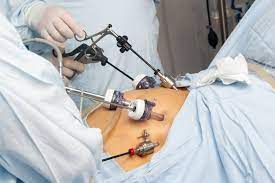
For the millions of adults living with the dual burden of obesity and type 2 diabetes (T2D), the clinical path forward has long been a choice between intensive lifestyle and medical management or the more invasive route of metabolic surgery. While short-term successes are common in both, a new long-term study published in the International Journal of Obesity has provided definitive evidence that surgery offers a superior, sustained advantage in both weight reduction and blood sugar control.
The retrospective cohort study, which tracked patients over a five-year period, reveals that metabolic bariatric surgery isn’t just about aesthetic changes; it acts as a potent tool for metabolic “resetting.” The findings suggest that for many, surgery may be the most effective intervention available to prevent the long-term complications of diabetes.
The Weight of the Evidence: A Five-Year Comparison
Researchers analyzed data from 411 adults referred for bariatric surgery at a major hospital in West Scotland between 2009 and 2020. The cohort was divided into two groups: 186 individuals who underwent surgery and 225 who remained in non-surgical care, receiving standard medical therapy and lifestyle interventions.
The results at the five-year mark were stark. Nearly 38% of all patients in the study achieved a total weight loss (TWL) of at least 20%. However, of those who hit this significant milestone, a staggering 87.2% were from the surgical group.
“What we are seeing is a divergence in long-term outcomes,” says Dr. Elena Rossi, an endocrinologist not involved in the study. “In traditional medical management, we often see a ‘U-shaped’ curve where weight is lost initially but slowly creeps back. Surgery appears to fundamentally alter the body’s weight set-point in a way that medication alone rarely achieves.”
Mastering the A1c: Glycemic Control and Remission
While weight loss is the most visible outcome, the impact on blood sugar—measured by the A1c test—is arguably more critical for long-term health. The A1c test provides a three-month average of blood sugar levels; a level below 6.5% is typically the threshold for a diabetes diagnosis, while below 6.0% is considered the “normal” or “pre-diabetes” range.
The study found a dramatic difference in glycemic success:
-
42.5% of surgical patients achieved an A1c of less than 6.0% at five years.
-
Only 7.8% of non-surgical patients reached that same level.
These numbers suggest that surgery can lead to what clinicians call “remission”—a state where blood sugar levels are in the non-diabetic range without the need for active pharmacological intervention.
“Diabetes is a progressive disease,” explains Dr. Marcus Thorne, a metabolic health researcher. “The fact that nearly half of the surgical group maintained near-normal A1c levels after five years is a testament to the hormonal shifts surgery triggers. It’s not just about eating less; it’s about how the gut communicates with the brain and pancreas.”
Public Health Implications: A Shift in Treatment Philosophy?
For years, bariatric surgery was viewed as a “last resort” for those who had failed all other options. However, these findings, alongside recent updates to the American Diabetes Association (ADA) and International Diabetes Federation (IDF) guidelines, suggest surgery should be considered much earlier in the treatment algorithm for patients with a BMI over 30 who cannot achieve glycemic targets.
The public health stakes are high. Type 2 diabetes is a leading cause of kidney failure, blindness, and cardiovascular disease. By achieving sustained weight loss and A1c reduction, patients significantly lower their risk of these life-altering complications.
Challenges and Considerations
Despite the clear benefits, surgery is not a “magic bullet.” The study authors and independent experts highlight several nuances:
-
Accessibility: Not all patients have equal access to surgical centers or insurance coverage for these procedures.
-
Lifelong Commitment: Surgery requires a permanent change in eating habits and lifelong vitamin supplementation to prevent nutritional deficiencies.
-
The Rise of GLP-1s: It is important to note that this study spanned 2009-2020. This was largely before the widespread use of highly effective new medications like semaglutide (Ozempic/Wegovy) and tirzepatide (Mounjaro/Zepbound). Future studies will need to compare surgery against these “next-generation” medical therapies.
Limitations to the Research
As a retrospective cohort study, this research looked back at existing data rather than randomly assigning patients to groups (as a randomized controlled trial would). This means there may be “selection bias”—patients who chose surgery might have been more motivated or had different baseline health characteristics than those who didn’t.
Additionally, the study focused on a specific population in Scotland. While the biological mechanisms are universal, socioeconomic factors and healthcare delivery systems vary by region, which could influence long-term adherence and support.
What This Means for You
If you are living with obesity and type 2 diabetes, this study underscores that “standard care” may not always be enough to halt the progression of the disease.
Key Takeaways for Patients:
-
Earlier Intervention Matters: Discussing metabolic surgery early in your diagnosis—rather than waiting for complications—may lead to better long-term outcomes.
-
Holistic Success: Success isn’t just about the number on the scale; it’s about the reduction of medication and the stabilization of blood sugar.
-
Consult the Experts: Every patient’s biology is different. A multidisciplinary team including a primary care doctor, an endocrinologist, and a bariatric surgeon is essential to determine the right path.
The conversation around diabetes is changing. It is moving away from simply “managing” a chronic condition toward the active pursuit of metabolic health and remission.
References
- https://www.emedinexus.com/post/53856/Bariatric-Surgery-Outperforms-Medical-Therapy-for-Weight-and-A1c-Reduction
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.