Inaccurate blood pressure measurements in clinical settings can lead to misdiagnosis and inappropriate treatment of hypertension, affecting millions worldwide. Recent studies highlight multiple factors behind this problem, including improper technique, equipment issues, and clinic workflow constraints. Experts call for standardized protocols and improved training to ensure accurate readings essential for effective cardiovascular care.
Key Findings and Developments
Recent research published in the Journal of Primary Care & Community Health reveals that between 10% to 50% of patients diagnosed with high office BP readings actually have normal blood pressure outside the clinic setting. This “white coat effect” or measurement inaccuracy can lead to unnecessary initiation or escalation of blood pressure medications, posing risks of adverse side effects and increasing healthcare costs. The American Medical Association (AMA) estimates that inaccurate office BP measurement contributes to inappropriate clinical decisions in 20% to 45% of cases.
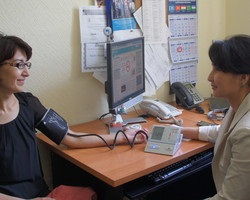
A pivotal barrier identified is the lack of adequate time during routine visits to follow proper measurement protocols. Accurate BP measurement requires patient preparation, correct positioning, multiple readings, and appropriately sized cuffs—steps often skipped in busy clinical workflows. Further complicating accuracy are patient factors such as recent caffeine intake, full bladder, talking during measurement, and movement, which can elevate readings falsely.
Equipment-related issues also contribute significantly. Aneroid sphygmomanometers may lose calibration if not regularly tested annually, a practice often neglected. Additionally, improper cuff size is identified as the number one cause of measurement error, with too-small cuffs overestimating systolic pressure by up to 20 mm Hg.
Expert Perspectives
Jane Drage, AMA improvement specialist, emphasizes the critical role of cuff size selection. She explains that measuring the arm circumference helps determine the correct cuff size, preventing major inaccuracies. Hypertension expert Dr. Andrew Kronish highlights the need for standardized, clinic-wide protocols addressing timing and environment during BP measurement, advocating for quiet, seated rest before readings.
Dr. Albert Hwang, from a study analyzing workflow in primary care clinics, points out that systemic workflow and physical layout often hinder accurate BP measurement, with patients frequently rushed directly to measurement without sufficient rest. He stresses systemic changes, including staff education and clinic workflow redesign, are essential for improvement.
Context and Background
Accurate blood pressure measurement is the cornerstone of diagnosing and managing hypertension, a leading risk factor for heart disease and stroke globally. According to the CDC, nearly half of adults in the United States have hypertension, but many remain undiagnosed or inadequately treated partly due to clinical measurement errors.
Automated office blood pressure monitoring (AOBPM) methods have been promoted to reduce human error, but they have not eliminated inaccuracies entirely. Issues such as patient posture, device placement, and environmental factors remain challenges.
Implications for Public Health
Misdiagnosis due to inaccurate office BP readings contributes to both overtreatment and undertreatment, affecting patient safety and healthcare costs. Overestimation may expose patients to unnecessary medication side effects, while underestimation may miss opportunities for critical intervention.
National initiatives such as the Target: BP program, co-led by the AMA and the American Heart Association, provide resources for training healthcare teams on accurate BP measurement techniques, device selection, maintenance, and standardized workflows, aiming to reduce errors and improve hypertension control rates.
Potential Limitations and Counterarguments
While standardized protocols and new devices can improve accuracy, logistical barriers such as time constraints, clinic layout, and staff workload pose ongoing challenges. Additionally, not all healthcare settings may have access to validated, calibrated equipment or the resources for repeated measurements.
Some experts argue that home and ambulatory blood pressure monitoring should complement office readings to provide a more comprehensive assessment, reducing reliance on sometimes unreliable office measurements.
Medical Disclaimer:
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://www.ama-assn.org/public-health/prevention-wellness/4-big-ways-bp-measurement-goes-wrong-and-how-tackle-them
- https://www.medscape.com/viewarticle/what-causes-inaccurate-office-bp-measurement-and-how-can-we-2025a1000wgw