Uganda’s ongoing battle with mpox has entered a crucial phase as the country reports 8,001 confirmed cases—yet new infections are steadily declining, according to figures from the Ministry of Health released September 5, 2025. Health authorities are cautiously optimistic, with vaccination campaigns and expanded surveillance credited for the downward trend.
Mpox Situation in Uganda
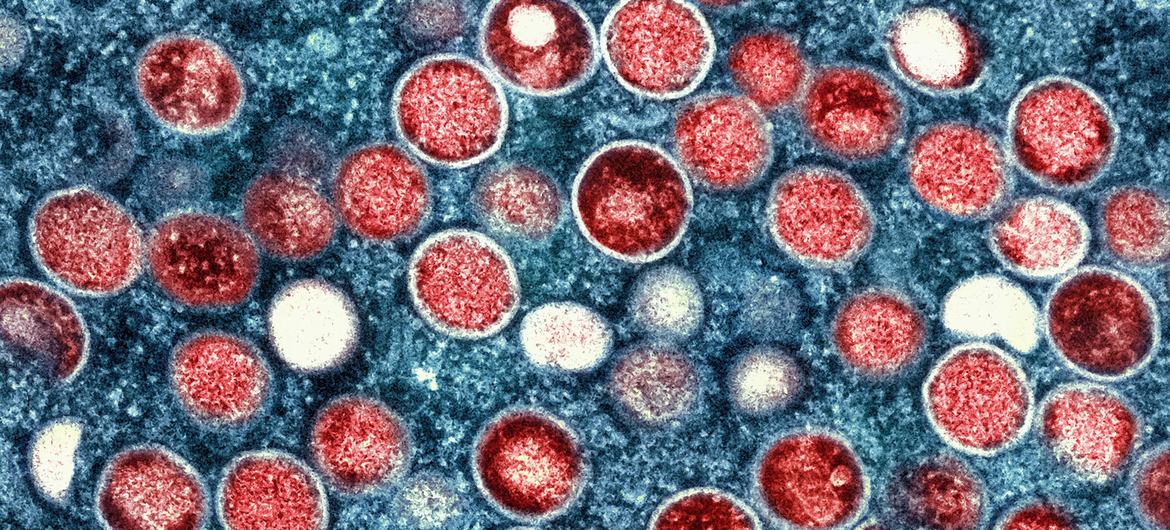
Mpox, formerly called monkeypox, is a viral infectious disease known for symptoms such as fever, swollen lymph nodes, muscle aches, skin rashes, and a sore throat. The outbreak in Uganda began in August 2024 and quickly spread to 120 out of 146 districts. In the past 24 hours, Uganda registered 15 new cases and two deaths, adding to a cumulative total of 50 fatalities. Notably, 46% of those who died were coinfected with HIV.
A significant milestone was reached recently: for six consecutive weeks, incident cases have stayed below 100 per week—a sign of progress since October 2024. Young adults (ages 20–29) remain at highest risk, with sexual networks shown as a major driver of transmission, though household and community spread are also increasing.
Key Developments and Health Initiatives
Authorities have ramped up several initiatives:
-
Mass vaccination campaigns targeting high-risk groups, including healthcare workers.
-
Deployment of a novel epidemic alert system—health workers receive mobile notifications about suspected mpox cases, allowing for rapid response and containment.
-
Strengthened surveillance and case management protocols.
Dr. Misaki Wayengera, a senior official at the Ugandan Ministry of Health, highlighted that “when a public health emergency becomes a community problem we all need to respond. Mpox has emerged as a community disease”.
Global Perspective and WHO Response
Globally, mpox is no longer considered an international health emergency, as declared by the World Health Organization (WHO) in September 2025. WHO Director-General Dr. Tedros Adhanom Ghebreyesus stated that the “lifting of the emergency declaration does not mean the threat is over, nor that our response will stop”. Internationally, over 34,000 confirmed cases and 138 deaths have been reported in 2025, with neighboring countries like DRC having higher caseloads.
Despite the downgrade of emergency status, the WHO and local officials emphasize ongoing vigilance, resource mobilization, and public health efforts. Experts such as Dr. Dimie Ogoina, chair of the WHO emergency committee, stress that “mpox remains a public health concern, globally and especially in Africa, and there’s a need for us not to be complacent about the response strategy”.
Transmission Dynamics and At-Risk Populations
Mpox spreads through close personal contact: skin-to-skin, mouth-to-mouth, mouth-to-skin, and also via respiratory droplets in close proximity. People with multiple sexual partners, healthcare workers (via needle injuries), and those exposed to contaminated objects (clothing, linens) are at higher risk. Animal-to-human transmission can occur, though the exact animal reservoir remains unknown.
Pregnant individuals face heightened risks—the virus may be transmitted during pregnancy or birth, endangering both parent and child. In Uganda, 46% of mpox fatalities had HIV coinfection; underlying illnesses and immunocompromised status increase the severity of disease and fatal outcomes.
Statistical and Epidemiological Context
-
Total cases in Uganda (Sep 2025): 8,001
-
Total deaths: 50 (46% HIV coinfection)
-
Mpox now found in 82% of districts, with Kampala region reporting the highest concentration
-
Age most affected: 20–29 years
-
Global mpox cases (Jan–Jul 2025): Over 34,000; deaths: 138
-
Median age of Ugandan cases: 29 years; 52% male, 48% female
Expert Perspectives
Dr. Boghuma Titanji, infectious diseases expert at Emory University, noted that prior declarations of emergency “did very little to change the reality on the ground for many communities most affected by mpox”. Dr. Nicholas Bamulasa, head of Nabweru Health Centre III, underlines the critical role of community-trained surveillance officers in successful containment.
Practical Implications for Readers
For the public, the current phase of Uganda’s mpox outbreak highlights the importance of:
-
Maintaining vigilance, especially for those at higher risk (young adults, people with HIV, healthcare workers, multiple sexual partners).
-
Participating in vaccination campaigns where available.
-
Practicing infection prevention: hygiene, isolation of suspected cases, safe handling of potentially contaminated materials.
-
Consulting healthcare professionals about symptom recognition, testing, and treatment.
Limitations and Counterarguments
While progress in Uganda is encouraging, experts caution that underreporting, evolving transmission patterns, and patchy healthcare infrastructure could obscure the true scale of the outbreak. Additionally, more research is needed on transmission dynamics, especially in community and household settings.
Public Health Outlook
Uganda’s experience underscores the need for sustainable investment in public health surveillance, rapid response systems, vaccination infrastructure, and community engagement. With WHO’s emergency status lifted, national and regional collaboration remains vital to ensure continued progress and preparedness for future outbreaks.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.