February 15, 2026
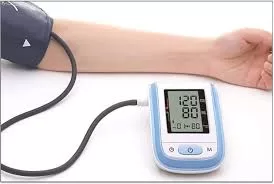
NEW DELHI — The foundational ritual of hypertension management—swallowing a pill every morning—may soon become a relic of the past. A landmark review published in The Lancet suggests that the medical community is on the precipice of the most significant shift in blood pressure treatment in decades. Emerging long-acting injectable therapies, currently in late-stage clinical trials, demonstrate the potential to control hypertension with as few as two doses per year, offering a high-tech solution to the age-old problem of medication non-adherence.
The Adherence Barrier: Why Pills Fail
For over half a century, the frontline defense against high blood pressure has been a rotating cast of daily oral medications: ACE inhibitors, beta-blockers, and diuretics. While these drugs are biologically effective, they rely on a fragile human variable: consistency.
“We have excellent tools, but they only work if patients take them,” says Dr. Elena Rossi, a cardiovascular researcher not involved in the Lancet review. “Between ‘treatment fatigue’—the psychological exhaustion of taking daily meds—and the complex regimens required for patients who also have diabetes or high cholesterol, adherence often crumbles.”
The statistics are sobering. According to the World Health Organization (WHO), an estimated 1.28 billion adults globally live with hypertension, yet fewer than one in four have their condition under control. In India, the 2023 ICMR-INDIAB study revealed that 315 million people—roughly 35% of the population—are hypertensive. When patients miss doses, their blood pressure fluctuates, significantly increasing the risk of “silent killers” like stroke and myocardial infarction (heart attack).
Turning Off the Tap: The Science of RNA Interference
Unlike traditional pills that neutralize hormones already circulating in the blood, the new generation of injectables—specifically small interfering RNA (siRNA) agents—works “upstream.”
One of the most watched candidates is Zilebesiran, currently in Phase 3 trials by Roche and Alnylam. Zilebesiran targets the liver to suppress the production of angiotensinogen, a precursor protein that the body eventually turns into a potent vessel-constricting hormone. By “silencing” the gene responsible for this protein, a single injection can keep blood pressure lowered for six months.
Other promising therapies include:
-
Ziltivekimab: Developed by Novo Nordisk, this agent targets inflammatory pathways that contribute to vascular damage and hypertension.
-
Aldosterone Synthase Inhibitors: These focus on more precisely regulating aldosterone, the hormone responsible for salt and water retention.
“The shift from ‘reactive’ daily dosing to ‘proactive’ semi-annual dosing is akin to the transition from manual insulin injections to automated pumps, or daily birth control to long-acting implants,” explains Dr. Rossi. “It removes the burden of memory from the patient.”
The Cost of Innovation: A Barrier to Access?
While the clinical promise is immense, public health experts warn of a looming “equity gap.” The primary concern is affordability, particularly in low- and middle-income countries where the burden of hypertension is highest.
History provides a cautionary tale. Inclisiran, an injectable cholesterol-lowering drug introduced in India in 2024, carries an annual price tag of ₹1.8 lakh to ₹2.4 lakh ($2,100–$2,800 USD). For a condition as prevalent as hypertension, such pricing would make the treatment a luxury rather than a public health tool.
“If these injections cost fifty times more than a month’s supply of generic amlodipine, they won’t solve the global crisis,” says Arishta Sen, a public health policy analyst. “To truly transform outcomes, these must be accessible within public health systems, not just private boutiques.”
Safety and Long-Term Considerations
Because these drugs stay in the system for months, they present a unique clinical challenge: you cannot “un-take” the medicine. If a patient experiences an adverse reaction or an extreme drop in blood pressure (hypotension) after an injection, doctors must manage those effects over a long duration.
Furthermore, current trials primarily involve stable populations. Experts stress the need for “real-world” data across diverse ethnicities and age groups, especially the elderly, who may react differently to long-term hormonal suppression.
What This Means for You
For the average person managing high blood pressure, these developments do not mean you should toss your pillbox today.
-
Current Management: Daily oral medication remains the gold standard of care until these injectables receive final regulatory approval (expected in the next 18–24 months for leading candidates).
-
Future Planning: Patients who struggle with side effects or forgetfulness should discuss these emerging “long-acting” options with their cardiologists to see if they might be candidates for clinical trials or early-access programs.
-
Lifestyle Foundation: No injection replaces the need for a low-sodium diet, regular exercise, and stress management, which work synergistically with any pharmacological intervention.
As we move toward a “twice-a-year” model, the goal of cardiology is shifting from merely treating a number on a cuff to providing a seamless, “set-it-and-forget-it” shield against the world’s leading cause of premature death.
References
- https://www.daijiworld.com/news/newsDisplay?newsID=1306487
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.