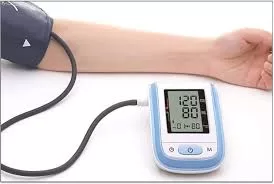
In a potential shift for the millions of adults living with hypertension, new clinical evidence suggests that a single, low-dose “triple pill” is as effective—and in some cases superior—to the standard practice of starting patients on a single, full-dose medication.
The findings, published in the Journal of the American College of Cardiology, come from two Phase 3 double-blind trials, HM-APOLLO-301 and HM-APOLLO-302. The studies suggest that by hitting high blood pressure from three different physiological angles simultaneously at very low doses, doctors can achieve faster control with fewer side effects than the traditional “start low and go slow” approach with a single drug.
Redefining the First Line of Defense
For decades, the standard of care for mild-to-moderate hypertension has been monotherapy: starting a patient on one drug, such as a calcium-channel blocker or an ACE inhibitor, and slowly increasing the dose or adding a second drug if targets aren’t met.
However, investigators for the HM-APOLLO trials argue this traditional method may actually hinder patient health. Titrating a single drug upward can increase the risk of dose-related side effects and delay the time it takes to reach healthy blood pressure levels. Furthermore, the more pills a patient has to take at different times of the day, the more likely they are to miss a dose—a hurdle known as “treatment non-adherence.”
“Starting treatment with single-pill combination therapy helps to achieve therapeutic targets faster,” noted a recent report in the Cleveland Clinic Journal of Medicine, echoing the sentiment of the HM-APOLLO investigators.
The Study: 610 Patients, Two Crucial Comparisons
The multicenter trials, conducted in South Korea, enrolled 610 adults with mild-to-moderate hypertension (systolic blood pressure between 140 and 180 mm Hg). Following a four-week placebo period to establish a baseline, participants were randomized into two eight-week trials.
The “Triple Pill” used in the study contained ultra-low doses of three common medications:
-
Amlodipine (1.67 mg): A calcium-channel blocker that relaxes blood vessels.
-
Losartan (16.67 mg): An angiotensin receptor blocker (ARB) that prevents blood vessels from narrowing.
-
Chlorthalidone (4.17 mg): A diuretic that helps the kidneys remove excess water and salt.
The Results
The researchers compared this low-dose trio against standard-dose versions of the individual components:
-
Triple Pill vs. Amlodipine (Study 301): The low-dose combination was found to be just as effective as a full 5 mg dose of amlodipine. Both groups saw a systolic reduction of approximately 19 mm Hg.
-
Triple Pill vs. Losartan (Study 302): The combination therapy was superior to 50 mg of losartan. The triple pill reduced systolic blood pressure by 19.9 mm Hg, compared to only 16.4 mm Hg for the single-drug group ($P = .037$).
Notably, in the losartan comparison, 64% of patients on the triple pill achieved blood pressure control (<140/90 mm Hg), compared to only 51% of those on the single drug.
A “Win” for Precision Medicine and Women’s Health
One of the most intriguing findings from the trials involved sex-based responses to the medication. Exploratory analyses showed that women experienced significantly greater reductions in blood pressure than men when taking the triple pill.
In Study 302, the triple pill outperformed losartan by a much wider margin in women than in men. “This suggests that multi-mechanism, ultra-low-dose triple combination therapy… may provide particular benefit in certain subgroups, including women,” said Dr. Moo-Yong Rhee, a professor of cardiology at Dongguk University Ilsan Hospital and a study author.
Dr. Rhee emphasized that because women have historically been underrepresented in heart research, these findings are a vital step toward “individualized and precision-based hypertension management.”
Global Implications: Cost and Accessibility
While the “Triple Pill” tested in these trials is not yet a standard option in the United States, cardiovascular experts see a bright future for the strategy.
Dr. Clyde Yancy, Chief of Cardiology at Northwestern Medicine Bluhm Cardiovascular Institute, believes the global impact could be massive. “I would readily embrace a low-dose combination pill,” Yancy said, noting that these types of medications should ideally be available at a very low cost.
“With a conservative estimate of an at least 10-mm Hg blood pressure reduction, the global burden of cardiovascular disease would diminish,” Yancy added. This is particularly relevant for low- and middle-income countries, where access to frequent doctor visits for “titrating” or adjusting medication doses is often limited.
Limitations and Future Outlook
Despite the positive data, the study has limitations. The trial period was relatively short (eight weeks), and the study population was limited to adults in South Korea, meaning more research is needed to see if these results remain consistent across more diverse global populations over several years.
Additionally, in Study 301, the “non-inferiority” margin—the statistical bar used to prove the new pill is “just as good” as the old one—was slightly exceeded in some specific analyses, though the authors maintain the clinical results remain consistent.
For now, the message for patients is one of cautious optimism. The shift from “one big pill” to “three tiny ones in one” may soon offer a faster, safer, and simpler way to keep the “silent killer” of hypertension at bay.
References
https://www.medscape.com/viewarticle/low-dose-combo-pill-treating-hypertension-shows-positive-2026a10005ra
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.