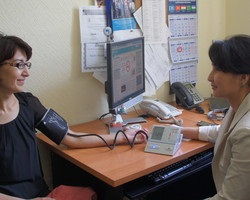
Recent research is challenging long-standing advice on the timing of blood pressure medication. For years, most patients and doctors have stuck to a morning routine—take your pill as soon as you wake up, and carry on with your day. The reasoning was simple: blood pressure often surges in the morning, so taking medication at that time seemed logical.
However, a wave of new studies is shifting the conversation. One notable Spanish study published in 2019 followed over 19,000 people with high blood pressure for an average of six years. The findings were striking: those who took their medication at bedtime had a 40% lower risk of heart attacks, a 34% lower risk of strokes, and a 66% lower risk of cardiovascular death compared to the morning group. These results suggest that nighttime dosing may help restore the natural nighttime dip in blood pressure, which is often absent in people with hypertension—especially older adults or those with diabetes.
Despite these promising results, not all research points in the same direction. A large 2022 study published in The Lancet, involving more than 21,000 participants, found little difference in outcomes between those taking their medication in the morning (between 6 a.m. and 10 a.m.) and those taking it at night (between 8 p.m. and midnight). The rates of stroke, heart attack, or vascular death were nearly identical in both groups (3.7% for morning, 3.4% for evening).
So, what should patients do? Experts emphasize that the best time to take your blood pressure medication depends on several factors:
-
Type of Medication: Some drugs, like diuretics (water pills), can increase nighttime bathroom trips and disrupt sleep if taken in the evening.
-
Your Body’s Pattern: If your blood pressure does not drop at night (a “non-dipping” pattern), nighttime dosing might be more beneficial.
-
Routine and Consistency: The most important factor is taking your medication consistently at a time that fits your lifestyle and minimizes side effects.
-
Multiple Medications: Sometimes, a split schedule—part in the morning, part at night—works best.
Key Takeaway
While recent studies suggest nighttime dosing may offer extra protection for some, the evidence is not one-size-fits-all. The best approach is to consult your doctor before changing your medication schedule, especially if you have kidney disease, diabetes, or a non-dipping blood pressure pattern. Above all, consistency is crucial—never skip doses, and always follow your healthcare provider’s advice.
Disclaimer:
The content in this article is intended for informational and educational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare provider before starting any diet, supplement, fitness, or health program, or before making changes to your medication schedule.