In the quiet progression of chronic illness, few connections are as profound—or as frequently overlooked—as the link between the glucose in our bloodstream and the clarity of our vision. While many patients associate diabetes primarily with heart health or nerve pain, a growing body of clinical evidence suggests that the eyes are often the first casualty of metabolic dysfunction.
Recent data from the Centers for Disease Control and Prevention (CDC) indicates that approximately 9.6 million Americans are living with diabetic retinopathy, a leading cause of blindness in working-age adults. Yet, medical experts stress that this vision loss is not an inevitability. Through a combination of rigorous glycemic control, lifestyle modifications, and early screening, the “silent thief” of diabetic eye disease can be halted in its tracks.
The Biological Link: Glucose and the Retina
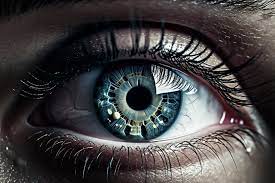
To understand why blood sugar matters for your eyes, one must look at the microvascular level. The retina—the light-sensitive tissue at the back of the eye—is nourished by a dense network of tiny, fragile blood vessels.
When blood glucose levels remain chronically elevated, these vessels undergo structural changes. High sugar levels weaken the vessel walls, making them prone to leaking fluid or blood into the eye. In response to poor circulation, the eye may attempt to grow new, abnormal blood vessels. However, these new vessels are fragile and often leak further, leading to scarring and, in severe cases, retinal detachment.
“The eye is essentially a window into the body’s vascular system,” says Dr. Elena Rossi, an ophthalmologist not involved in the latest CDC reporting. “We often see the first signs of systemic diabetes during a routine eye exam. When those tiny vessels in the retina are under stress, it’s a clear signal that the rest of the body’s microvasculature is likely struggling as well.”
The Core Pillars of Protection
Protecting your vision requires a multi-pronged approach that extends beyond the medicine cabinet. According to the American Diabetes Association (ADA), “consistent” control is more impactful than “occasional” perfection.
1. Stability Over Fluctuations
Maintaining stable blood sugar levels is the most powerful defense. Sharp spikes and crashes in glucose can cause the lens of the eye to swell, leading to blurred vision that fluctuates throughout the day. Long-term elevation, however, leads to permanent damage. Clinical trials, such as the landmark Diabetes Control and Complications Trial (DCCT), proved that intensive blood sugar control reduces the risk of developing retinopathy by as much as 76%.
2. The “Double Stress” of Blood Pressure
Hypertension (high blood pressure) acts as a force multiplier for eye damage. When blood pressure is high, it puts additional physical strain on the already weakened retinal vessels. Managing blood pressure helps reduce the risk of “wet” complications, such as macular edema (swelling in the sharp-vision area of the retina).
3. Annual Dilated Examinations
Because diabetic retinopathy often presents no symptoms in its early stages, the ADA recommends an annual dilated eye exam for everyone with diabetes. Unlike a standard vision test for glasses, a dilated exam allows an eye specialist to see the retina clearly and identify microaneurysms or early swelling before they affect your sight.
Lifestyle as Medicine: Diet, Exercise, and Smoking
Preventative care is rooted in daily habits. A nutrient-rich diet—specifically one high in leafy greens, fiber, and omega-3 fatty acids—provides the antioxidants necessary to combat oxidative stress in the ocular tissues. Nutrients like lutein and zeaxanthin are particularly noted for their role in retinal health.
Physical activity also plays a critical role. Regular movement—even 30 minutes of brisk walking—improves insulin sensitivity, allowing the body to clear glucose from the blood more efficiently. This reduces the “soaking” effect that high sugar has on the delicate tissues of the eye.
Furthermore, medical authorities are unanimous on the dangers of smoking for diabetic patients. Smoking constricts blood vessels and reduces oxygen delivery to the retina, significantly accelerating the progression of vision loss.
Recognizing the Warning Signs
While the goal is to intervene before symptoms appear, patients should be vigilant for “red flag” changes, including:
-
Floaters: Dark spots or “cobwebs” that seem to float in your field of vision.
-
Fluctuating Vision: Sight that changes from clear to blurry over the course of a day.
-
Empty Spots: Dark or blank areas in the center of your vision.
-
Poor Night Vision: Increasing difficulty seeing in low-light conditions.
The Shift Toward Prevention
While modern medicine offers advanced treatments—including intravitreal injections (medication injected into the eye) and laser photocoagulation—these are reactive measures.
“We have incredible tools to save vision today, but they are not ‘cures,'” notes Dr. Rossi. “A laser can seal a leaking vessel, but it cannot restore the natural health of the retina once extensive damage has occurred. Prevention is not just safer; it is significantly more effective at preserving quality of life.”
Who is Most at Risk?
The risk of complications increases with:
-
Duration: The longer you have lived with diabetes.
-
Uncontrolled A1C: Persistently high average blood sugar.
-
Comorbidities: High cholesterol and hypertension.
-
Pregnancy: Gestational diabetes or pregnancy in those with Type 1 or Type 2 can cause rapid changes in eye health.
Looking Ahead
Vision loss from diabetes is largely preventable. By focusing on the “ABCs” of diabetes management—A1C (blood sugar), Blood pressure, and Cholesterol—and committing to annual screenings, patients can protect their sight for a lifetime. Your vision is a precious resource; protecting it begins with the choices you make at the dinner table and the consistency of your medical check-ups.
References
https://www.edexlive.com/news/why-blood-sugar-control-matters-for-your-eyes
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.