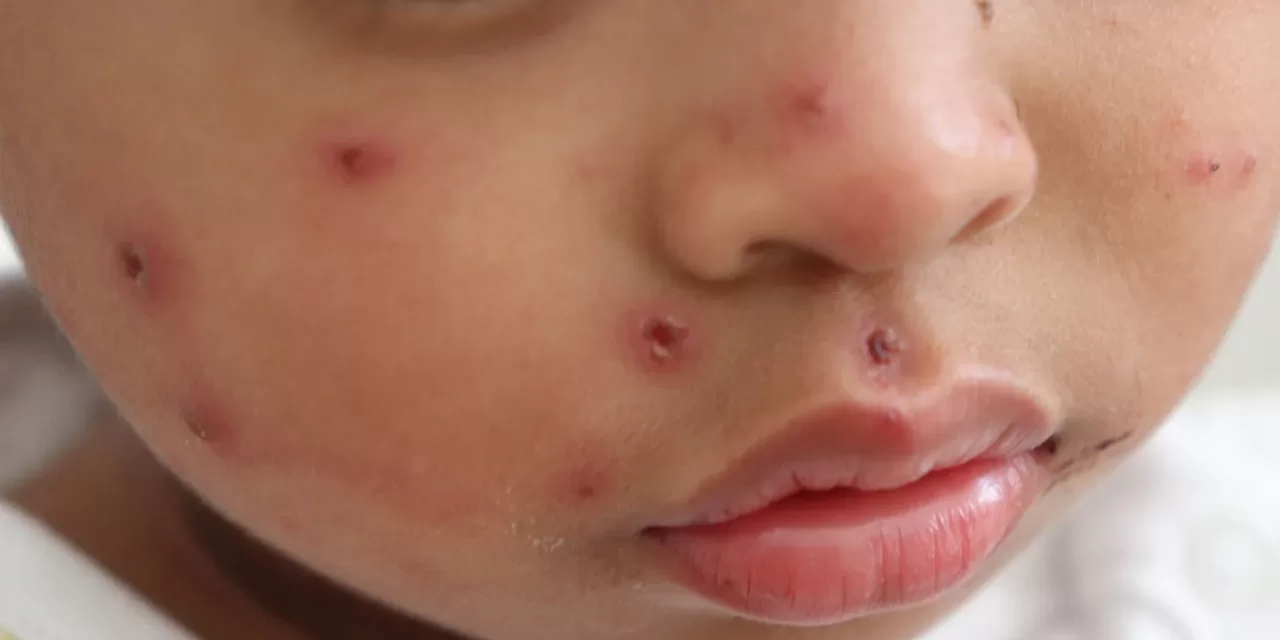
In 2025, the United States experiences its largest measles outbreak in over two decades, with more than 1,600 confirmed cases reported across 42 states by October 21. This resurgence, driven primarily by undervaccinated communities and vaccine hesitancy, has raised urgent concerns among health experts and authorities nationwide.
Key Findings and Developments:
This year, the U.S. has reported 1,618 confirmed measles cases, the highest in a single year since measles was declared eliminated nationally in 2000. The cases span 42 states, with notable outbreaks centered in Texas, New Mexico, Oklahoma, and South Carolina. Among these, 87% of the cases are linked to outbreaks—defined as clusters of three or more related infections—reflecting the contagious nature of measles spreading rapidly where vaccination rates are low.
Hospitalizations stand at 12% of all cases, indicating serious health impacts, including three confirmed deaths this year related to measles complications. Most cases (92%) occurred among individuals unvaccinated or with unknown vaccination status, highlighting vulnerability in these populations.
Expert Commentary:
Sharon Ward-Fore, a recognized expert in infectious diseases and the 2023 Educator of the Year by Infection Control Today, noted, “2025 has seen the most measles cases since measles was declared eradicated in the U.S. in 2000. Nearly all cases are among the unvaccinated or those with unknown immunization status. Measles is entirely preventable with vaccination”.
Heather Lanthorn, ScD, political and behavioral scientist at Duke Global Health Institute, linked the resurgence to rising public mistrust of vaccines and health authorities. “Where outbreaks occur is like forest fires: they ignite when there are ‘dry forests’—communities with insufficient vaccine coverage. This embers-on-the-wind effect explains why measles can rapidly spread in pockets of low immunity,” she explained.
The Global Virus Network also urged immediate action to reverse declining immunization rates, warning that falling vaccination coverage threatens to undo decades of progress against measles and other vaccine-preventable diseases.
Context and Background:
Measles, caused by the highly contagious rubeola virus, was declared eliminated in the U.S. in 2000 following widespread vaccination campaigns. However, the disease remains endemic globally, and international travel continues to introduce imported cases.
The current outbreak traces back to early 2025 when the virus was seeded in undervaccinated communities in West Texas, spreading quickly to neighboring states and beyond. Declining vaccine uptake — with kindergarten MMR (measles-mumps-rubella) coverage falling below the 95% herd immunity threshold to around 92.7% nationally — has created susceptible populations allowing rapid expansion.
Nonmedical vaccine exemptions have risen significantly in some areas; for example, Gaines County, Texas, saw conscientious exemptions increase from under 5% in 2015-16 to over 14% in 2024-25. This trend is part of a broader socio-behavioral pattern linked to misinformation, mistrust, and vaccine hesitancy.
Public Health Implications:
The resurgence serves as a critical warning about the consequences of declining vaccination coverage. Measles is one of the most contagious viruses known, with a basic reproduction number (R₀) between 12 and 18, meaning one infected person can infect 12-18 others in a susceptible population.
Efforts to increase MMR vaccination, prompt case isolation, and community engagement are essential to stopping outbreaks before they expand further. Public health campaigns aimed at educating about vaccine safety and encouraging timely immunization must be prioritized, especially in communities with low coverage.
Limitations and Counterarguments:
While the absolute number of cases remains low compared to pre-vaccine era millions of cases annually, the current increase signals vulnerability in immunity. Some experts highlight that vaccine hesitancy is multifactorial and that trust-building approaches coupled with equitable access to vaccines are crucial.
Also, reported cases may underestimate the true burden due to delays or gaps in case reporting. Surveillance is ongoing, and health agencies maintain real-time updates for public awareness and response coordination.
Practical Advice for Readers:
Individuals, particularly parents, are encouraged to verify their vaccination status and that of their children, ensuring they receive the recommended two doses of the MMR vaccine. Routine immunization remains the most effective protection against measles.
Healthcare providers should maintain high suspicion for measles in patients with rash and fever, report suspected cases immediately, and advocate vaccination in their communities.
Medical Disclaimer:
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References:
- https://www.cdc.gov/measles/data-research/index.html
- https://publichealth.jhu.edu/ivac/2025/us-measles-cases-hit-highest-level-since-declared-eliminated-in-2000