be driving this outbreak, with preliminary data pointing toward Bundibugyo ebolavirus. This distinction carries significant implications for outbreak containment. The U.S. Centers for Disease Control and Prevention (CDC) notes that the most widely deployed vaccine in routine outbreak response, ERVEBO, specifically targets the Zaire species and does not provide protection against other species like Bundibugyo.
Strain Specifics and Clinical Treatment
The potential involvement of the Bundibugyo strain presents unique challenges because it has been documented only a few times since its discovery. Consequently, it lacks the standardized vaccine and targeted monoclonal antibody toolkits available for Zaire Ebola outbreaks.
Historical data from past outbreaks provide context on what clinicians might expect:
-
2007 Outbreak (Uganda): Research published on the initial Bundibugyo outbreak indicated a case fatality rate of approximately 32% to 40%.
-
2012 Outbreak (DRC): Subsequent evaluations confirmed similar mortality ranges, which, while lower than the 70% to 90% fatality rates sometimes seen in Zaire strain outbreaks, still represent a severe public health threat.
Despite the lack of a strain-specific vaccine, survival rates can be significantly improved through optimized supportive care. The WHO states that rapid fluid replacement (oral or intravenous rehydration) and the immediate treatment of specific symptoms greatly enhance recovery prospects across all Ebola species.
Commenting on the situation, Dr. Monica Gandhi, an infectious-disease specialist at the University of California, San Francisco (who was not involved in the field response), emphasized the broader strategy required:
“This outbreak underscores the absolute necessity of rigorous cross-border coordination. Because vaccine and treatment options are highly strain-specific, containment must rely heavily on classic epidemiological interventions.”
Dr. Gandhi’s perspective aligns with standard WHO guidelines, which dictate that controlling an outbreak relies on a multi-pronged approach: enhanced surveillance, meticulous contact tracing, strict infection prevention and control (IPC) in clinics, safe and dignified burials, reliable laboratory support, and deep community engagement.
+--------------------------+-----------------------+-------------------------+
| Ebola Species | Historical Fatality | Vaccine Availability |
+--------------------------+-----------------------+-------------------------+
| Zaire ebolavirus | Approx. 60% - 90% | Yes (ERVEBO) |
+--------------------------+-----------------------+-------------------------+
| Bundibugyo ebolavirus | Approx. 32% - 40% | No specific vaccine |
+--------------------------+-----------------------+-------------------------+
Public Health Impact and Long-Term Consequences
Currently, the immediate health risk is localized. It is highest for individuals living within the affected communities in Ituri, their close family contacts, and frontline healthcare workers who may lack adequate personal protective equipment (PPE). The U.S. CDC notes that filoviruses like Ebola pose minimal risk to international travelers or the general public outside the endemic zones, provided there is no direct contact with infectious bodily fluids.
However, epidemiologists look beyond immediate containment. Emerging research highlights the long-term public health burden face by survivors. A retrospective cohort study published in The Lancet Infectious Diseases tracked survivors of the 2007 Bundibugyo outbreak in Uganda. The study revealed that survivors experienced significantly higher long-term health complications compared to uninfected control groups, including:
-
Ocular complications (eye pain and visual blurring)
-
Hearing loss and tinnitus
-
Difficulty swallowing (dysphagia)
-
Chronic joint and muscle pain
-
Persistent sleep disturbances and memory limitations
These findings indicate that the medical response to an Ebola outbreak cannot end when transmission stops; public health systems must plan for long-term survivor support and follow-up care.
Uncertainties and Limitations in Early Reporting
Public health journalists and medical experts urge caution when interpreting early outbreak statistics. At this stage, many recorded figures represent “suspected” cases rather than laboratory-verified infections.
In fast-moving epidemiological situations, initial numbers frequently fluctuate as field teams reconcile data from remote health zones, conduct diagnostic PCR testing, and differentiate Ebola from more common febrile illnesses endemic to the region, such as malaria or typhoid fever. Furthermore, definitive genomic sequencing is still required to conclusively confirm whether Bundibugyo ebolavirus or another species is the primary causative agent.
Guidance for Communities and Health Workers
For the international public and individuals outside the immediate conflict-and-outbreak zones of the DRC, health authorities emphasize vigilance over panic.
For Travelers and the Public
If an individual has recently traveled to an Ebola-affected region and subsequently develops symptoms such as sudden fever, severe weakness, vomiting, or unexplained bleeding, they must seek immediate medical evaluation. It is vital to disclose their complete travel history to healthcare providers before or immediately upon arrival at a medical facility. The public is also advised to rely strictly on validated updates from official bodies like the WHO or local ministries of health to prevent the spread of misinformation regarding unverified treatments.
For Clinicians and Healthcare Providers
Medical personnel are urged to maintain a high index of suspicion for patients presenting with compatible symptoms and a history of travel to eastern DRC. The primary clinical directives include:
-
Immediate isolation of any suspected case.
-
Strict adherence to standard, contact, and droplet infection control precautions.
-
Use of appropriate personal protective equipment (PPE).
-
Rapid notification of institutional infection control and public health authorities.
Effective outbreak management relies entirely on transparency, speed, and collaborative action among local communities, clinicians, and international public health networks.
References
- https://barlamantoday.com/2026/05/15/africa-cdc-confirms-ebola-outbreak-in-eastern-congo-65-deaths-reported/
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.