A groundbreaking study from Stanford Medicine reveals why wounds on the face and scalp often heal with minimal scarring compared to other body areas, pointing to differences in fibroblast origins and a protein called ROBO2. Published January 21, 2026, in Cell, the research used mouse models to identify a signaling pathway that could inspire new anti-scarring therapies, potentially benefiting surgery patients and those with internal fibrosis.
The Scarring Problem’s Hidden Toll
Scars form when the body prioritizes quick repair over perfect regeneration, depositing stiff collagen instead of flexible tissue. This process affects skin from surgery or injury but also drives deadly internal fibrosis; estimates link about 45% of U.S. deaths to fibrotic diseases like lung, liver, or heart scarring, though precise figures vary by condition. Scarred skin lacks hair follicles and sweat glands, impairing temperature regulation and strength, while hypertrophic scars complicate 32-72% of burn cases.
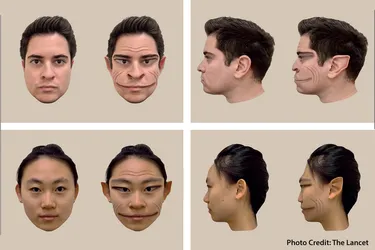
Clinicians have long observed that facial wounds scar less, likely because the face demands functional preservation for senses and eating, unlike body wounds focused on survival. This pattern hints at location-specific healing strategies rooted in embryonic development.
Study Design and Key Findings
Researchers wounded mice on the face, scalp, back, and abdomen, stabilizing sites with rings to mimic controlled conditions. After 14 days, facial and scalp wounds showed smaller scars and fewer fibrosis-linked proteins. Transplanting facial skin to mouse backs preserved low-scarring behavior, proving the effect ties to resident cells, not location.
Fibroblasts—collagen-producing cells—from facial skin, derived from neural crest cells, drove regenerative healing. Injecting just 10-15% facial-like fibroblasts into back wounds reduced scarring via a cascade effect. Single-cell RNA sequencing pinpointed ROBO2 overexpression in these fibroblasts, maintaining less-fibrotic states through quieter DNA transcription, resembling embryonic progenitors.
Blocking EP300, a gene-activating protein downstream of ROBO2, with existing small molecules mimicked facial healing in body wounds, restoring hair follicles and glands without delaying closure.
Expert Insights from the Research Team
“The face and scalp are developmentally unique,” said Dr. Derrick Wan, study co-author, noting neural crest origins enable regenerative paths. Dr. Michael Longaker emphasized survival trade-offs: “Injuries on the body must heal quickly… you will likely still survive.”
Dr. Dayan J. Li, a dermatologist on the team, highlighted minimal intervention’s power: “Changing just a few cells can trigger a cascade… even 10% to 15% of surrounding fibroblasts.” Longaker added that common mechanisms across tissues suggest broad applications.
Broader Context in Wound Healing
Fetal skin heals scarlessly via regeneration, but adult wounds shift to fibrosis around mid-gestation. Fibroblast diversity— papillary (regenerative) versus reticular (fibrotic)—further explains outcomes, with Engrailed-1 lineage fibroblasts fueling scars. Facial fibroblasts’ ROBO2-EID1-EP300 axis epigenetically silences pro-scarring genes.
Current scar management includes lasers, injectables, and silicone, but none reverse fibrosis fully. Hypertrophic scars affect 8-67% post-burn or surgery, with contractures in 38-54% at discharge.
Public Health Implications
This discovery could transform post-surgical care, reducing cosmetic and functional burdens for millions undergoing procedures yearly. EP300 inhibitors, in cancer trials, offer a fast-track to clinic via topical or injected forms. Beyond skin, targeting this pathway might treat organ fibrosis, a leading killer.
Patients could see less pain, better mobility, and restored skin functions like sweating. For burns or trauma survivors, scarless options mean fewer revisions—5-20% currently need them up to 10 years post-injury.
Limitations and Critical Perspectives
As a mouse study, translation to humans remains uncertain; rodent healing differs, lacking ideal scar models. Small wounds were tested; large or infected ones may vary. EP300’s cancer role demands safety checks for skin use.
No external expert quotes directly critiqued this work, but general reviews stress fibroblast therapies’ promise amid model gaps. Ongoing trials and human data are needed before claims of scarless healing.
Long-term, reprogramming fibroblasts embryonically could redefine repair, but ethical and practical hurdles loom.
References
-
Griffin MF, et al. Fibroblasts of disparate developmental origins harbor distinct fibrogenic potential. Cell. 2026 Jan 21. doi:10.1016/j.cell.2025.12.027.sciencedirect+1
-
Li DJ, et al. Stanford Medicine news release: The face scars less than the body. EurekAlert!/Stanford Medicine. 2026 Jan 21.eurekalert+1
-
Earth.com. Why some wounds heal without scars – and others don’t. 2026 Jan 25.[earth]
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidnce emerges.