LOS ANGELES — Researchers at the University of California, Los Angeles (UCLA) have developed a pioneering implantable microdevice designed to solve one of the most persistent hurdles in cancer treatment: the “exhaustion” of immune cells within a tumor. The study, published recently in Nature Biomedical Engineering, introduces a biocompatible scaffold that acts as a local “charging station,” providing engineered immune cells with the continuous stimulation and nutrients they need to sustain a prolonged attack on solid tumors. By reinforcing the immune response directly at the site of the disease, this “immunoengineering” approach could significantly improve outcomes for therapies that currently struggle to penetrate the hostile environment surrounding many cancers.
The Fuel Crisis in Cancer Immunotherapy
Immunotherapy has fundamentally shifted the oncology landscape, moving the focus from attacking the cancer directly with chemicals to empowering the body’s own immune system to do the work. However, while drugs like checkpoint inhibitors and cellular therapies like CAR-T have saved countless lives, they face a steep uphill battle against solid tumors.
Inside a tumor, the environment is often “immunosuppressive”—a biological fortress where oxygen is low, nutrients are scarce, and chemical signals actively shut down immune activity. Consequently, even the most advanced engineered T-cells often “run out of gas” shortly after arriving at the scene.
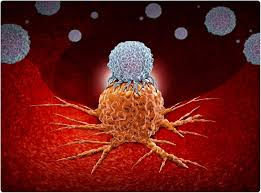
The UCLA team’s solution is a tiny, porous scaffold placed near or within the tumor. This device is embedded with biomimetic microparticles that mimic the natural signals the body uses to keep immune cells in “fighting mode.”
“You can think of it almost like plugging your phone into a charging cable,” said Yan-Ruide “Charlie” Li, a postdoctoral scholar at UCLA and the study’s first author. “The cells connect to the activation signal, get a boost, and then head back out to destroy cancer cells.”
How the “Charging Station” Works
The device specifically supports an emerging class of treatment known as chimeric antigen receptor–invariant natural killer T cells (CAR-iNKT cells). While traditional CAR-T cells are the current gold standard for blood cancers, CAR-iNKT cells are increasingly viewed as a more potent weapon against solid tumors because they can navigate dense tissue more effectively.
Once the scaffold is implanted, it performs three critical functions:
-
Recruitment: It draws the engineered CAR-iNKT cells toward the tumor site.
-
Reactivation: The microparticles within the scaffold provide repeated “hits” of activation signals that keep the cells from becoming dormant.
-
Sustenance: The device slowly releases IL-15, a growth-supporting cytokine (a type of protein) that helps the immune cells multiply and persist over time.
Dr. Song Li, chancellor’s professor of bioengineering at UCLA Samueli and a senior author on the study, noted that the engineering required a delicate balance. “Too much stimulation can exhaust immune cells, while too little lets them fade quickly,” he explained. “We spent a lot of time optimizing the strength of the signals to keep immune activity in a therapeutic window.”
Key Findings: Longer Survival and “Immune Memory”
In laboratory experiments using human melanoma and lymphoma samples, the results were striking. The immune cells supported by the implant remained active significantly longer than those left to fend for themselves in tumor-like conditions.
Perhaps most importantly, the repeated stimulation helped the immune cells form “memory.” In the world of oncology, immune memory is the holy grail; it allows the body to recognize and destroy the same cancer if it attempts to return, potentially preventing a relapse.
While the current study focused on specific cancer models, the researchers emphasize that the platform is modular. By swapping out the molecules on the microparticles, the device could theoretically be “tuned” to support various types of immune cells or target different forms of cancer, such as pancreatic or gastrointestinal tumors.
The Rise of Immunoengineering
This research reflects a broader shift toward “immunoengineering”—a field that combines materials science with biology to modify the local immune landscape.
“Instead of just giving immune cells a one-time push from outside the body, we’re now learning how to maintain them inside the tumor,” said Dr. Michelle Monje, a neuro-oncologist and researcher (not involved in the study). “Engineering scaffolds that provide sustained, localized signals could be a game-changer for solid tumors.”
Currently, only about 20% to 40% of patients respond robustly to standard immunotherapies. By concentrating support exactly where it is needed, doctors hope to increase these response rates while simultaneously reducing side effects. Many systemic immunotherapies require high doses of drugs that circulate throughout the entire body, often causing collateral damage to healthy organs—leading to conditions like colitis or pneumonitis. Localized delivery via an implant could mitigate these risks.
Limitations and the Road Ahead
Despite the excitement, experts urge a measured perspective. The technology is in the preclinical stage, meaning it has yet to undergo the rigorous, multi-year human clinical trials required for FDA approval.
Dr. Javid Moslehi, a cardiologist and immunotherapy safety expert at Vanderbilt University, points out that adding hardware to a treatment regimen introduces new variables. “New engineering approaches are exciting, but they add another layer of complexity,” Moslehi noted. “We need to understand how these implants interact with the body’s existing regulatory systems and whether they increase the risk of local inflammation or infection.”
Other practical questions include:
-
Delivery: How easily can these be implanted in hard-to-reach internal organs?
-
Durability: How long does the “charge” last before the scaffold needs to be replaced or absorbed by the body?
-
Biocompatibility: Will the body’s natural foreign-object response eventually wall off the device, rendering it useless?
What This Means for Patients
For now, this “immune charging station” remains a promising look into the future of cancer care rather than a current treatment option. Patients should not seek out this device in clinical practice today but should instead view it as a signal of where the field is headed: toward more personalized, localized, and sustained treatments.
If you or a loved one are currently undergoing cancer treatment, the best course of action remains a close dialogue with an oncology team. Questions regarding participation in clinical trials for “next-generation” immunotherapies—including those involving CAR-iNKT cells—are becoming increasingly relevant as these engineering-driven solutions move toward the clinic.
The takeaway for the health-conscious public is clear: The next frontier of cancer survival likely won’t just come from a new drug, but from the clever engineering that helps our existing internal defenses stay in the fight.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
Study Citations:
- https://scitechdaily.com/this-tiny-device-could-solve-one-of-immunotherapys-biggest-weaknesses/