Published: March 5, 2026
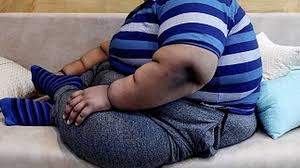
NEW DELHI — A staggering global health failure is unfolding as the World Obesity Federation (WOF) warns that most nations, including India, are now “off track” to meet the 2030 international mandate to halt the rise of childhood obesity. Originally set for 2025 and subsequently extended to 2030, the target remains elusive. New data released on World Obesity Day reveals that by 2040, India alone could see 20 million children living with obesity, while 120 million school-age children worldwide are projected to exhibit early markers of chronic conditions like hypertension and cardiovascular disease.
A Growing Crisis: The Numbers in India
The World Obesity Atlas 2026, published Wednesday, paints a sobering picture of the pediatric health landscape. In India, the crisis is bifurcated across age groups: as of 2025, approximately 14.9 million children aged 5–9 and over 26.4 million adolescents aged 10–19 were classified as overweight or obese.
By 2040, these figures are expected to culminate in a total of 56 million Indian children living with overweight and obesity. This trajectory places India second only to China in the total number of children affected by high Body Mass Index (BMI).
The Top 10 Contributors
According to the Atlas, just ten countries account for over 200 million school-age children with high BMI. By the close of 2025, three nations emerged as the primary epicenters of this epidemic:
-
China: 62 million (high BMI); 33 million (obesity)
-
India: 41 million (high BMI); 14 million (obesity)
-
United States: 27 million (high BMI); 13 million (obesity)
From Weight to Wellness: The Medical Implications
Obesity is not merely a matter of weight; it is a precursor to metabolic dysfunction that was once seen primarily in adults. The WOF report highlights a significant rise in “disease indicators” among Indian youth aged 5–19.
Between 2025 and 2040, the following complications are projected to increase substantially in India:
-
Hypertension: Rising from 2.99 million to 4.21 million cases.
-
Hyperglycemia (High Blood Sugar): Increasing from 1.39 million to 1.91 million.
-
High Triglycerides: Projected to hit 6.07 million.
-
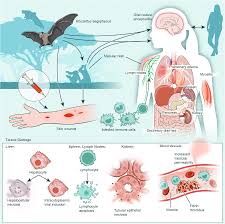
MASLD: Metabolic dysfunction-associated steatotic liver disease (formerly NAFLD) is expected to affect 11.88 million children.
“We are seeing adult-onset diseases in pediatric clinics with alarming frequency,” says Dr. Ananya Sharma, a pediatric endocrinologist not involved in the study. “When a ten-year-old presents with the liver profile of a 50-year-old, we are looking at a public health emergency that will strain our medical infrastructure for decades.”
The Root Causes: Lifestyle and Policy Gaps
The Atlas identifies several systemic failures contributing to the rise. In India, the data suggests a “perfect storm” of low physical activity and nutritional gaps:
-
Inactivity: 74% of adolescents (11–17 years) fail to meet recommended physical activity levels.
-
Nutritional Support: Only 35.5% of school-age children receive school meals.
-
Early Intervention: 32.6% of infants experience sub-optimal breastfeeding in their first five months.
-
Sugar Consumption: Children aged 6–10 consume up to 50 ml of sugary drinks daily, contributing to caloric surplus without nutritional value.
Expert Commentary: A Call for Policy Reform
Johanna Ralston, Chief Executive of the World Obesity Federation, issued a blunt critique of the current global response. “The increase in childhood obesity worldwide shows we have failed to take seriously a disease that affects one in five children,” Ralston stated.
She emphasized that the solution lies in “healthy environments” rather than individual blame. Ralston advocated for:
-
Sugar-sweetened beverage taxes to curb consumption.
-
Marketing restrictions on unhealthy foods targeting children.
-
Enhanced monitoring beginning in primary care settings.
“There is no reason to hesitate,” Ralston added. “It is not right to condemn a generation to chronic and potentially fatal non-communicable diseases.”
Limitations and Counter-Perspectives
While the Atlas provides a comprehensive data set, some public health experts caution that BMI remains an imperfect proxy for health. BMI does not distinguish between muscle mass and fat, nor does it account for ethnic variations in body composition—a factor particularly relevant in South Asian populations where “thin-fat” phenotypes (low BMI but high visceral fat) are common.
Furthermore, critics of aggressive taxation policies argue that without subsidized access to fresh produce, “sugar taxes” may disproportionately affect low-income families without necessarily improving nutritional quality.
Public Health Outlook
The global prevalence of obesity and overweight among those aged 5–19 has climbed from 14.6% in 2010 to 20.7% today. By 2040, the WOF predicts 507 million children worldwide will be affected. For parents and educators, the message is clear: the window for prevention is narrowing. Integrating physical movement into the school day and advocating for clearer “front-of-pack” labeling on processed foods are no longer optional—they are essential interventions.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
Most nations, including India, off track to meet 2030 target to halt childhood obesity