A growing body of medical research is prompting renewed consideration on whether dialysis is always the best option for older adults with kidney failure. While dialysis can extend life, emerging evidence suggests that for many older patients, particularly those with significant frailty and comorbidities, the modest survival benefits of dialysis may come at the cost of diminished quality of life and increased time spent in hospitals or care facilities. This understanding invites a more personalized decision-making process where patients, families, and clinicians weigh life expectancy against the burden of treatment and quality of remaining life.
The question at hand is whether older adults — especially those over 65 or 75 years old with advanced chronic kidney disease (CKD) or end-stage kidney disease (ESKD) — should always begin dialysis immediately upon reaching kidney failure, or if conservative management focusing on symptom relief and quality of life is sometimes preferable. This issue is particularly urgent as populations age globally, and more elderly individuals face kidney failure with limited eligibility for kidney transplantation due to age or other health conditions. New studies published in 2024-2025 highlight that while dialysis prolongs life, the margin may be minimal, and its side effects, lifestyle impact, and hospitalization rates are considerable.
Key Findings and Developments
Recent research led by Stanford Medicine analyzed health records of over 20,000 veterans aged 65 and older with kidney failure who were not candidates for transplantation. The study found that starting dialysis immediately prolonged survival by an average of nine days compared to delaying or foregoing dialysis; however, those patients also spent significantly more time — about two additional weeks — in hospitals or care facilities. Patients who chose to forgo dialysis died on average 77 days earlier but enjoyed more days at home rather than in institutional settings.
Older patients’ experience was mixed across age groups: those aged 65 to 79 who started dialysis immediately had fewer survival days and more inpatient days, while those over 80 saw a survival increase of about 60 days but still spent more time hospitalized. Experts caution that the quality of those extra days is equally important to consider.
A complementary 2024 study reported similar findings, noting that dialysis patients had only minimal longer survival (approximately 9 days) than those opting for conservative care emphasizing symptom management and emotional support. This research aligns with earlier qualitative studies showing many elderly patients may perceive their life as “complete” and prioritize quality and comfort over aggressive treatments.
Expert Perspectives
Dr. Manjula Tamura, a nephrology professor and senior author of the Stanford study, emphasized the importance of understanding the trade-offs dialysis entails for older adults and urged shared decision-making. “For some patients, dialysis is a blessing offering extended life; for others, it may be a burden that diminishes their remaining quality of life,” she said. Dr. Maria Montez Rath, a senior research engineer and the study’s lead author, questioned whether older adults desire to spend extended time receiving dialysis and hospital care instead of time at home.
Geriatric and palliative care specialists advocate framing dialysis decisions not solely around survival but encompassing broader goals including symptom control, daily functioning, and emotional well-being. They stress that older adults with multiple comorbidities and frailty may benefit from conservative management approaches that avoid dialysis while delivering compassionate symptom relief.
Context and Background
Kidney failure occurs when kidneys lose the ability to filter waste and fluids adequately, typically measured by estimated glomerular filtration rate (eGFR). Treatment options include kidney transplantation, dialysis, or supportive care without dialysis. Transplantation is generally considered the best solution but is often not feasible for older or frail patients with other illnesses.
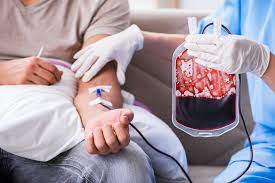
Dialysis treatments—whether hemodialysis in clinics or peritoneal dialysis at home—require significant time, can cause fatigue and cramping, and impose lifestyle changes such as frequent clinic visits or managing dialysis equipment. Older patients frequently report psychological and physical tolls, including loneliness, depression, and loss of independence.
Implications for Public Health and Patient Care
The expansion of dialysis to an aging population raises ethical and clinical challenges. Health systems must balance extending life with maintaining quality and dignity at older ages. Clinicians need to engage in individualized conversations with patients and families about realistic outcomes, personal values, and treatment preferences. These decisions should not be rushed but made with comprehensive information about survival benefits, potential hospitalizations, symptom burden, and lifestyle impacts.
Training healthcare providers in communication about end-of-life care and conservative kidney management is essential. From a public health perspective, supporting a range of care models, including palliative and home-based care options, will improve patient-centered care for older adults with kidney disease.
Limitations and Conflicting Viewpoints
While recent studies provide important insights, some limitations exist. Many studies rely on observational data, which may be subject to selection bias. Patient populations studied (e.g., veterans predominantly male) may limit generalizability. There is also variability in individual health status and goals that can influence outcomes and preferences.
Some clinicians and patients remain hopeful that dialysis can restore meaningful time and functionality even in later life, emphasizing that these decisions are deeply personal. The necessity of multidisciplinary care teams and ongoing reassessment, as health status changes, is widely acknowledged.
Conclusion
For older adults with kidney failure, dialysis is not always the unequivocal choice. Emerging evidence underscores the minimal survival benefit for some frail elderly patients compared to conservative care, and highlights the importance of balancing quantity of life with quality, time at home, and symptom control. Personal values, health status, and individual goals must guide treatment decisions, with healthcare providers playing a critical role in supporting informed, compassionate choices.
References
-
Moneta Rath M, Tamura M, et al. “Dialysis initiation and life expectancy in older adults with kidney failure.” Annals of Internal Medicine, 2024 Aug 19. DOI available on request.
-
Medscape. “When Ditching Dialysis Makes Sense for Older Adults,” 2025.
-
Singapore qualitative study on dialysis decision-making: [PMC: Opting out of dialysis – exploring patients’ decisions], 2013.
-
Academic OUP. “Smoothing transition to dialysis to improve early outcomes in older adults,” 2022.
-
Stanford Medicine News. “Dialysis may not be the best option for older adults,” 2024 Aug 18.
-
ScienceDirect. “Optimizing Care for Elderly Patients Failing to Thrive on Dialysis.”
-
ASN Online. “Dialysis Decisions in Elderly Patients with Advanced Kidney Disease.”
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.