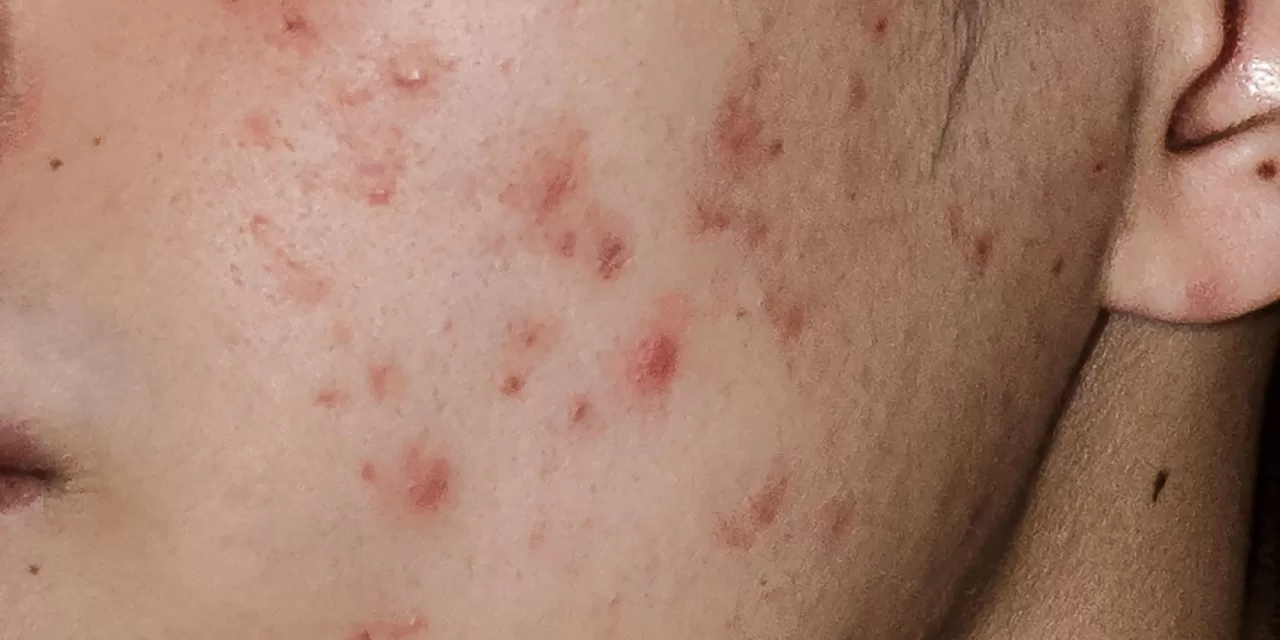
A groundbreaking study by researchers at the Massachusetts Institute of Technology (MIT) has uncovered new insights into the mysterious onset of teenage acne, revealing that the bacteria living on our faces play a pivotal role in this common skin condition. Published recently in Cell Host & Microbe, the research could revolutionize how acne is treated in the future by focusing on the skin’s microbiome during adolescence.
The Skin Microbiome: A Hidden World on Our Faces
Our skin is home to a complex ecosystem of microbes, with two bacteria-Cutibacterium acnes (formerly Propionibacterium acnes) and Staphylococcus epidermidis-dominating the facial landscape. While scientists have long suspected these bacteria influence conditions like acne and eczema, the timing and nature of their colonization remained unclear until now.
MIT researchers tracked the skin microbiomes of 30 children and 27 parents over time, sequencing individual bacterial cells. They discovered that during early teenage years-when oil production surges-new strains of C. acnes rapidly appear and establish themselves. These strains tend to persist for years, creating a stable, personalized bacterial signature unique to each individual.
Why Adolescence Is a Critical Window
This stability of bacterial strains is a double-edged sword. Once adulthood is reached, the skin microbiome becomes relatively fixed, making it harder for new bacterial strains, including potentially beneficial probiotics, to take root.
Dr. Tami Lieberman, senior author of the study and associate professor at MIT, explains, “If we had a strain that we knew could prevent acne, these results would suggest we should apply it early, during the transition to adulthood, so that it has a better chance to settle in.”
In essence, adolescence is like fertile soil for the skin’s bacteria. Introducing acne-preventing probiotics during this period could help “plant seeds” that promote healthier skin long-term.
The Role of Staphylococcus epidermidis
Unlike C. acnes, Staphylococcus epidermidis strains are more transient, living less than two years on average and varying greatly even among people living in the same household. The reasons behind this difference are not fully understood but may involve individual skincare habits, genetics, or bacterial competition.
Implications for Future Acne Treatments
Current acne therapies often rely on antibiotics or retinoids, which can irritate skin and offer limited long-term relief. This new research opens the door to innovative treatments that manipulate the skin microbiome during the critical adolescent window.
Several companies are already exploring topical probiotics for acne, and this study provides a scientific basis for applying such treatments early, before the skin’s bacterial community becomes set.
For teenagers struggling with acne, this research offers hope that more personalized, microbiome-based therapies could soon be available-treatments that work with the skin’s natural ecosystem rather than against it.
Looking Ahead
The MIT team’s next goal is to determine how the timing of bacterial colonization affects long-term skin health and to use this knowledge to design targeted interventions.
“We’re each walking around with a unique skin microbiome, shaped by early events in our lives. If we can understand that better, we may be able to guide it toward healthier outcomes,” Dr. Lieberman said.
Disclaimer
This article summarizes findings from a recent scientific study and is intended for informational purposes only. It does not constitute medical advice. Individuals experiencing skin issues should consult a qualified dermatologist or healthcare professional for diagnosis and treatment tailored to their specific needs.
Citations: