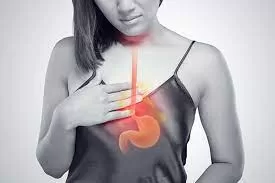
A large Nordic population-based study published in 2025 has found that menopausal hormone therapy (MHT) is associated with an up to 30% lower risk of developing cancers of the upper gastrointestinal (GI) tract, specifically esophageal and gastric cancers, in postmenopausal women compared to those not using MHT. This significant reduction in cancer risk was most notable for the combined estrogen-progestin formulations and systemic types of MHT.
Key Study Findings
The study, presented by Dr. Victoria Wocalewski from Karolinska Institutet at United European Gastroenterology Week 2025, analyzed data across five Nordic countries. It showed a clear inverse association between MHT use and the risk of esophago-gastric cancers, particularly esophageal adenocarcinoma (EAC) and gastric adenocarcinoma (GAC). Women using any form of MHT had significantly reduced odds of developing these cancers, with adjusted odds ratios (aORs) around 0.68 to 0.74 for esophageal adenocarcinoma depending on hormone dose, indicating a 26–32% decreased risk. Combined estrogen-progestin therapy appeared more protective than estrogen alone. However, there was no significant reduction for esophageal squamous cell carcinoma (ESCC).
Dose-response relationships emerged, suggesting higher daily doses and longer duration of MHT further decreased risk. The associations held even after adjusting for known confounders such as age, obesity, smoking, alcohol use, reflux disease, Helicobacter pylori eradication treatment, and use of statins or anti-inflammatory medications. The study did not adjust for socioeconomic factors.
Expert Commentary and Context
Dr. Jan Bornschein, University of Oxford, who was not involved in the study, underscored its relevance: “We’ve seen for a long time a link between hormones and gastrointestinal (GI) pathology, but it has been poorly investigated until now. This structured, large-scale study advances understanding significantly.”
These findings complement previous research indicating hormonal factors influence GI cancer risk and may partly explain why these cancers are more common in men than women. The protective mechanism is hypothesized to involve estrogenic signaling’s effect on epithelial tight junctions and nitric oxide synthesis in the GI tract, which may affect cellular environments and smooth muscle biology.
A systematic review and meta-analysis from 2022, including nearly 2 million women, also found that hormone replacement therapy—including both estrogen-only and combined estrogen-progestin formulations—was associated with approximately a 28% lower risk of gastric cancer. This supports the current study’s population-based findings. However, given that MHT is primarily prescribed to manage menopausal symptoms, these findings do not establish MHT as a preventive therapy for GI cancers due to the complex risk-benefit profile of hormone use, including risks related to breast cancer, cardiovascular disease, and thrombosis.
Implications for Public Health
Given that stomach and esophageal cancers are significant causes of cancer morbidity worldwide, identifying modifiable risk factors is important. These findings provide new insight into how menopausal hormones influence upper GI cancer risk and highlight a potential protective role.
Women considering MHT should discuss personalized risks and benefits with their healthcare providers, balancing menopausal symptom relief with known hormone therapy risks. Awareness of hormonal impact on GI cancer risk may also inform risk stratification and prevention strategies in postmenopausal women.
Limitations and Balanced Perspective
The Nordic study did not account for socioeconomic status, which may influence cancer risk and hormone therapy use patterns. Observational data cannot prove causation and residual confounding cannot be excluded. The effect was not observed for all esophageal cancer subtypes, and further mechanistic research is needed to clarify hormonal pathways involved. Additionally, hormone therapy’s adverse effects, particularly increased breast cancer risk with combined therapy and cardiovascular risks in certain populations, remain important considerations.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: