CLEVELAND, OH — For more than a century, a diagnosis of Alzheimer’s disease has been viewed as an irreversible, one-way street toward cognitive decline. However, a groundbreaking study published this week in Cell Reports Medicine is challenging this medical dogma. Researchers from University Hospitals (UH), Case Western Reserve University, and the Louis Stokes Cleveland VA Medical Center have demonstrated that restoring a specific energy molecule in the brain can not only halt but actually reverse advanced symptoms of the disease in animal models.
The study, led by Kalyani Chaubey, Ph.D., suggests that the “damaged” brain may possess an inherent, untapped capacity to repair itself if provided with the right biochemical support. By targeting the balance of Nicotinamide Adenine Dinucleotide (NAD+), a molecule essential for cellular energy, the team achieved full neurological recovery in mice—a feat previously thought impossible once the disease reached an advanced stage.
The Energy Crisis in the Alzheimer’s Brain
At the heart of this discovery is NAD+, a coenzyme found in every living cell. It acts like a cellular currency, powering the metabolic processes that allow neurons to communicate, repair DNA, and defend against stress. While NAD+ levels naturally decline as we age, the research team found that this “energy crisis” is significantly more profound in brains afflicted by Alzheimer’s.
“Without proper NAD+ balance, cells eventually become unable to execute critical processes required for proper functioning and survival,” the study authors noted. By analyzing human brain tissue and mouse models, the researchers confirmed that this precipitous drop in NAD+ is a primary driver of the neurodegeneration seen in Alzheimer’s patients.
A Two-Pronged Attack on Pathology
To test whether restoring this balance could heal the brain, the team used two distinct mouse models:
-
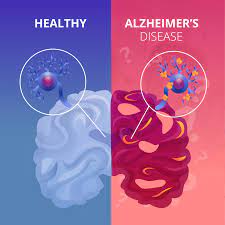
The Amyloid Model: Mice engineered with mutations that cause the buildup of “plaques” between neurons.
-
The Tau Model: Mice engineered with mutations leading to “tangles” inside neurons.
Both amyloid plaques and tau tangles are hallmarks of human Alzheimer’s, leading to a cascade of destruction: the breakdown of the blood-brain barrier, widespread inflammation, and the loss of synapses (the connections between brain cells).
From Advanced Decline to Full Recovery
Unlike most clinical trials that focus on early intervention or prevention, the Cleveland-based team waited until the mice showed significant, advanced disease. They then administered a pharmacological agent called P7C3-A20, a compound developed in the laboratory of Andrew A. Pieper, MD, Ph.D.
The results were startling. Not only did the treatment stop further damage, but it also enabled the brain to “fix” existing pathological events. The mice showed:
-
Restoration of the Blood-Brain Barrier: The protective shield of the brain was repaired.
-
Reduced Inflammation: Widespread neuroinflammation subsided.
-
Cognitive Recovery: Perhaps most importantly, the mice regained their ability to perform memory and learning tasks, returning to levels seen in healthy, “normal” mice.
“We were very excited and encouraged by our results,” said Dr. Pieper, senior author of the study and Director of the Brain Health Medicines Center at the Harrington Discovery Institute. “Restoring the brain’s energy balance achieved pathological and functional recovery in both lines of mice with advanced Alzheimer’s.”
A Note of Caution: Not All NAD+ Boosters are Equal
While these results offer immense hope, Dr. Pieper issued a critical warning for consumers. Currently, various NAD+ “precursors” (like NR or NMN) are sold over-the-counter as supplements. However, the study utilized a specific pharmacological approach—P7C3-A20—rather than high-dose supplements.
“Currently available over-the-counter NAD+ precursors have been shown in animal models to raise cellular NAD+ to dangerously high levels that promote cancer,” Dr. Pieper explained. The P7C3-A20 compound works differently: it helps the cell maintain its natural balance under stress without pushing levels into a “supraphysiologic” range that could trigger unintended side effects.
Expert Perspective: A Paradigm Shift
The implications for public health are significant. For decades, the “Amyloid Hypothesis”—the idea that clearing plaques is the only way to treat Alzheimer’s—has dominated the field. This new research suggests that focusing on bioenergetics (how cells use energy) might be a more effective route to recovery.
“The key takeaway is a message of hope—the effects of Alzheimer’s disease may not be inevitably permanent,” Dr. Pieper said.
Independent experts note that while mouse models are an essential step, human biology is vastly more complex. Translating “full recovery” from a mouse to a human will require rigorous, multi-phase clinical trials. However, the study also identified specific proteins in human Alzheimer’s brains that correlate with these findings, providing a roadmap for upcoming human studies.
What This Means for Patients and Families
For the millions of families currently navigating an Alzheimer’s diagnosis, this research marks a transition from “managing decline” to “pursuing recovery.”
-
New Biomarkers: The study found that blood levels of phosphorylated tau 217 (p-tau217)—a marker already used in human diagnostics—normalized as the mice recovered. This could provide a non-invasive way to track treatment success in future human trials.
-
Future Trials: The technology is currently being commercialized by Glengary Brain Health, with the goal of moving into human clinical trials as soon as possible.
Next Steps in Research
The research team is now focused on:
-
Identifying which specific aspects of brain energy balance are most vital for repair.
-
Determining if this “recovery approach” works for other neurodegenerative conditions, such as Parkinson’s disease or ALS.
-
Moving P7C3-A20 into carefully designed human trials to ensure safety and efficacy.
As we look toward 2026 and beyond, the medical community is watching closely to see if the resilience shown in the laboratory can finally be mirrored in the clinic.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
Peer-Reviewed Studies:
-
Chaubey, K., et al. (2025). Pharmacologic reversal of advanced Alzheimer’s disease in mice and identification of potential therapeutic nodes in human brain. Cell Reports Medicine. DOI: 10.1016/j.xcrm.2025.102535
-
Pieper, A. A., et al. (Previous Work). Restoring the brain’s NAD+ balance achieves pathological and functional recovery after severe traumatic brain injury. Proceedings of the National Academy of Sciences (PNAS).