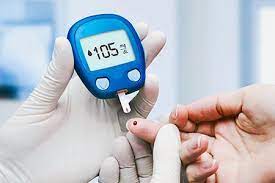
Diabetes is commonly understood as a disease directly caused by high sugar intake, but recent findings and expert insights reveal a spectrum of diabetes types—some of which have no direct connection to sugar. From diabetes insipidus to type 3c diabetes caused by pancreatic damage, these forms challenge conventional notions and highlight the complexity of glucose regulation disorders. Understanding these less-known types, their causes, and implications is vital for public health awareness and patient care.
Key Developments in Non-Sugar Diabetes Types
While type 1 and type 2 diabetes dominate public attention—both characterized primarily by dysfunction in insulin production or use—other diabetes forms exist that do not stem from sugar metabolism problems. Diabetes insipidus, for instance, is a rare disorder affecting the kidneys’ ability to conserve water, leading to excessive thirst and urination but not altering blood glucose levels.
Another important category is type 3c diabetes, which occurs when diseases like pancreatitis, cystic fibrosis, or pancreatic cancer damage the pancreas, resulting in both insulin deficiency and impaired digestion. There are also rare genetic forms such as Wolfram Syndrome, which present with diabetes as part of a complex syndrome affecting multiple organs.
Moreover, recent medical research has debunked the oversimplification that sugar intake alone causes diabetes. Instead, type 2 diabetes is chiefly linked to insulin resistance often driven by obesity, genetic predisposition, and lifestyle factors rather than direct sugar consumption.
Expert Perspectives and Commentary
Dr. Elmo Pretorius, an endocrinologist at Mediclinic Vergelegen, emphasizes, “Type 2 diabetes is primarily about how the body handles insulin, not directly about sugar. Insulin resistance related to abdominal obesity is the real culprit behind elevated blood sugar.” Dietician Ilsabé Spoelstra adds that “managing carbohydrate intake and weight can reduce the need for insulin in many cases, challenging the myth that sugar alone is to blame.” These insights support a more nuanced, evidence-based understanding that considers total calorie balance, body fat distribution, and genetics.
Medical experts also note that diabetes insipidus, while sharing the name diabetes, is mechanistically distinct from diabetes mellitus (types 1 and 2). It involves antidiuretic hormone deficiency or kidney resistance to it, with no effect on glucose metabolism, requiring entirely different management.
Context and Background on Diabetes Types
Globally, diabetes affects over 500 million people, predominantly type 2, which accounts for about 90-95% of cases and is strongly associated with metabolic syndrome and lifestyle factors. However, up to 1.5-2% of diabetes cases involve rare or secondary types such as MODY (Maturity Onset Diabetes of the Young) and type 3c diabetes. These require specialized diagnostic criteria because their treatments and prognoses differ significantly.
Secondary diabetes can arise from other medical conditions or medications, including steroid-induced diabetes and cystic fibrosis-related diabetes. Each subtype brings unique challenges for clinicians, underscoring the importance of personalized care strategies and accurate diagnosis.
Public Health Implications
Recognizing the diversity of diabetes types beyond sugar-centric views is critical for improving diagnosis, treatment, and prevention strategies. Public health campaigns that focus solely on reducing sugar intake may overlook other modifiable risk factors like obesity, physical inactivity, and genetic predispositions, which are equally or more important in preventing type 2 diabetes.
Awareness of rare diabetes forms facilitates early detection and management, potentially reducing complications associated with delayed or incorrect treatment. For instance, type 3c diabetes requires management of both insulin deficiency and pancreatic digestive insufficiency.
Limitations and Conflicting Views
Despite growing knowledge, some aspects remain under research. For example, the full pathophysiology of diabetes insipidus or the exact interplay between pancreatic damage and insulin dysfunction in type 3c diabetes is still being explored. There also exists debate about the potential long-term effects of artificial sweeteners on glycemic control, underscoring that no single intervention is universally effective.
Furthermore, emphasizing that sugar “does not cause diabetes” should not downplay the risk that excessive sugar consumption contributes indirectly via obesity and metabolic disruptions. Thus, balanced messages are essential.
Practical Takeaways for Readers
For those concerned about diabetes risk or management, the key is to focus on overall healthy eating, maintaining a healthy weight, and regular physical activity rather than demonizing sugar alone. Individuals with unusual diabetes symptoms or poor response to standard therapies should seek evaluation for rare or secondary diabetes types.
Understanding that diabetes is a complex disease with varied causes empowers patients to work effectively with healthcare providers for tailored prevention and treatment plans.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://scitechdaily.com/the-diabetes-that-has-nothing-to-do-with-sugar/