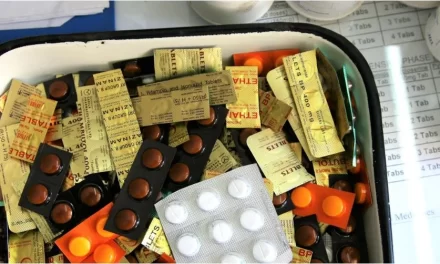
KARACHI, Pakistan — A catastrophic breakdown in medical regulation and infection control has left nearly 4,000 children in Pakistan’s Sindh province HIV-positive, according to a chilling new report that describes the crisis as a “socio-economic catastrophe in the making.”
Despite the 2019 Ratodero tragedy—a mass outbreak that infected hundreds of children and was supposed to be a “never again” moment for the nation—new data reveals that the crisis is accelerating. In 2025 alone, over 100 new pediatric HIV cases were reported in Karachi, pointing to a persistent failure to eliminate the root causes of transmission: reused syringes, unregulated blood banks, and the rampant operation of “quack” clinics.
A Preventable Tragedy
The numbers, released by the Pakistan Medical Association (PMA), are a stark indictment of the country’s healthcare oversight. Of the 3,995 registered HIV-positive children in Sindh, the vast majority were not infected at birth or through personal behavior. Instead, they were infected in the very places meant to provide healing: healthcare facilities.
“What makes this crisis particularly disturbing is that it is largely preventable,” noted a report in The Express Tribune. The investigation highlights a trifecta of systemic failures:
-
Unsafe Injections: The routine reuse of syringes across both private and public sectors.
-
Unregulated Blood Banks: A lack of standardized screening for blood transfusions.
-
The “Quack” Epidemic: An estimated 600,000 unlicensed practitioners operating across Pakistan, with 40% based in Karachi alone.
The Human Cost of Institutional Rot
Medical experts argue that the virus is not “spreading silently”—it is being facilitated by institutional neglect. While the World Health Organization (WHO) and UNAIDS have established clear Standard Operating Procedures (SOPs) for syringe disposal and blood safety, these protocols are frequently ignored in Pakistan.
“This is no longer just a medical emergency,” the PMA warned in its high-level alert. The association described the situation as a “systemic collapse,” where clinics have been turned into “sites of contagion.”
Dr. Aziz Ahmed, a public health consultant (not involved in the PMA report), explains the gravity of the situation: “When we see pediatric HIV cases that are not mother-to-child transmissions, it is an immediate red flag for medical malpractice. A child should never contract HIV during a routine visit for a fever or a cough. This is a crime of negligence.”
By the Numbers: The Scale of the Crisis
| Metric | Statistic |
| Total Registered HIV+ Children (Sindh) | 3,995 |
| New Pediatric Cases in Karachi (2025) | 100+ |
| Estimated Unlicensed “Doctors” in Pakistan | 600,000 |
| Regional HIV Growth Ranking | 2nd in Asia-Pacific |
The European Times reported that Pakistan now ranks second in the Asia-Pacific region for the fastest-growing HIV epidemic. However, health officials fear the documented 3,995 cases are only the “tip of the iceberg,” as testing remains stigmatized and many cases in rural areas go unregistered.
Barriers to Care
For the families already affected, the nightmare does not end with a diagnosis. Pakistan’s HIV treatment centers are reportedly buckling under the pressure. Shortages of:
-
Diagnostic testing kits
-
Pediatric Antiretroviral (ARV) formulations
-
Trained healthcare personnel
These shortages mean that families often travel hundreds of miles, moving from one hospital to another, only to be met with “stock-outs” of the life-saving medication their children need to survive.
Public Health Implications and Global Standards
The crisis in Sindh serves as a global warning about the dangers of unregulated healthcare markets. When “quacks” operate with impunity, they create reservoirs for blood-borne pathogens.
For the general public, the implications are harrowing. In regions where regulation is weak, every medical procedure—from a simple injection to a minor surgery—carries a life-altering risk. Public health experts urge patients to demand to see syringes being unwrapped from sterile packaging and to avoid any clinic that cannot prove its licensing status.
Potential Limitations and Counterarguments
While the data points toward systemic failure, some health officials argue that the rise in “registered” cases is partly due to increased testing and better surveillance compared to a decade ago. However, the PMA maintains that the sheer volume of new pediatric infections in 2025 contradicts the idea that this is simply a “data correction.” The persistent use of multi-dose vials and the lack of a waste management infrastructure for medical sharps remain objective, unaddressed physical risks.
A Call to Action
The PMA and international health bodies are calling for an immediate crackdown on illegal clinics and a rigorous, audited implementation of WHO safety standards. Without a “war footing” approach to medical regulation, the number of infected children is expected to climb, placing an unbearable burden on Pakistan’s future socio-economic stability.
“This is a story of systemic failure that allows the virus to thrive,” the report concludes. The question remains whether the 2025 surge will finally be the catalyst for the reform that the 2019 tragedy failed to secure.
Reference Section
Citations and Reports:
-
The Express Tribune: “PMA Alert: Rising Pediatric HIV Cases in Sindh” (Published Jan 2026).
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.