February 25, 2025 – Infectious disease specialists have released updated guidelines for the diagnosis and treatment of Buruli ulcer, a serious tropical disease caused by Mycobacterium ulcerans. The new consensus statement, published in the Medical Journal of Australia, updates the 2014 recommendations based on emerging evidence and growing case numbers in new regions.
What is Buruli Ulcer?
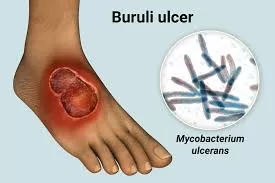
Buruli ulcer is a debilitating skin disease caused by an environmental bacterium that releases toxins, destroying skin, blood vessels, and underlying tissues. This leads to progressive ulceration, which can cause severe disfigurement if left untreated.
Previously, outbreaks were mostly confined to coastal regions of Victoria and northern Queensland. However, recent cases have been reported in Melbourne’s suburbs and Batemans Bay, New South Wales, highlighting the disease’s expanding reach.
Updated Recommendations
The new consensus statement provides critical updates for clinicians managing Buruli ulcer:
- Diagnosis: The preferred diagnostic method is polymerase chain reaction (PCR), using a dry swab from under the ulcer’s edge or a tissue sample from a punch biopsy if no ulcer is present.
- Treatment: The recommended approach is an eight-week course of rifampicin-based dual oral antibiotics, combined with either clarithromycin or a fluoroquinolone. Shorter durations may be considered for smaller lesions with a low risk of relapse.
- Healing Process: Patients should be informed that ulcers typically enlarge during antibiotic treatment and may take four to five months to heal fully.
- Surgical Approach: Aggressive surgery is no longer recommended. Instead, conservative surgical intervention may assist in reducing healing times or antibiotic duration.
- Complications: Paradoxical reactions (immune reconstitution inflammatory reactions) must be promptly recognized and treated, as they can lead to increased tissue damage and delayed healing.
- Wound Care: Proper wound management is essential for effective healing and infection prevention. Patients who cannot manage their own wound dressings should receive assistance from community nursing services.
The guidelines also include recommendations for treating vulnerable populations, including children and Aboriginal and Torres Strait Islander communities.
Prevention Strategies
To reduce the risk of contracting Buruli ulcer, experts recommend the following preventive measures:
- Protect against mosquito bites with repellents, protective clothing, and fly screens.
- Remove potential mosquito breeding sites, such as standing water in pot plants.
- Keep cuts and abrasions clean and covered.
- Limit contact with possums and their excreta, as possums are suspected carriers of the bacterium.
Looking Ahead
With the growing spread of Buruli ulcer in Australia, ongoing research and public health measures will be crucial in controlling the disease. Healthcare professionals and residents in affected areas are urged to stay informed and adopt preventative measures.
For more details, refer to the full publication: Stephen Muhi et al., Management of Mycobacterium ulcerans infection (Buruli ulcer) in Australia: consensus statement, Medical Journal of Australia (2025). DOI: 10.5694/mja2.52591.
Disclaimer: This article is for informational purposes only and should not be considered a substitute for professional medical advice. If you suspect a Buruli ulcer infection, consult a healthcare provider for an accurate diagnosis and appropriate treatment.