NEW DELHI — As India undergoes a seismic demographic shift toward an older population, a dormant viral threat is emerging from the shadows. Data released during Shingles Action Week (February 23–March 1, 2026) highlights a critical surge in shingles vulnerability among the nation’s 153 million seniors. Despite the availability of high-efficacy vaccines, experts warn that a combination of low public awareness, high out-of-pocket costs, and policy gaps is leaving millions of Indians—particularly those with chronic illnesses—unprotected against a disease that can cause debilitating, long-term nerve pain.
The Enemy Within: Understanding the Shingles Surge
Shingles, medically known as herpes zoster, is not a new infection. It is the second act of the varicella-zoster virus, the same pathogen responsible for childhood chickenpox. After the initial spots fade in childhood, the virus doesn’t leave the body; instead, it retreats into the nerve tissues near the spinal cord and brain, lying dormant for decades.
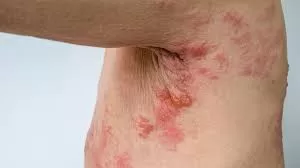
As the immune system weakens—a process called immunosenescence that occurs naturally with age or is accelerated by chronic illness—the virus can “reactivate.” It typically manifests as a painful, blistering rash on one side of the body, often following the path of a specific nerve (thoracic dermatomes).
For many, the rash is only the beginning. Between 10% and 30% of patients develop Post-Herpetic Neuralgia (PHN), a complication where “shock-like” nerve pain persists for months or even years after the rash has healed. In India, studies suggest PHN prevalence may be as high as 24% among the elderly, significantly disrupting their ability to work, sleep, or socialize.
A Perfect Storm: Ageing and Chronic Disease
The scale of the threat is tied directly to India’s changing biology. By 2050, India’s over-60 population is projected to reach 347 million. Currently, over 75 million of these seniors live with at least one chronic condition, such as diabetes or cardiovascular disease.
“More than 90% of adults over 50 in India carry the dormant chickenpox virus,” explains Dr. Monalisa Sahoo, an infectious diseases expert. “As the immune system declines with age or is compromised by conditions like diabetes, the virus seizes the opportunity to reactivate.”
The risk is not distributed equally. Research indicates:
-
Diabetes increases the odds of developing shingles by 38%.
-
Patients with chronic kidney or heart disease experience more severe disruptions to daily life during an outbreak.
-
43% of Indian adults aged 50–70 who previously had shingles reported pain so severe it disrupted their daily routines.
The “Prevention Gap”: Awareness vs. Access
A comprehensive survey of 752 Indian adults, part of a larger global study commissioned by GSK and released this week, revealed a startling disconnect. While the risks are climbing, doctor-patient conversations regarding adult vaccination are lagging. Nearly half of at-risk Indians with chronic conditions have overlooked shingles prevention entirely.
“Shingles evolves from an individual health issue to a significant socio-economic strain if left unaddressed,” say leading clinicians. When a senior is sidelined by PHN, the burden often falls on family caregivers, impacting household productivity and increasing healthcare spending on pain management.
The Shield: Shingrix and Vaccine Efficacy
In 2023, the landscape of prevention changed with the Indian launch of Shingrix, a recombinant (non-live) vaccine. Unlike earlier live-virus versions, this two-dose series offers:
-
Over 90% efficacy in preventing shingles and PHN in adults over 50.
-
Long-term protection, with data showing nearly 80% efficacy sustained up to 11 years post-vaccination.
-
Safety for the immunocompromised, as it does not contain a live virus.
“These findings instill confidence for policymakers to include shingles vaccination in public health plans,” says Dr. Rashmi Hegde, Executive Vice President of Medical Affairs at GSK India.
Barriers to Protection: The Cost of Prevention
Despite the clinical success of the vaccine, uptake in India remains stalled by two primary hurdles: cost and policy.
Currently, shingles vaccination is not part of India’s Universal Immunization Programme (UIP). This means there is no public procurement, and the vaccine is only available in the private market. With a price tag of approximately Rs. 10,000 to 12,000 for the full two-dose course, it remains financially out of reach for a large portion of the population who lack comprehensive health insurance.
Furthermore, India’s public health narrative has historically focused on pediatric immunization. Experts argue that adult vaccination strategies need a radical overhaul to match the realities of an ageing nation.
“We use seatbelts to protect against the ‘what if’ of an accident,” says one public health advocate. “Vaccination for shingles serves the same purpose for our internal biology—it fortifies the body against a latent threat we know is already there.”
Limitations and the Road Ahead
While the recent survey data provides a vital snapshot, some experts note that because the study was commissioned by a vaccine manufacturer, it is essential to cross-reference findings with independent epidemiological data.
While the lifetime risk of shingles is roughly one in three globally, not every carrier will experience reactivation. Furthermore, for those who do develop a rash, early intervention with antiviral medications (within 72 hours) can reduce severity. However, antivirals do not always prevent the onset of the dreaded long-term nerve pain (PHN), which remains the strongest argument for vaccination.
As India moves forward, the medical community is calling for:
-
Increased Physician Proactivity: Doctors treating diabetics and cardiac patients must integrate vaccination discussions into routine visits.
-
Policy Integration: Evaluating the cost-benefit of including shingles shots in government health schemes for the most vulnerable.
-
Public Education: Moving beyond “awareness” to “action,” helping seniors understand that the “shocks” they feel aren’t just a part of getting older—they are preventable.
For adults over 50, the advice from specialists like Dr. V. Ramasubramanian is clear: don’t wait for the rash. Consult a healthcare provider about the two-dose vaccine schedule (typically administered 2–6 months apart) to ensure the “second act” of the chickenpox virus never takes center stage.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- Economic Context: Economic Times Health (March 2, 2026) – “Shingles risk rises with ageing India.”