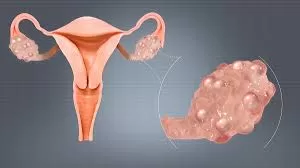
Polycystic Ovary Syndrome (PCOS), widely known for its physical symptoms like irregular menstrual cycles, weight gain, and infertility, has been increasingly recognized as a significant factor affecting mental health in women. Recent research reveals that women with PCOS are two to three times more likely to experience anxiety, depression, and body image disturbances compared to those without the syndrome. These findings underscore the vital need for a holistic approach to PCOS that addresses both physical and psychological well-being.
Rising Mental Health Challenges Among Women with PCOS
A recent meta-analysis published in Human Reproduction Update highlights that nearly 40% of women with PCOS endure significant depressive episodes, while over 30% have an anxiety diagnosis. Another cross-sectional study involving PCOS patients found that approximately 47.7% exhibited symptoms of depression and 39.9% showed signs of anxiety — significantly higher than in control groups without PCOS. Mild to severe forms of depression and anxiety were documented among these women, indicating a widespread mental health burden.
The increased prevalence of these mental health disorders among women with PCOS aligns with findings from several international studies. For example, data from a large Korean population study suggested that PCOS patients have a higher risk of depressive, bipolar, anxiety, and sleep disorders compared to controls, reinforcing the link between PCOS and psychiatric conditions. Similarly, a 2025 study on mood disorders in women with PCOS reported elevated psychological symptoms, including somatization and heightened perceived stress, compared with women without the condition.
Biological and Psychosocial Contributors
The interplay between hormonal imbalances and mental health in PCOS is complex. Elevated androgens and insulin resistance—hallmark features of PCOS—are implicated in disrupting neurotransmitter regulation, which governs mood and emotional well-being. This biochemical disruption may partly explain the increased susceptibility to anxiety and depression.
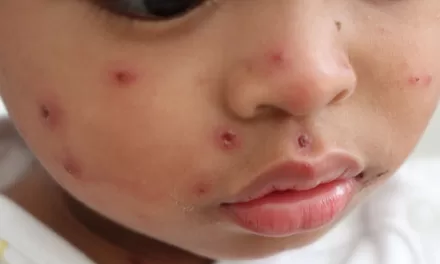
Moreover, the physical manifestations of PCOS, such as acne, hirsutism (excessive hair growth), obesity, and infertility, heavily impact body image and self-esteem, further escalating psychological distress. Societal pressures and stigma related to these visible symptoms and fertility challenges often compound feelings of anxiety and depression, creating a vicious cycle of emotional and physical health struggles.
Expert Insights
Dr. Pooja Wadhawan, a gynecologist specializing in PCOS management, notes, “Anxiety, stress, depression, and low self-esteem are quite prevalent among women with PCOS. Concerns about fertility, body image, and long-term health risks place a heavy emotional burden on patients.” She emphasizes that mental well-being is integral to effective PCOS management, advocating for multidisciplinary care that combines medical treatment with psychological support.
Psychiatrist Dr. Anita Desai adds, “Mental health disorders in PCOS are often under-recognized. Screening for anxiety and depression should be a routine part of care, as addressing these can significantly improve patient outcomes and quality of life.” She recommends integrating lifestyle modifications with counseling and, when necessary, pharmacotherapy to manage both PCOS symptoms and associated mental health conditions.
Implications for Public Health and Patient Care
The high incidence of anxiety and depression among women with PCOS indicates a pressing public health concern that transcends the traditional focus on reproductive and metabolic issues. Healthcare providers must adopt an integrated approach to screening and treatment that includes mental health as a core component.
Lifestyle interventions—including a balanced diet, regular exercise, and quality sleep—have demonstrated benefits not only in improving metabolic health but also in alleviating symptoms of anxiety and depression. Psychological strategies such as mindfulness, journaling, and stress management programs contribute to enhancing emotional resilience in affected women.
Routine psychological assessment using validated tools like the Generalized Anxiety Disorder 7-item scale (GAD-7) and Patient Health Questionnaire-9 (PHQ-9) is recommended to identify mental health needs promptly. Collaboration between gynecologists, endocrinologists, psychiatrists, and psychologists ensures comprehensive care tailored to individual patient profiles.
Limitations and Need for Further Research
While the association between PCOS and mental health disorders is well-supported, the precise biological mechanisms remain incompletely understood. Many studies are cross-sectional, limiting causal inference. Additionally, cultural, socioeconomic, and environmental factors vary widely and may influence the psychological experience of PCOS differently across populations.
Further longitudinal and mechanistic research is essential to unravel the pathways linking endocrine dysfunction in PCOS with mood disorders. This will aid in developing targeted treatments that address both reproductive and mental health simultaneously.
Practical Takeaways for Readers
Women diagnosed with PCOS should be aware that experiences of anxiety and depression are common and not a sign of personal weakness or failure. Seeking mental health support alongside medical treatment for PCOS can greatly enhance life quality. Health professionals advise open communication about emotional symptoms and encourage proactive lifestyle changes that support overall well-being.
Social support systems, education about PCOS, and reducing stigma around both hormonal disorders and mental health can empower women to manage their condition holistically and effectively.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References