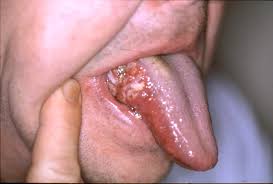
NEW DELHI — A comprehensive new analysis of oncological data has revealed a sobering reality for public health in India: the synergistic use of alcohol and smokeless tobacco is now responsible for approximately 62% of all mouth cancer cases in the country. The findings, emerging from a meta-analysis of regional cancer registries and clinical studies, underscore a growing epidemic that health experts warn is being driven by cultural normalization and a lack of awareness regarding “combined risk factors.”
While the link between smoking and lung cancer is well-established in the public consciousness, this latest data shifts the spotlight to the devastating impact of oral tobacco products—such as betel quid, khaini, and gutka—especially when paired with alcohol consumption. As India continues to report some of the highest rates of oral cavity cancer globally, medical professionals are calling for immediate policy interventions and a fundamental shift in how the public perceives these “everyday” habits.
The Power of Two: Understanding Synergistic Risk
The crux of the report lies in the concept of “synergy.” Medical researchers have long observed that while tobacco and alcohol are independent carcinogens, their combined effect is not merely additive—it is multiplicative.
“When a person uses smokeless tobacco, the chemicals cause micro-abrasions in the oral mucosa,” explains Dr. Ananya Sharma, a head and neck oncologist not involved in the study. “Alcohol then acts as a solvent, making the lining of the mouth more permeable. This allows the potent carcinogens in tobacco, such as tobacco-specific nitrosamines (TSNAs), to penetrate deeper into the tissue, triggering cellular mutations at an accelerated rate.”
According to the data, individuals who regularly engage in both habits face a risk of developing oral squamous cell carcinoma that is significantly higher than those who use only one or the other. In many rural and urban pockets of India, where the use of paan with tobacco is a social ritual often accompanied by locally brewed or branded alcohol, the biological “perfect storm” is created daily.
Statistical Reality: A Heavy Burden
The scale of the crisis is reflected in the numbers. India accounts for nearly one-third of the global burden of oral cancer. The study highlights that:
-
62% of cases are directly attributable to the combined use of alcohol and smokeless tobacco.
-
Early Onset: There is a worrying trend of oral cancer appearing in patients in their 30s and 40s, a demographic traditionally considered young for such diagnoses.
-
Gender Dynamics: While historically higher in men, the incidence among women in certain states is rising due to the increased social acceptance of smokeless tobacco use.
The Cultural Hurdle
One of the primary challenges in combating these figures is the deep-seated cultural integration of smokeless tobacco. Unlike cigarettes, which carry a heavy social stigma and are restricted by “no smoking” zones, smokeless tobacco is often used discreetly and is deeply woven into the social fabric of both rural and urban India.
“We are fighting a battle against tradition as much as we are fighting a disease,” says Rajeshwari Sinha, a public health advocate. “Many users do not even view gutka or khaini as ‘drugs’ or serious health hazards. When you add alcohol to the mix, which is often used as a stress-reliever in high-pressure labor environments, the health risks are completely overshadowed by immediate social or physical cravings.”
Public Health Implications and the Path Forward
The implications for India’s healthcare infrastructure are profound. Mouth cancer treatments, which often involve disfiguring surgeries, radiation, and chemotherapy, place an immense financial burden on families and the state. Furthermore, the survival rate for oral cancer in India remains lower than in Western nations, primarily because cases are often detected at advanced stages (Stage III or IV).
Experts suggest a multi-pronged approach to bend the curve:
-
Stricter Enforcement: While several Indian states have banned the sale of gutka, enforcement remains inconsistent, and “twin-pack” marketing (selling tobacco and flavoring separately) often bypasses legal hurdles.
-
Targeted Screening: Implementing mandatory oral screenings during routine dental or primary care visits for high-risk demographics.
-
Publicity Campaigns: Shifting the narrative from “tobacco causes cancer” to “tobacco and alcohol together are a lethal combination.”
Limitations and Counterarguments
While the 62% figure is a powerful indicator, some researchers argue that other factors deserve equal attention. Poor oral hygiene, chronic irritation from jagged teeth, and nutritional deficiencies (specifically a lack of antioxidants from fruits and vegetables) also play significant roles in the Indian context.
Additionally, some industry proponents argue that the focus should remain on “harm reduction” rather than outright bans, suggesting that the black market created by bans can lead to the consumption of even more toxic, unregulated products. However, the oncological community remains firm: there is no “safe” level of tobacco or alcohol when it comes to the delicate tissues of the mouth.
What This Means for You
For the average consumer, the message is clear: the occasional use of smokeless tobacco is not a harmless habit, and its dangers are magnified exponentially by alcohol.
“Prevention is the only sustainable cure for oral cancer,” says Dr. Sharma. “If you use these substances, regular self-examinations—looking for white patches (leukoplakia), red sores that don’t heal, or unusual lumps—can be life-saving. But the best defense is cessation.”
As India strives to meet its global health targets, addressing the 62% of mouth cancer cases linked to these two common substances remains one of the most urgent priorities for the coming decade.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
NDTV Health: Data reporting on the 62% mouth cancer correlation (Source: Press Trust of India/Research findings).