In the quest to manage metabolic health, the medical community has long championed the “7 to 9 hours” sleep rule. However, a groundbreaking study is narrowing that window significantly. New research suggests that the “sweet spot” for regulating blood sugar and minimizing insulin resistance may be exactly 7 hours and 18 minutes of sleep per night.
The study, recently published in the peer-reviewed journal BMJ Open Diabetes Research & Care, indicates that straying too far below or above this specific duration could increase the risk of Type 2 diabetes. Perhaps most surprisingly, the research warns that the common habit of “catching up” on sleep during the weekend may actually harm metabolic health for those who already hit their nightly targets.
The Science of the “U-Shaped” Curve
To reach these conclusions, researchers analyzed a massive dataset from the National Health and Nutrition Examination Survey (NHANES), spanning from 2009 to 2023. The study included 23,475 adults between the ages of 20 and 80.
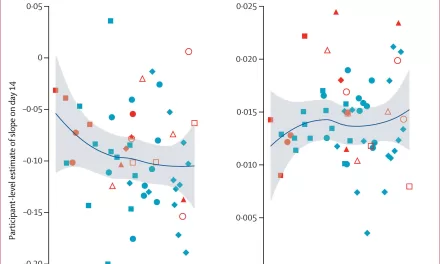
Scientists focused on the estimated glucose disposal rate (eGDR)—a critical metric used to determine insulin sensitivity. A higher eGDR indicates high insulin sensitivity (which is healthy), while a lower eGDR suggests insulin resistance, a precursor to Type 2 diabetes.
The findings revealed a distinct “inverted U-shaped curve.” Insulin sensitivity improved as sleep duration increased toward the 7.32-hour mark ($7$ hours and $19$ minutes, or roughly $7$ hours and $18$ minutes). However, once participants crossed this threshold, their metabolic health began to decline.
“The data suggests a Goldilocks zone for metabolism,” says Dr. Elena Rossi, an endocrinologist not involved in the study. “Too little sleep triggers a stress response that raises blood sugar, but excessively long sleep—more than 7.5 or 8 hours—is also associated with poorer glucose metabolism, particularly in middle-aged women.”
The Danger of the Weekend “Sleep Binge”
For millions of office workers, the “weekend sleep-in” is a cherished ritual. The study found that for those who consistently sleep less than seven hours during the week, an extra hour or two on Saturday and Sunday did provide a modest boost to insulin sensitivity.
However, for those who already achieved the “sweet spot” during the week, sleeping an extra two hours or more on the weekend was linked to an increased risk of impaired glucose metabolism.
“This suggests that consistency is more important than total volume,” explains Sarah Jenkins, a senior sleep researcher. “Irregular sleep patterns—often called ‘social jetlag’—can disrupt the body’s internal clock, which directly governs how we process sugar.”
Why Does Sleep Impact Blood Sugar?
The biological link between the bedroom and the blood-sugar monitor is primarily hormonal. When we are sleep-deprived, the body enters a state of “fight or flight,” increasing levels of:
-
Cortisol: The primary stress hormone that stimulates glucose production.
-
Adrenaline: Which can inhibit the effective release of insulin.
Conversely, oversleeping is often a “proxy” for other health issues. Long sleep durations are frequently correlated with sedentary lifestyles, low physical activity, or underlying conditions like depression—all of which are independent risk factors for metabolic dysfunction.
The researchers noted a “vicious cycle” where poor blood sugar control disrupts sleep (due to frequent urination or night sweats), and that disrupted sleep, in turn, worsens insulin resistance.
The Global Stakes
The timing of this study is critical. According to the World Health Organization (WHO), the global prevalence of diabetes has skyrocketed, rising from 200 million cases in 1990 to over 830 million in 2022.
If left unmanaged, high blood sugar can lead to devastating complications, including:
-
Kidney failure and the need for dialysis.
-
Retinopathy leading to permanent blindness.
-
Increased risk of cardiovascular events, such as heart attacks and strokes.
Study Limitations
While the findings are compelling, the researchers urge caution. Because this was an observational study, it cannot definitively prove that sleeping exactly 7 hours and 18 minutes causes better blood sugar.
“We rely on self-reported data, which can be imprecise,” the authors noted in the report. They also pointed out the possibility of reverse causation: it may be that healthier metabolic systems simply allow for more stable, “optimal” sleep patterns, rather than the sleep duration creating the health.
8 Tips for Reaching Your Metabolic “Sweet Spot”
If you are looking to stabilize your blood sugar through better rest, experts recommend these evidence-based sleep hygiene habits:
-
Prioritize Consistency: Aim to wake up and go to bed within the same 30-minute window every day, including weekends.
-
Seek Morning Light: Exposure to natural sunlight shortly after waking helps calibrate your circadian rhythm.
-
The “Digital Sunset”: Turn off blue-light-emitting devices (phones, tablets) 60–90 minutes before bed to allow melatonin to rise naturally.
-
Watch the Caffeine: Caffeine has a half-life of about 5-6 hours. Avoid it after 12:00 PM to ensure it’s out of your system by bedtime.
-
Cool Your Environment: The body’s core temperature needs to drop to initiate sleep. Keep your bedroom around 18°C (65°F).
-
Gentle Evening Movement: While vigorous exercise is great, finish heavy workouts at least 3 hours before bed. Opt for light stretching or meditation in the evening.
-
Mind Your Diet: Avoid heavy, spicy, or high-sugar meals late at night, as they can cause blood sugar spikes that disrupt deep sleep cycles.
-
Limit Alcohol: While alcohol may help you fall asleep faster, it significantly degrades the quality of restorative sleep and can cause “rebound” high blood sugar.
References
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.