NEW DELHI, December 4, 2025
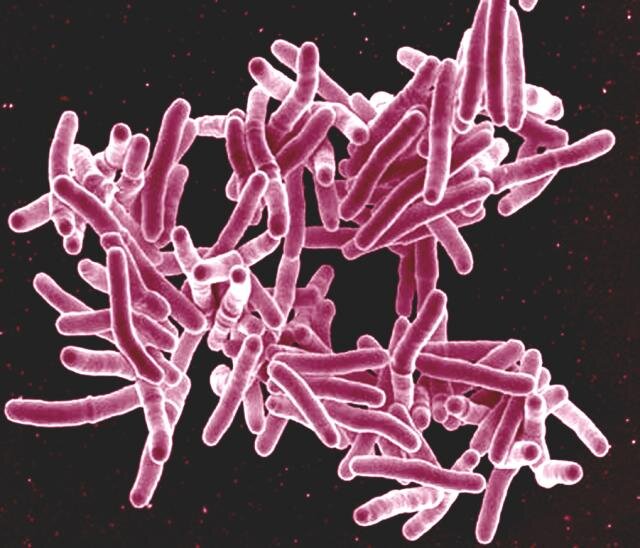
In a groundbreaking discovery that could reshape the treatment landscape for one of the world’s deadliest infectious diseases, researchers at the Indian Institute of Technology (IIT) Bombay have identified a novel “survival shield” used by tuberculosis (TB) bacteria. The study, published this week in the prestigious journal Chemical Science, reveals that Mycobacterium tuberculosis does not just rely on genetic mutations to resist drugs; instead, it physically hardens its outer coating to block antibiotics from entering.
This finding offers a critical clue into why TB treatment requires months of intensive medication and why the disease often relapses, potentially paving the way for faster, more effective therapies.
The “Sleeping” Enemy
Tuberculosis remains a global health crisis. According to World Health Organization (WHO) data, an estimated 10.7 million people developed TB in 2024, claiming 1.23 million lives. India continues to bear a significant portion of this burden, with over 2.71 million cases reported last year.
While standard antibiotics effectively kill actively dividing bacteria, a sub-population of the bacteria often enters a dormant or “sleep” state (latency). In this state, they become “phenotypically tolerant”—meaning they are not genetically resistant to the drugs, but the drugs simply stop working on them. Until now, the precise mechanical reason for this tolerance was not fully understood.
“The same drug that worked well in the early stage of the disease would now be needed at a much higher concentration to kill the dormant or persistent TB cells,” explained Prof. Shobhna Kapoor, lead researcher from the Department of Chemistry at IIT Bombay. “This change was not caused by genetic mutations, which usually explain antibiotic resistance.”
Decoding the Lipid Shield
The study, conducted in collaboration with Prof. Mibel Aguilar and researchers from Monash University, Australia, focused on the bacterial cell membrane—a complex barrier made primarily of fats, or lipids.
The team grew TB bacteria in two distinct phases: an active phase (mimicking acute infection) and a dormant phase (mimicking latent infection). When exposed to four common antibiotics—rifabutin, moxifloxacin, amikacin, and clarithromycin—the dormant bacteria proved remarkably resilient. It took drug concentrations two to ten times higher to stop their growth compared to the active bacteria.
By analyzing over 270 distinct lipid molecules in the bacterial membranes, the researchers discovered a striking structural transformation:
-
Active Bacteria: Possessed “loose,” fluid membranes that allowed antibiotics to penetrate easily.
-
Dormant Bacteria: Remodeled their membranes into rigid, tightly packed structures. This hardening effectively sealed the cell, acting as a physical shield against the drugs.
“People have studied TB from the protein point of view for decades,” said Prof. Kapoor. “But lipids were long seen as passive components. We now know they actively help the bacteria survive and resist drugs.”
Specifically, the study found that rifabutin, a potent antibiotic, could easily cross the fluid membrane of an active cell but was blocked by the solidified defense of a dormant one.
Expert Perspectives
The distinction between “genetic resistance” and “phenotypic tolerance” is a critical one for clinicians. Dr. Rajesh Gupta, a senior pulmonologist and infectious disease specialist not involved in the study, highlighted the clinical relevance of these findings.
“In clinical practice, we often see patients who appear to be cured but suffer a relapse months or years later,” Dr. Gupta noted. “We have long known that ‘persister’ cells survive the initial antibiotic onslaught, but we lacked a clear target. If this study suggests that the membrane’s physical state is the gatekeeper, it shifts our focus from just finding new poisons to finding ways to ‘unlock’ the door so the poison can get in.”
Independent researchers emphasize that targeting the bacterial membrane has historically been difficult due to its complexity. However, understanding the specific lipid changes offers a roadmap for “adjuvant” therapies—drugs that don’t kill the bacteria themselves but make them vulnerable to existing antibiotics.
Implications for Public Health
The implications of this research are far-reaching. The current standard of care for TB involves a grueling 6-month regimen of multiple antibiotics. For drug-resistant TB, treatment can last up to two years.
The IIT Bombay team suggests a new therapeutic strategy: Membrane-Loosening Agents.
“Even old drugs can work better if combined with a molecule that loosens the outer membrane,” Prof. Kapoor stated.
If researchers can develop a safe molecule that reverses this membrane hardening—turning the “rigid” shield back into a “fluid” one—it could:
-
Shorten treatment duration by killing dormant bacteria faster.
-
Prevent relapse by eradicating the reservoirs of latent bacteria.
-
Revitalize older antibiotics that have become less effective against persistent strains.
Limitations and Future Directions
While the study provides a compelling mechanism using Mycobacterium smegmatis (a surrogate model for TB) and lipid analysis, the transition to clinical application will take time. Researchers must now identify specific molecules that can safely disrupt this lipid shield in the human body without damaging human cells. Furthermore, clinical trials will be needed to verify if “membrane looseners” translate to faster cure rates in actual patients.
For now, the discovery stands as a significant leap forward in the biological understanding of an ancient foe. As the world aims to eliminate TB by 2030, uncovering the bacterium’s secret survival strategies is the first step toward defeating it for good.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Primary Study: Menon, A. P., Lee, T., Aguilar, M., & Kapoor, S. (2024). Decoding the role of mycobacterial lipid remodelling and membrane dynamics in antibiotic tolerance. Chemical Science. DOI: 10.1039/D4SC06618A
-
Additional Context: “IIT Bombay study shows how TB bacteria shield themselves from antibiotics,” Nagaland Tribune, Dec 3, 2025.