India’s journey in immunisation dates back over two centuries, marking a significant chapter in public health and disease prevention. The story began in 1802 when the first smallpox vaccine was administered in Mumbai, laying the foundation for the country’s preventive healthcare system. This pioneering step was crucial in the fight against smallpox, a disease that had plagued India and the world for millennia.
Smallpox, known to have existed for over 3,000 years, was a major cause of mortality, with historic outbreaks such as the 1545 epidemic in Goa claiming thousands of lives. Early preventive efforts included variolation—inoculation with smallpox material to induce mild infection and immunity—which was practiced in India long before the introduction of vaccination. However, the arrival of the smallpox vaccine in 1802 marked a turning point, gradually replacing variolation despite resistance from traditional practitioners and cultural misconceptions.
The initial vaccine doses came from England, and the first Indian recipient was a three-year-old girl in Bombay. The vaccine spread through a human chain of volunteers to other regions, including Madras and Hyderabad. Despite the proven benefits, uptake was slow due to factors such as fees for vaccination, belief in traditional practices, religious objections, and organized opposition by those who feared losing their livelihoods.
The 20th century brought new challenges and developments. Epidemics of cholera and plague, the First World War, and the devastating influenza pandemic diverted attention and resources. Scientific advances revealed that two doses of the smallpox vaccine were necessary for long-lasting protection. Administrative changes under the Government of India Act, 1919, decentralized health responsibilities to provincial governments, shaping the future of vaccine delivery.
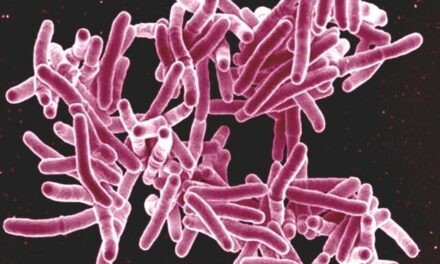
Post-independence, India intensified its immunisation efforts. The establishment of national institutes and vaccine laboratories, along with private manufacturers, supported the eradication of smallpox by 1977. The launch of the Expanded Programme on Immunisation (EPI) in 1978, later renamed the Universal Immunisation Programme (UIP) in 1985, marked a new era. These programs provided free vaccines against multiple diseases, including tuberculosis, polio, measles, and hepatitis B, targeting mothers and children.
Today, the UIP stands as one of the world’s largest public health initiatives, reaching over 26 million newborns and pregnant women annually. A landmark achievement under this program was the eradication of polio, with India declared polio-free in 2014—a milestone that serves as a model for global health efforts.
Despite these successes, challenges remain. Vaccine hesitancy, misinformation, and inequitable coverage continue to hinder full immunisation. Clear, transparent communication and sustained policy focus are essential to overcome these barriers and ensure that the life-saving benefits of vaccines reach every child in India.
: This article is based on information available from historical and recent sources on the evolution of immunisation in India. It aims to provide an overview and does not cover all operational details or address ongoing developments in vaccine research and delivery. Readers are encouraged to consult official health sources for current immunisation guidelines and policies.