The World Health Organization (WHO) has expressed regret and “deep concern” after the United States formally completed its withdrawal from the UN health agency this week, ending a year‑long process that culminated on Thursday, 22 January 2026. The move by Washington, historically the WHO’s largest single donor, raises pressing questions about how global disease surveillance, pandemic preparedness, and health programs in low‑ and middle‑income countries will be financed and coordinated in the years ahead.
What happened and why it matters
In a joint statement from the U.S. Department of Health and Human Services and the State Department, officials confirmed that the United States has completed its withdrawal from WHO, citing what they described as the organization’s “mishandling” of the COVID‑19 pandemic and its failure to address calls for governance reforms and political independence. The notification of withdrawal had been lodged a year earlier, in January 2025, with the formal exit taking effect after the required 12‑month notice period and the settlement of outstanding financial obligations.
WHO, in an official statement, said it “regrets” the U.S. decision and warned that it will make “both the United States and the world less safe,” emphasizing that infectious diseases do not respect borders and that coordinated global action is essential for rapid detection and response. This is the first time since WHO’s founding in 1948 that the United States has not been a member, underscoring the significance of the break and the uncertainty surrounding future U.S. engagement with multilateral health initiatives.
WHO’s response and ongoing roles
WHO leaders have defended the agency’s record during the COVID‑19 pandemic, describing it as an “unprecedented global health crisis” in which technical guidance, emergency operations, and surveillance systems “before, during and after the emergency phase” contributed to keeping all countries safer, including the U.S. itself. In its statement on the withdrawal, WHO said the issues raised by Washington will be discussed by the Executive Board in early February and by the World Health Assembly at its annual meeting in May 2026, signaling that member states may revisit governance and financing arrangements.
Despite the U.S. exit, WHO has stressed that its core functions—such as coordinating responses to outbreaks, maintaining global disease surveillance networks, developing health norms and standards, and supporting national health systems—will continue. However, the agency acknowledged that the loss of one of its primary funders will intensify pre‑existing financial pressures and could force further prioritization or scaling back of certain programs.
The funding gap: how big is the hole?
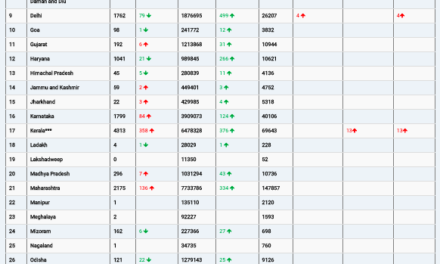
The United States has long been one of WHO’s largest financial contributors, providing both mandatory “assessed” contributions (membership dues) and substantial “voluntary” funding targeted to specific programs such as polio eradication, health emergencies, and disease‑specific initiatives. For the 2022–2023 budget cycle, U.S. contributions totaled about 1.28 billion dollars, roughly 12 percent of WHO’s approved budget and around 15 percent of funds actually received when accounting for shortfalls. In the 2024–2025 period, U.S. support amounted to approximately 958.5 million dollars, the majority of it in voluntary contributions, representing about 14 percent of WHO’s programme budget up to late 2024.
WHO’s overall 2024–2025 programme budget stands at about 6.83 billion dollars, of which only around 16.8 percent comes from assessed contributions, with the rest dependent on voluntary and often earmarked funding from member states and philanthropic organizations. Analysts warn that abruptly removing U.S. funds from this already fragile mix could trigger a “financial crisis” for the agency, forcing cuts to technical staff, emergency operations, and country‑level support, especially in low‑resource settings that rely heavily on WHO expertise and logistics. As one global health economist not involved with WHO policy debates might put it, losing a donor of this scale is like “pulling a major pillar out of a shaky building—the structure may still stand, but only after painful and risky re‑engineering.”
U.S. government rationale and criticisms of WHO
U.S. officials have framed the withdrawal as a necessary step to protect American interests and taxpayer funds. In their 2026 statement, health and foreign policy leaders argued that WHO failed to adequately investigate the origins of COVID‑19, did not act quickly enough in the early stages of the outbreak, and has been overly influenced by certain member states, particularly China. They also criticized what they described as WHO’s “unfairly onerous” financial demands on the United States compared with other large economies.
These positions build on earlier political critiques that the agency was “too China‑centric” during the pandemic and insufficiently transparent, echoing long‑standing debates about how much power member states wield over WHO’s decisions. Supporters of the withdrawal argue that the U.S. can redirect resources into bilateral health agreements, regional partnerships, and domestic public health infrastructure, claiming that this could yield more control and accountability over how funds are used. However, independent experts caution that bilateral projects, while valuable, cannot easily replace WHO’s unique role in coordinating global surveillance, issuing technical norms, and convening countries during emergencies.
How this could affect global health programs
The potential consequences of the U.S. exit extend far beyond Geneva meeting rooms, with implications across multiple health areas:
-
Disease surveillance and early warning: WHO hosts global alert systems that track emerging threats—from novel influenza strains to viral hemorrhagic fevers—by aggregating data from member states and partner labs. Reduced funding could slow data analysis, technical support, or field investigations, potentially delaying responses to future outbreaks.
-
Immunization and eradication efforts: U.S. voluntary contributions have supported WHO’s work in polio eradication, measles control, and routine immunization campaigns in low‑income countries. Funding cuts could force program consolidation or fewer vaccination drives, which may increase the risk of preventable disease outbreaks, especially in regions with fragile health systems.
-
Health emergencies and humanitarian crises: WHO’s Health Emergencies Programme coordinates responses to conflicts, natural disasters, and epidemics, including deploying rapid‑response teams, delivering medical supplies, and issuing clinical guidance. A smaller budget may limit surge capacity or prolong response times, affecting vulnerable populations in conflict zones or disaster‑affected areas.
-
Technical guidance and standard‑setting: From essential medicines lists to infection‑prevention protocols, WHO provides evidence‑based guidance that many countries, especially those with limited regulatory capacity, adopt as national standards. Budget stress could reduce the speed or breadth of guideline updates, including in areas such as antimicrobial resistance, non‑communicable diseases, and maternal health.
A senior infectious disease specialist at a major academic medical center, who is not affiliated with WHO, might summarize the risk for clinicians this way: “If surveillance weakens anywhere, clinicians everywhere eventually feel the impact—in the form of delayed alerts, slower guideline updates, or vaccines and treatments that reach our patients later than they should.”
What it means for patients and the general public
For most individuals, the effects of the U.S. withdrawal are unlikely to be immediate in day‑to‑day healthcare, but the decision could influence longer‑term health risks and access to services. People living in countries that rely heavily on WHO‑supported programs—for example, immunization campaigns, tuberculosis control, or maternal health initiatives—may be at higher risk if funding gaps are not filled by other donors or domestic budgets.
In high‑income countries, including the U.S., the impact will likely be more subtle, such as changes in how rapidly new outbreaks are detected abroad, how quickly global travel advisories are issued, or how smoothly international clinical trial coordination occurs during emergencies. For health‑conscious readers, global health governance can feel distant, but it underpins familiar aspects of daily life—from the safety of vaccines to the speed of travel‑related health alerts on diseases like Zika, Ebola, or new respiratory viruses.
Public health experts generally emphasize that individual preventive actions remain crucial regardless of geopolitical decisions. This includes staying up to date with recommended vaccinations, following evidence‑based guidance on infection prevention (such as hand hygiene and respiratory etiquette), managing chronic conditions like diabetes or hypertension with regular medical follow‑up, and seeking reliable information from trusted sources like national health ministries, recognized medical societies, and peer‑reviewed journals.
Limitations, uncertainty, and what comes next
Several uncertainties surround the U.S.–WHO split. First, while WHO has warned of increased risk to global health security, the exact impact will depend on how quickly other member states, philanthropic organizations, or regional bodies step in to close funding gaps and share technical responsibilities. Second, the United States has indicated it will pursue alternative forms of international cooperation, but details on which programs will be expanded or created—and how they will interact with existing WHO‑led initiatives—remain limited.
There is also political uncertainty: future U.S. administrations or Congress could revisit the decision, potentially seeking re‑entry or new forms of association, as has occurred in the past with other international agreements. WHO’s governing bodies will now examine the legal and operational implications of losing a founding member that had negotiated a special withdrawal clause when joining, including how to manage the transition and whether to seek changes in the agency’s constitution to reduce future vulnerabilities.
Finally, experts highlight that both criticism and defense of WHO often conflate two issues: the agency’s performance during a once‑in‑a‑century pandemic, and deeper structural constraints such as limited funding, complex governance, and heavy reliance on earmarked voluntary contributions. As one global health policy scholar might note, “We should distinguish between fixing what went wrong in COVID‑19 and weakening the very institutions we need to respond better next time.”
For readers, the key takeaway is that global health decisions made at the diplomatic level can eventually shape local health policies, clinical practice, and access to essential services—even if those effects are not immediately visible. Staying informed through credible sources, supporting evidence‑based public health measures, and engaging constructively with discussions about global cooperation can help ensure that health security remains a shared priority across borders.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Reuters. “World Health Organization says it regrets US decision to withdraw.” 24 January 2026.theprint+2