Published: March 7, 2026
In an era where “low-fat” labels once dominated grocery aisles, a different dietary culprit has emerged as a primary driver of the modern metabolic crisis. New clinical evidence and epidemiological data released this week underscore a harrowing reality: the fructose found in sugar-sweetened beverages (SSBs) is not just adding calories—it is fundamentally reengineering human metabolism.
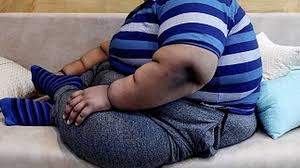
Recent studies, highlighted in a March 5, 2026, report by Times Now, confirm that excessive fructose intake is a direct catalyst for nonalcoholic fatty liver disease (NAFLD), obesity, and type 2 diabetes. With added sugars like high-fructose corn syrup (HFCS) now accounting for roughly 15% of the average Western caloric intake, medical experts are sounding the alarm on a “silent epidemic” that begins in the gut and ends in chronic organ failure.
The Metabolic “Bypass”: Why Fructose is Different
To understand why a soda is more damaging than a potato, one must look at the liver. While nearly every cell in the human body can use glucose for energy, fructose is processed almost exclusively by the liver.
When we consume glucose, the body uses what it needs and stores the rest as glycogen. However, fructose bypasses the “regulatory gatekeepers” of glycolysis. Research shows that fructose is rapidly metabolized by an enzyme called fructokinase C. This process is aggressive; it depletes the cell’s energy currency (ATP) and generates uric acid as a byproduct.
“Fructose uniquely precipitates hepatic fat via ATP depletion and uric acid,” explains Manal F. Abdelmalek, MD, a specialist from Duke University. This “metabolic flooding” forces the liver to convert the excess sugar directly into fat—a process known as de novo lipogenesis.
Key Findings from Recent Research:
-
Rapid Onset: Animal studies demonstrate that high-fructose diets can induce fatty liver in as little as 8 to 24 weeks, even when total calorie intake is not excessive.
-
Human Impact: In a pivotal six-month trial, participants drinking sugary beverages saw an increase in liver fat of up to 143% compared to those drinking water or diet sodas.
-
Pediatric Reversal: Encouragingly, a nine-day study of children showed that simply restricting fructose—without reducing total calories—significantly lowered liver fat and slowed fat production.
The Uric Acid Connection and Gut Health
The damage isn’t limited to fat storage. The spike in uric acid caused by fructose metabolism triggers mitochondrial stress. This stress inhibits the enzymes responsible for burning fat (such as aconitase-2), effectively locking the “fat-burning furnace” while the “fat-making factory” runs at triple speed.
Furthermore, new insights from Penn Medicine suggest the gut acts as a primary shield that eventually fails. Zoltan Arany, MD, PhD, notes that while the small intestine can process small amounts of fructose, sugary drinks provide such a high, rapid dose that the gut’s defenses are overwhelmed. This causes “leaky gut,” allowing endotoxins to spill into the bloodstream and inflame the liver.
A Growing Public Health Crisis
The correlation between the rise of high-fructose corn syrup and the prevalence of NAFLD is stark. National Health and Nutrition Examination Survey (NHANES) data reveals that NAFLD now affects 25-30% of all adults globally.
| Condition | Risk Increase from 1 Sugary Drink Daily |
| Type 2 Diabetes | 26% |
| Heart Disease | 35% |
| Fatty Liver (NAFLD) | Significantly higher (dose-dependent) |
The disparity is even more pronounced among youth and ethnic minority groups, who statistically consume the highest volumes of SSBs. Frank Hu, MD, PhD, of the Harvard T.H. Chan School of Public Health, is blunt about the solution: “Sugar-sweetened beverages urgently need public health curbs to stem metabolic diseases.”
Expert Perspectives: The Call for Policy Change
For years, the beverage industry argued that “a calorie is a calorie.” Modern science has largely debunked this in the context of fructose.
“Diets high in fructose from sucrose and HFCS are likely major NAFLD risk factors, activating lipogenesis while impairing oxidation,” says Richard J. Johnson, MD, of the University of Colorado Anschutz Medical Campus.
Experts are now calling for “sugar taxes” and clearer labeling of hidden HFCS in processed foods. They emphasize that while the fructose in a whole apple is buffered by fiber and antioxidants—slowing absorption and protecting the liver—the “liquid fructose” in sodas offers no such protection.
Limitations and Counterpoints
While the evidence is robust, some nuances remain. Short-term trials (under four weeks) occasionally show no significant difference in liver fat between fructose and glucose, suggesting that the damage of NAFLD is a slow, cumulative process that requires months or years of habitual consumption to manifest.
Additionally, genetics play a role. Variants in the PNPLA3 gene can make certain individuals far more susceptible to liver fat buildup than others, even at similar levels of sugar intake.
Practical Advice: How to Protect Your Liver
The good news is that the liver is remarkably resilient. Reducing fructose intake can yield rapid improvements in metabolic markers.
-
Prioritize “Water First”: Replace sodas and “fruit cocktails” with sparkling water, unsweetened tea, or water infused with real fruit slices.
-
Read Labels Diligently: Look for “High Fructose Corn Syrup,” “Agave Nectar,” and “Sucrose.” Aim to keep added sugars below 25g per day, per World Health Organization (WHO) guidelines.
-
Don’t Fear Whole Fruit: The fiber in whole fruit prevents the fructose “spike” that overwhelms the liver.
-
Boost Activity: Physical exercise increases the body’s ability to oxidize (burn) fat, helping to clear the liver of accumulated triglycerides.
-
Talk to Your Doctor: If you have a history of high sugar intake, ask about a uric acid test or a non-invasive liver ultrasound.
As the research evolves, the message remains clear: our bodies were not designed to process the massive, liquid sugar loads of the modern diet. Protecting the liver may be as simple—and as difficult—as putting down the can.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Times Now News. Excess Fructose May Trigger Fatty Liver, Obesity and Diabetes Risk. Published March 5, 2026