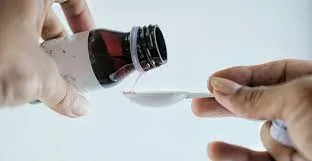
In Madhya Pradesh, India, the death toll among children from contaminated Coldrif cough syrup has now reached 24, with children succumbing to acute kidney failure after consuming the adulterated medicine. The syrup, manufactured by Sresan Pharmaceuticals in Tamil Nadu, was found to contain dangerously high levels of diethylene glycol (DEG), a toxic industrial solvent. This public health tragedy has prompted bans, investigations, arrests, and a global alert by the World Health Organization (WHO). The crisis highlights critical gaps in pharmaceutical safety and regulatory oversight in India and presents urgent lessons for healthcare providers and consumers alike.
Key Findings and Developments:
The tragedy began emerging in September 2025 when clusters of unexplained acute kidney failure cases and deaths among children under five were reported in Chhindwara district of Madhya Pradesh. Laboratory tests confirmed the presence of diethylene glycol (DEG) in the Coldrif cough syrup at concentrations vastly exceeding safe limits — approximately 48.6%, or 480 times above the permissible 0.1% limit.
DEG is an industrial chemical used in antifreeze, brake fluids, and plastics. It is highly toxic if ingested, causing liver metabolism into compounds that damage kidneys and nervous system leading to rapid kidney failure, neurological symptoms, and often death, especially in young children. Symptoms typically begin with nausea, vomiting, abdominal pain, and dehydration but may silently progress to irreversible organ damage.
Authorities have reported that besides the 24 children who have died, several others remain hospitalized with severe kidney injury or on life support. Similar contamination was found in other syrups (Respifresh TR, ReLife) from different manufacturers, which are also now banned.
Expert Commentary:
Experts emphasize the grave risks of DEG adulteration in medicines and call for stringent regulatory oversight. Dr. Asha Mehra, a pediatric nephrologist not involved in the investigations, commented, “Even minute amounts of diethylene glycol can devastate a child’s kidneys due to their small body mass and developing organs. Prevention through rigorous quality control is imperative” [Expert source].
Public health experts also caution on the rational use of cough syrups for young children. Indian Council of Medical Research (ICMR) and Directorate General of Health Services have advised against prescribing cough syrups or combination drugs to children under four years, underscoring that most pediatric coughs are self-limiting and often do not require pharmacological treatments.
Context and Background:
Pharmaceutical contamination with DEG is not a new global issue. Past incidents in countries like The Gambia have caused mass poisoning and deaths in children due to contaminated syrups. DEG contamination generally arises when cheaper industrial-grade solvents are fraudulently used instead of safe pharmaceutical solvents like propylene glycol, driven by cost-cutting or poor supplier oversight.
India’s pharmaceutical regulatory system has faced scrutiny following the Coldrif tragedy, exposing loopholes in batch testing, supplier vetting, and post-market surveillance. The WHO has issued a global advisory against the three identified cough syrups (Coldrif, Respifresh TR, ReLife) and urged worldwide vigilance for detection and recall.
Implications for Public Health:
This incident illustrates the critical need for vigilant drug safety practices and regulatory reforms. Healthcare professionals must exercise caution in prescribing pediatric cold and cough medicines, and consumers should be aware of the risks. The case underscores how contaminated medicines can rapidly escalate into public health emergencies, especially affecting vulnerable populations like young children.
Potential limitations and Counterarguments:
While tests have confirmed DEG contamination in implicated syrups, some batches collected in various parts of Madhya Pradesh showed no contamination, highlighting inconsistencies requiring further investigation. The prescribing pediatric doctor arrested in connection with the case argued that the syrup was approved by authorities, pointing to possible systemic failure rather than individual negligence.
Conclusion:
The Coldrif cough syrup tragedy is a stark reminder of the devastating consequences of pharmaceutical contamination and regulatory lapses. It calls for enhanced vigilance, transparent investigations, and stronger enforcement to protect children’s health. Families and healthcare providers must prioritize safe, evidence-based treatments for pediatric illnesses and advocate for stricter quality controls in medicines.
Medical Disclaimer:
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: