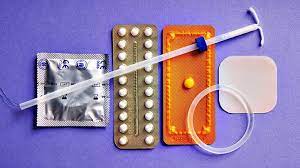
For decades, the “birth control shot” has been a staple of reproductive healthcare. But for most patients, receiving that shot has required a trip to a clinic, a co-pay, and time off work every three months. What many patients—and surprisingly, many doctors—don’t realize is that a version of this medication exists that can be safely administered at home, tucked away in a bathroom cabinet rather than a doctor’s office.
A new study published in the journal Obstetrics & Gynecology reveals a significant gap in American reproductive healthcare: a “hidden” contraceptive option that remains underutilized due to a lack of provider awareness and systemic clinical barriers. Despite being safe, effective, and approved for nearly two decades, self-injectable contraception remains off the radar for the vast majority of healthcare providers.
A Crisis of Awareness
The research, led by experts at the University of California, San Francisco (UCSF), surveyed 422 clinicians across the United States who regularly prescribe contraception. The results were startling. Only about one-third of the clinicians surveyed were even aware that self-injectable contraception was an option for their patients.
Of those who did know about it, only a small fraction actually prescribed it. Ultimately, only 25% of reproductive health experts involved in the study offered the method to their patients.
“Since most physicians don’t know that this is an option, patients don’t know about it,” says Dr. Jennifer Karlin, an associate professor of family and community medicine at UCSF and the study’s senior author. “It’s safe, effective, and puts the control in patients’ own hands. We should be talking about and offering it to patients without biases.”
The implications are clear: when providers are unaware of the full spectrum of contraceptive care, patient autonomy suffers. For individuals living in “contraceptive deserts” or those with demanding schedules, the inability to access a self-administered option creates an unnecessary hurdle to preventing unintended pregnancy.
How It Works: The Science of Subcutaneous DMPA
The medication at the center of this discussion is depot medroxyprogesterone acetate (DMPA), a synthetic form of the hormone progesterone. While the traditional “Depo-Provera” shot is injected deep into the muscle (intramuscular) by a nurse or doctor, the self-injectable version is subcutaneous. This means it is injected into the fatty tissue just beneath the skin—similar to how millions of people self-administer insulin or modern weight-loss medications.
DMPA prevents pregnancy through a triple-action mechanism:
-
Inhibiting Ovulation: It signals the brain to stop the ovaries from releasing an egg.
-
Cervical Mucus Alteration: It thickens the mucus at the cervix, creating a physical barrier that prevents sperm from entering the uterus.
-
Endometrial Thinning: It thins the lining of the uterus, making it less receptive to an embryo.
A single dose provides highly effective pregnancy prevention for 13 weeks. Because the subcutaneous version uses a smaller needle and a lower dose of hormones than the intramuscular version, it is specifically designed for ease of use and reduced discomfort.
Identifying the Barriers
If the technology exists and is effective, why is it so rare in U.S. clinics? The study identified several key “pain points” for providers:
-
Clinical Skepticism: Many doctors expressed concern over whether patients could successfully inject themselves. However, global data suggests that with minimal training, patients are highly proficient at self-administration.
-
Administrative Hurdles: The FDA-approved labeling for the subcutaneous version (DMPA-SC) still technically lists “provider administration,” even though “off-label” self-use is supported by major medical bodies like the American College of Obstetricians and Gynecologists (ACOG). This discrepancy creates confusion regarding liability and insurance reimbursement.
-
Logistical Gaps: Doctors cited a lack of educational brochures, limited pharmacy stock, and the “time crunch” of standard 15-minute appointments as reasons for not teaching patients the technique.
Interestingly, the study found that clinicians in states with more restrictive abortion laws were less likely to prescribe the self-injectable option, suggesting that the broader political climate surrounding reproductive health may influence which tools doctors feel comfortable offering.
Safety Profile and Considerations
As with any hormonal medication, DMPA is not without risks. Long-term use has been associated with a temporary decrease in bone mineral density, leading the FDA to include a “Black Box Warning” advising against use longer than two years unless other methods are inadequate. However, many experts note that bone density typically recovers once the medication is stopped.
More recently, a study published in The BMJ suggested a link between long-term progestogen use and an increased risk of meningioma, a generally non-cancerous brain tumor. While the absolute risk remains very low, it underscores the necessity of the patient-provider dialogue that is currently missing in many clinics.
“The goal isn’t to put everyone on the shot,” says Sarah Miller, a reproductive health advocate and nurse practitioner not involved in the study. “The goal is to ensure the patient knows the shot is an option they can manage themselves if they want to.”
The Path Forward: Lessons from the Pandemic
The COVID-19 pandemic provided a natural experiment for self-injectable birth control. As clinics closed their doors to non-emergency visits, interest in home-based care skyrocketed. In fact, more than half of the clinicians who were aware of self-injection reported learning about it between 2020 and 2022.
In many parts of sub-Saharan Africa, self-injectable DMPA is already a cornerstone of reproductive health, proven to increase “continuation rates” (how long a person stays on birth control) because it removes the barrier of travel.
To bridge the gap in the U.S., the UCSF researchers recommend:
-
Provider Education: Targeted campaigns to update clinicians on ACOG guidelines.
-
Labeling Updates: Encouraging the FDA to update the official label to include self-administration.
-
Pharmacy Access: Ensuring pharmacies stock the subcutaneous version as readily as the intramuscular one.
By moving birth control from the exam table to the bedside table, the medical community can offer patients something often missing in healthcare: true convenience and the privacy of self-care.
Reference Section
- https://www.earth.com/news/most-patients-dont-know-this-birth-control-option-exists/
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
Would you like me to create a printable guide or checklist you can take to your next doctor’s appointment to ask about self-injectable birth control?