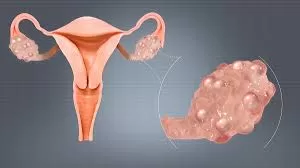
NEW DELHI — For millions of women living with Polycystic Ovary Syndrome (PCOS), the battle is often framed by visible symptoms: stubborn acne, unexpected weight gain, or the frustration of irregular menstrual cycles. However, a growing body of clinical evidence and expert consensus suggests that the most debilitating symptoms may be the ones hidden from view.
New insights from leading endocrinologists and gynecologists indicate that the hormonal fluctuations inherent to PCOS are fundamentally linked to significant emotional disturbances, including acute anxiety, irritability, and clinical depression. Experts warn that these psychological components are frequently sidelined in clinical settings, leaving patients to struggle with “unexplained” emotional instability.
The Biological Link: Androgens, Insulin, and the Brain
PCOS is a complex endocrine disorder affecting approximately 8% to 13% of reproductive-aged women worldwide, according to the World Health Organization (WHO). While it is often treated as a reproductive issue, its impact on the central nervous system is profound.
At the heart of the emotional turbulence are two primary physiological drivers: Hyperandrogenism (excessive male-type hormones like testosterone) and Insulin Resistance.
“Hormonal imbalances, including elevated androgen levels and insulin resistance, can make women feel unusually anxious, irritable, or emotionally unstable even without a clear reason,” says Dr. Neelam Suri, Senior Consultant in Obstetrics and Gynaecology at Indraprastha Apollo Hospitals.
These hormones do not act in isolation; they directly interfere with the brain’s delicate chemistry. Specifically, high androgen levels can disrupt the production and reception of serotonin, often dubbed the “feel-good” neurotransmitter.
Dr. Anjana Singh, Director of Obstetrics and Gynaecology at Fortis Hospital Noida, explains that when insulin resistance—present in up to 70% of PCOS cases—enters the equation, it can trigger low-grade systemic inflammation. This inflammation can affect the brain’s emotional processing centers, further exacerbating mood swings.
The “Cycle of Distress”: Physical Symptoms and Mental Health
The relationship between PCOS and mental health is not merely biological; it is also psychosocial. The physical manifestations of the syndrome often create a feedback loop that degrades emotional well-being.
-
Hirsutism and Self-Esteem: Excessive hair growth on the face or body can lead to body dysmorphia and social withdrawal.
-
Infertility Fears: The irregular ovulation associated with PCOS often causes significant “procreational distress” for those wishing to start families.
-
The Weight Paradox: Insulin resistance makes weight loss difficult, leading to frustration and a higher prevalence of eating disorders compared to the general population.
“The physical symptoms of the disorder can impact self-esteem and create a cycle where hormonal imbalance and emotional stress reinforce each other,” experts note. When a patient feels distressed about their appearance or health, the resulting cortisol (stress hormone) spike can, in turn, worsen insulin resistance, deepening the hormonal divide.
Shifting the Treatment Paradigm: Beyond the Birth Control Pill
Historically, the standard of care for PCOS has focused heavily on oral contraceptives to regulate periods or Metformin to manage blood sugar. While these remain vital tools, experts are calling for a more holistic, “neuro-endocrine” approach.
1. Nutritional Stabilization
Stabilizing blood sugar is a primary defense against mood crashes. Specialists recommend a diet rich in whole foods—complex carbohydrates, lean proteins, and healthy fats—while strictly limiting refined sugars. This prevents the “insulin spikes” that can trigger irritability and fatigue.
2. Physical Intervention
Regular physical activity (30 to 40 minutes daily) serves a dual purpose. Beyond managing weight, exercise triggers the release of endorphins, which act as natural stress-fighters. Data suggests that consistent resistance training can also improve insulin sensitivity more effectively than cardio alone in some PCOS patients.
3. Psychological Integration
Cognitive Behavioral Therapy (CBT) is increasingly recommended as a frontline treatment for PCOS-related anxiety. By addressing negative thought patterns associated with the condition, patients can break the psychological cycle of the “PCOS blues.”
Limitations and Counterarguments: A Nuanced View
While the link between PCOS and mood is strong, researchers caution against attributing all emotional distress solely to hormones. External factors—such as socioeconomic stress, sleep apnea (common in PCOS), and vitamin deficiencies (like Vitamin D or B12)—also play significant roles.
Furthermore, some critics in the medical community argue that over-pathologizing “mood swings” might lead to the over-prescription of antidepressants without first addressing the underlying metabolic issues. A balanced diagnostic approach is essential to ensure that a patient’s emotional state is viewed through a multi-dimensional lens.
Looking Ahead: The Importance of Early Intervention
The consensus among healthcare providers is clear: persistent emotional instability should not be dismissed as “just stress,” especially when it co-occurs with irregular cycles.
“Timely diagnosis and a combination of medical care, lifestyle changes, and emotional support can help women manage the condition and improve their overall quality of life,” says Dr. Suri. For the woman navigating the complexities of PCOS, understanding that her anxiety has a biological basis can be the first step toward reclaiming her mental agency.
As research continues into the “gut-brain-ovary axis,” the medical community is hopeful that future treatments will move beyond symptom management and toward true hormonal harmony.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References and Sources
- https://www.daijiworld.com/news/newsDisplay?newsID=1309159