December 11, 2025
Cardiovascular disease often strikes without warning, but for the one in 250 people born with Familial Hypercholesterolemia (FH), the risk begins at birth. New data released this week highlights a critical failure in current detection methods, sparking an urgent push for universal pediatric lipid screening to prevent premature heart attacks and save lives.
For decades, the medical community has relied on a “targeted” approach to identifying high cholesterol in children—screening only those with a known family history of heart disease or visible risk factors like obesity. However, a landmark series of reports and guideline updates published in late 2025 suggests this strategy is leaving thousands of children vulnerable to a silent, genetic killer.
According to a new analysis referenced by Medscape Medical News and recent studies from the Mayo Clinic, current screening protocols miss nearly 90% of individuals with Familial Hypercholesterolemia (FH). With only about 10% of affected individuals currently diagnosed, experts are declaring a public health emergency, urging healthcare providers to adopt universal lipid screening for all children ages 9 to 11 and again at 17 to 21.
“We are essentially operating with a blindfold on,” says Dr. Niloy Jewel Samadder, a gastroenterologist and geneticist at the Mayo Clinic, whose recent study in Circulation: Genomic and Precision Medicine exposed the flaws in current detection criteria. “Our findings expose a massive blind spot in national guidelines. Relying on family history alone is a failed strategy because it assumes parents know they have high cholesterol or that a cardiovascular event has already occurred in the family. Too often, the first symptom of FH is a fatal heart attack in a young adult.”
The “Silent” Genetic Driver
Familial Hypercholesterolemia is the most common life-threatening genetic condition in the world, affecting approximately 1.3 million Americans. Unlike lifestyle-induced high cholesterol, FH is caused by a genetic mutation that impairs the body’s ability to clear low-density lipoprotein (LDL) cholesterol—often called “bad” cholesterol—from the bloodstream.
From day one, a child with FH has LDL levels two to three times higher than their peers. Over time, this cumulative burden damages arteries, leading to aggressive atherosclerosis (hardening of the arteries) in childhood and adolescence. Without treatment, men with FH have a 50% risk of having a heart attack by age 50, and women have a 30% risk by age 60.
“Think of it as a credit card debt that starts accumulating the moment you are born,” explains Dr. Sarah Jenkins, a pediatric cardiologist and preventive health advocate who was not involved in the new research. “By the time these patients reach their 30s, their arteries have been exposed to a level of cholesterol that a typical person wouldn’t see until their 60s or 70s. If we don’t catch it early, we lose the window of opportunity to prevent irreversible damage.”
The Case for Universal Screening
The renewed focus on screening comes on the heels of the Family Heart Foundation’s “LEAD” (Leveraging Evidence and Data) initiative, which has aggressively campaigned throughout 2024 and 2025 to dismantle barriers to diagnosis. Their data shows that despite guidelines from the National Heart, Lung, and Blood Institute (NHLBI) and the American Academy of Pediatrics (AAP) recommending universal screening, less than 20% of children in the U.S. actually undergo lipid testing.
The new consensus emerging in late 2025 reinforces that universal screening is the only way to catch these “invisible” patients.
“Targeted screening is failing because family history is often incomplete or unknown,” notes Dr. Laurence Sperling, Chief Medical Officer of the Family Heart Foundation and a professor in preventive cardiology at Emory University School of Medicine. In a recent statement regarding the LEAD initiative, Sperling emphasized that early diagnosis allows for “immediate and appropriate treatment,” potentially “saving hundreds of thousands of young lives from being cut short.”
The proposed screening schedule aligns with the AAP’s bright futures guidelines:
-
First Screen: Ages 9–11 (before puberty changes lipid levels).
-
Second Screen: Ages 17–21 (before young adulthood).
A simple blood test can reveal the hallmark signs of FH: LDL cholesterol levels above 190 mg/dL (or >160 mg/dL in children with a family history).
Safe, Effective Treatment Exists
One of the most compelling arguments for screening is the availability of safe, effective treatment. Statins, the cornerstone of FH management, have been proven safe for use in children as young as 8 to 10 years old.
“We have decades of data now showing that initiating statin therapy in childhood normalizes the risk of cardiovascular disease,” says Dr. Jenkins. “A child diagnosed with FH at age 10 who starts treatment can live a normal lifespan. That is a medical miracle that is currently being denied to 90% of the FH population simply because we aren’t testing them.”
Recent studies have also highlighted the psychological relief for families. A diagnosis often removes the “burden of guilt” associated with high cholesterol, helping patients understand that their condition is genetic and not solely the result of diet or exercise habits.
Barriers and Counterpoints
Despite the overwhelming evidence, barriers remain. The U.S. Preventive Services Task Force (USPSTF) has historically assigned an “I” rating (insufficient evidence) to universal childhood lipid screening, citing a lack of long-term randomized trials proving that childhood screening directly reduces adult heart attacks.
Critics of universal screening also point to the potential “medicalization” of healthy children and the cost of testing. However, proponents argue that the cost of a lipid panel is negligible compared to the cost of treating premature heart failure, bypass surgeries, and stroke in young adults.
“The evidence gap the USPSTF cites is largely theoretical,” Dr. Samadder argues. “We cannot ethically conduct a 40-year study where we withhold life-saving medication from half a group of children with FH just to prove they have more heart attacks. The biology is clear: high LDL causes heart disease. Lowering it prevents it.”
A Call to Action for 2026
As we move into 2026, the message for parents and clinicians is clear: do not wait for a warning sign.
“If you have a child between the ages of 9 and 11, ask your pediatrician for a cholesterol check,” Dr. Jenkins advises. “It is a simple finger-prick or blood draw that could quite literally define their future. We have the tools to end the legacy of premature heart disease in these families. We just need to use them.”
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- Primary Study on Screening Gaps:
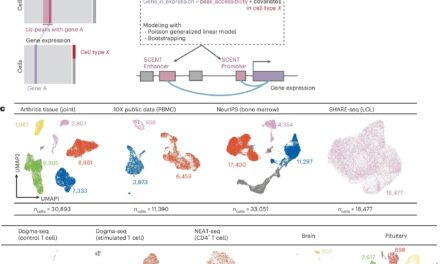
Samadder, N. J., et al. (2025). “Exome Sequencing Enhances Screening for Familial Hypercholesterolemia Within a Multi-Site Healthcare System.” Circulation: Genomic and Precision Medicine. DOI: 10.1161/CIRCGEN.125.005174.