Published: January 15, 2026
DAEJEON, South Korea — Researchers at the Korea Advanced Institute of Science and Technology (KAIST) have unveiled a sophisticated new immunotherapy strategy that could bypass the most grueling hurdles of modern cancer treatment. By injecting specialized genetic “instructions” directly into a tumor, the team successfully reprogrammed resident immune cells—originally suppressed by the cancer—into aggressive hunters capable of destroying the disease from the inside out.
The study, led by Professor Ji-Ho Park and published in the journal ACS Nano, represents a paradigm shift in Chimeric Antigen Receptor (CAR) therapy. Unlike current methods that require a multi-week, high-cost laboratory process to engineer a patient’s cells, this “in-vivo” (inside the body) approach transforms cells where they sit, potentially offering a faster and more affordable lifeline for patients with hard-to-treat solid tumors.
The “Trojan Horse” of the Immune System
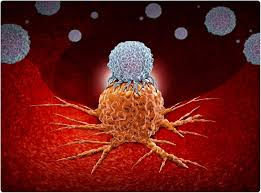
To understand the breakthrough, one must first understand the macrophage. In a healthy body, these white blood cells act as the “cellular vacuum cleaners,” engulfing pathogens and debris. However, tumors are masters of manipulation. They often hijack macrophages, sending signals that flip them from “anti-tumor” defenders to “pro-tumor” accomplices that actually help the cancer grow and hide from the immune system.
While much of the medical world has focused on CAR-T cell therapy—which targets T-cells—the KAIST team focused on these Tumor-Associated Macrophages (TAMs). Because macrophages are already present in high numbers inside dense solid tumors like lung, liver, and gastric cancers, they are perfectly positioned to act if they can be “re-educated.”
“Solid tumors are like fortresses; it is incredibly difficult for external immune cells to penetrate the dense tissue,” explains Dr. Jun-Hee Han, the study’s lead author. “Our strategy was to stop trying to force our way in and instead recruit the ‘guards’ already standing at the gates.”
How It Works: Direct Reprogramming
The KAIST team developed a delivery vehicle known as a lipid nanoparticle (LNP)—similar to the technology used in mRNA COVID-19 vaccines. These nanoparticles were engineered to be swallowed specifically by macrophages.
Inside the LNP is a payload of messenger RNA (mRNA) that carries the blueprint for a Chimeric Antigen Receptor (CAR). Once the macrophage absorbs the LNP, it begins producing these CAR proteins on its surface. These proteins act like a “GPS,” allowing the macrophage to recognize specific markers on cancer cells that were previously invisible to it.
The result is a CAR-macrophage. Not only does this transformed cell begin to “eat” the cancer cells directly (a process called phagocytosis), but it also releases chemical signals that “wake up” other nearby immune cells, creating a localized inflammatory “hot zone” that the cancer can no longer survive.
The Animal Trials: A Body-Wide Response
In laboratory models of melanoma, the researchers found that the treatment significantly suppressed tumor growth. Perhaps most importantly, the researchers observed a “systemic” effect. Even though the injection was local, the immune system appeared to learn how to recognize the cancer elsewhere in the body, suggesting the potential for treating metastatic disease.
Expert Perspective: A Leap Toward “Off-the-Shelf” Therapy
While the KAIST study is currently in the pre-clinical phase, outside experts say the implications for public health are profound.
“The current bottleneck in immunotherapy is the ‘vein-to-vein’ time,” says Dr. Elena Rossi, an independent oncology researcher not involved in the study. “Currently, we have to ship a patient’s blood to a lab, wait weeks for modification, and then re-infuse it. Many patients with late-stage cancer simply don’t have that kind of time. A therapy that can be administered via a simple injection in a clinic would be a game-changer.”
However, Dr. Rossi cautions that moving from mice to humans involves significant hurdles. “The human immune system is vastly more complex. We must ensure that these reprogrammed macrophages don’t become overactive and attack healthy tissue, a condition known as ‘off-target’ toxicity.”
Comparing the Approaches
| Feature | Conventional CAR-T/CAR-M | KAIST In-Vivo Reprogramming |
| Cell Source | Patient’s blood (harvested) | Resident cells (already in tumor) |
| Manufacturing | Specialized external lab | Inside the patient’s body |
| Timeframe | 2–4 weeks | Immediate (post-injection) |
| Cost | High ($400k+ per dose) | Potentially much lower |
| Primary Target | Blood cancers (Leukemia/Lymphoma) | Solid tumors (Lung/Liver/Melanoma) |
Challenges and Limitations
Despite the excitement, the KAIST researchers and the broader scientific community acknowledge several limitations:
-
Delivery Precision: Ensuring the nanoparticles only target macrophages and not other healthy cells remains a technical challenge.
-
Duration of Effect: mRNA is naturally degraded by the body over time. This means the “reprogramming” may be temporary, potentially requiring multiple injections to sustain the attack on the tumor.
-
Human Translation: Animal models, particularly in melanoma, often respond more vigorously to immunotherapy than human solid tumors, which have more complex “immunosuppressive shields.”
What This Means for Patients
For those currently undergoing cancer treatment, this research does not change the standard of care today. However, it signals a move toward “precision internal medicine.” If successful in human trials, this technology could turn a terminal diagnosis into a manageable condition by utilizing the body’s own natural architecture.
“This study presents a new concept,” says Prof. Ji-Ho Park. “By addressing the delivery efficiency and the suppressed environment of the tumor simultaneously, we are providing a roadmap for the next generation of cancer treatment.”
The research was supported by the National Research Foundation of Korea and continues to undergo rigorous testing as it moves toward the clinical trial pipeline.
References
- https://www.daijiworld.com/news/newsDisplay?newsID=1303631
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.