January 11, 2026
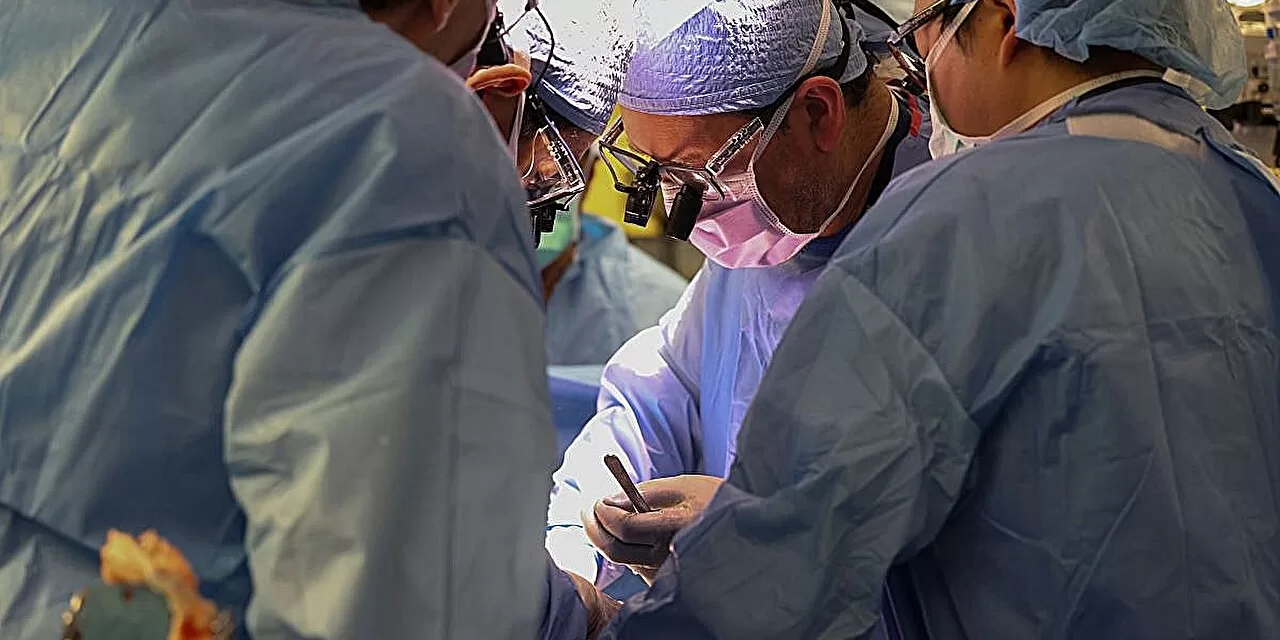
For decades, the success of a major operation was thought to rest almost entirely on two pillars: the skill of the surgical team and the underlying health of the patient. However, a groundbreaking study from the University of Manchester suggests a third, invisible factor may be at play: the time of day.
New research involving over 24,000 patients across the United Kingdom has revealed that heart surgeries beginning in the late morning are associated with an 18% higher risk of death from cardiovascular causes compared to those performed just a few hours earlier. The findings, published in the journal Anaesthesia, are sparking a global conversation about “circadian medicine” and whether the healthcare system should begin scheduling high-stakes procedures according to the human body clock.
Mapping the Risk: The 10:00 AM Pivot
The study, led by Dr. Gareth Kitchen, a Clinical Senior Lecturer at the University of Manchester, analyzed national healthcare data from 24,145 patients who underwent heart surgery in England, Wales, and Northern Ireland.
Researchers divided the surgical start times into three categories:
-
Early Morning: 7:00 AM to 9:59 AM
-
Late Morning: 10:00 AM to 12:59 PM
-
Afternoon: 1:00 PM onwards
The results were striking. While early-morning procedures were the most common—accounting for 47% of the total cases—those that began in the late-morning window (10:00 AM to 12:59 PM) showed a statistically significant increase in cardiovascular mortality.
Interestingly, the timing did not appear to impact non-fatal complications, such as infections or hospital readmission rates. The risk was specifically tied to cardiac-related death, suggesting that the heart’s resilience—or its vulnerability—may fluctuate throughout the day.
The Role of the Biological Clock
At the heart of this research is the circadian rhythm, the internal 24-hour clock that regulates almost every biological process in the human body, from hormone release to body temperature and heart rate.
“The body clock is not just a mental state; it is a cellular reality,” says Dr. Kitchen. “Our organs function differently at 8:00 AM than they do at 11:00 AM. This study suggests that aligning surgical intervention with these natural biological rhythms could open the door to a more personalized and precise level of medical care.”
The researchers hypothesize that the heart may be more susceptible to the stress of surgery—specifically the “ischemia-reperfusion injury” that occurs when blood flow is stopped and then restarted during a procedure—at certain times of the day.
Expert Perspectives: A Modest but Meaningful Shift
While an 18% increase in risk sounds alarming, medical experts urge patients to keep the numbers in perspective.
“We are talking about a modest increase in what is already a very low-risk environment,” explains Dr. Sarah Jenkins, a consultant cardiologist not involved in the Manchester study. “Most patients undergo heart surgery with excellent outcomes regardless of the hour. However, when you look at population-level data involving tens of thousands of people, these ‘modest’ risks translate into lives that could potentially be saved through better scheduling.”
Dr. Kitchen echoes this sentiment, noting that for the individual patient, the danger remains low. “The overall risk is small, and most people are unlikely to be affected. But for clinicians and hospital administrators, adjusting schedules is a virtually cost-free way to improve patient outcomes.”
Limitations and Alternative Explanations
As with any observational study, researchers must account for “confounding variables”—factors other than the time of day that might influence the results.
Critics and some members of the medical community have raised several points of caution:
-
Staff Fatigue: Is the increased risk due to the patient’s body clock, or the surgical team’s natural dip in energy as they approach the mid-day hours?
-
Case Complexity: Are more complex or emergency cases naturally pushed to later in the morning after the “routine” slots are filled?
-
Individual Variation: Everyone has a different “chronotype” (being a “morning lark” or a “night owl”). A 10:00 AM surgery might be optimal for one person but poorly timed for another.
The University of Manchester team acknowledged these factors, noting that while they adjusted for many patient-related risks, the human element of the surgical team is harder to quantify.
The Future: Personalized Surgery Schedules?
The ultimate goal of this research is not to cause panic among those scheduled for mid-morning procedures, but to refine how we approach surgery.
In the future, a patient’s “circadian profile” might be determined before they ever enter the hospital. By understanding whether a patient is genetically predisposed to function better in the morning or afternoon, surgeons could potentially tailor the timing of the operation to the patient’s specific biological peak.
“This is the beginning of a shift toward ‘personalized timing’ in medicine,” says Dr. Kitchen. “It’s a simple intervention: change the clock, change the outcome.”
What Should Patients Do?
For now, the advice from health authorities remains clear: Do not delay or reschedule a necessary heart surgery based on this study. The risks associated with delaying cardiac intervention far outweigh the 18% relative risk increase identified in the late-morning window.
Patients are encouraged to discuss any concerns with their surgical team, focusing on the team’s experience, the hospital’s success rates, and their personal recovery plan.
Reference Section
Primary Study:
-
Journal: Anaesthesia
-
Authors: Kitchen, G. B., et al. (University of Manchester).
-
Publication Date: January 2026.
-
Title: “The influence of time-of-day on outcomes following cardiac surgery: A retrospective analysis of national healthcare data.”
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.