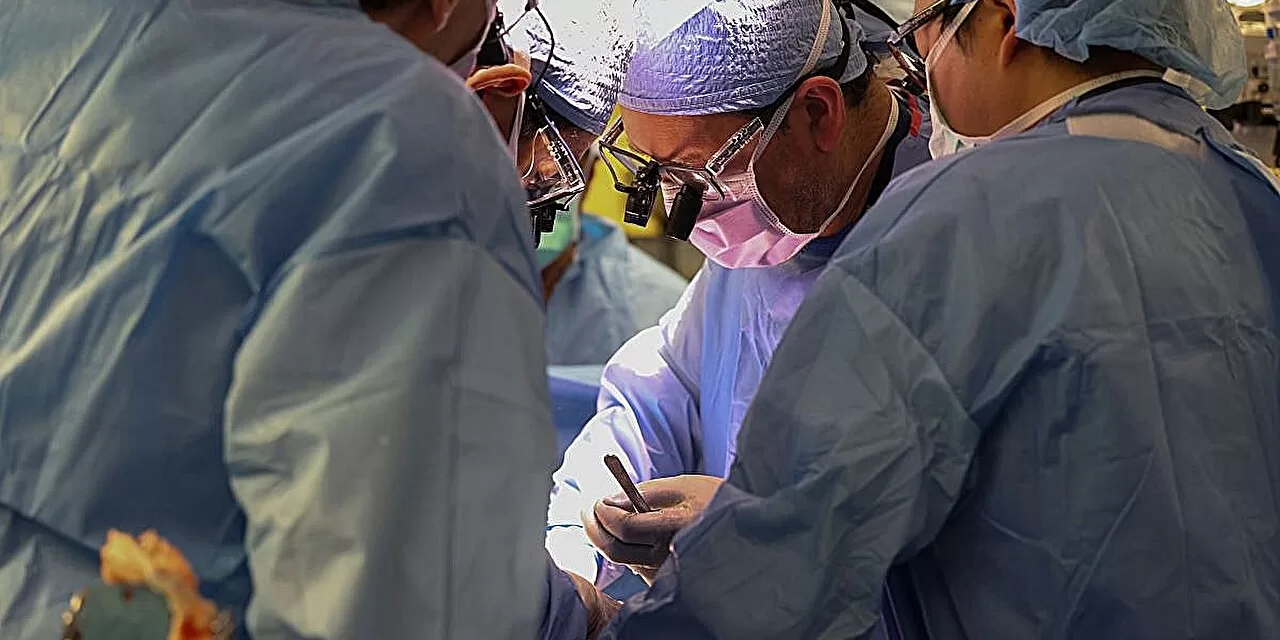
In a landmark study conducted by Harvard Medical School researchers, U.S. surgeons have been found to face a cancer mortality rate more than twice that of their nonsurgical physician counterparts, and approximately 20% higher than the rates observed in most non-physician workers. The research, published in JAMA Surgery, highlights potentially work-related risks unique to the surgical profession, prompting renewed attention to occupational health in medicine.
The investigation, titled “Mortality Among Surgeons in the United States,” analyzed over one million death records from individuals aged 25–74, leveraging data from the 2023 National Vital Statistics System. The cohort included 224 surgeons, 2,740 other physicians, and a diverse group of other professionals, such as lawyers, engineers, and scientists.
Key findings show that surgeons experienced 355.3 deaths per 100,000 population, compared to 228.4 per 100,000 among nonsurgeon physicians, yielding a mortality rate ratio (MRR) of 1.56. While the overall death rates for surgeons still trailed behind those of the general workforce (632.5 per 100,000), their mortality patterns bore closer resemblance to other high-education professions like lawyers, engineers, and scientists, whose rates stood at 404.5 per 100,000.
A striking outlier emerged with cancer mortality: surgeons suffered 193.2 cancer deaths per 100,000, more than double the 87.5 per 100,000 observed in nonsurgeons, translating to an MRR of 2.21. Notably, cancer was the only category where surgeons exceeded all other worker groups, with the next highest being 162.0 per 100,000 for the general workforce.
Analysis of other causes of death showed disparities driven by occupational and lifestyle factors. For instance, car accident mortality was higher among surgeons (13.4 per 100,000) than among other physicians, yet still below the 16.6 per 100,000 rate seen across all workers. Surgeons were the least likely group to die from respiratory diseases, influenza, kidney or liver disease, septicemia, and diabetes, reflecting general health advantages within the profession.
Researchers suggest that because surgical and nonsurgical physicians share similar levels of health knowledge and access to resources, the excess cancer deaths hint at possible surgery-specific workplace exposures or stressors. Eliminating the surplus of 105.7 cancer deaths per 100,000 would bring surgeons’ overall mortality rates in line with their non-surgical peers.
Disclaimer:
This article is based on early findings from a peer-reviewed study published in JAMA Surgery. Medical and scientific research continues to evolve, and further investigation is necessary to determine causation and underlying mechanisms. This content is intended for informational purposes only and should not be interpreted as medical advice. For concerns about occupational health risks, consult a qualified healthcare professional.