NEW DELHI — The Supreme Court of India has officially commenced a landmark examination into the safety of the nation’s blood supply, weighing whether the “Right to Safe Blood” should be recognized as an intrinsic part of the fundamental Right to Life under Article 21 of the Constitution.
The case, triggered by a public interest litigation (PIL) filed by the NGO Sarvesham Mangalam Foundation, seeks to mandate Nucleic Acid Testing (NAT)—a highly sensitive molecular screening method—across all licensed blood banks in India. The bench, led by Chief Justice Surya Kant and supported by Justices Joymalya Bagchi and Vipul M. Pancholi, is currently evaluating the feasibility of replacing or augmenting traditional screening methods to protect patients from transfusion-transmissible infections (TTIs) such as HIV and Hepatitis.
The “Window Period” Risk: Why Current Screening May Fall Short
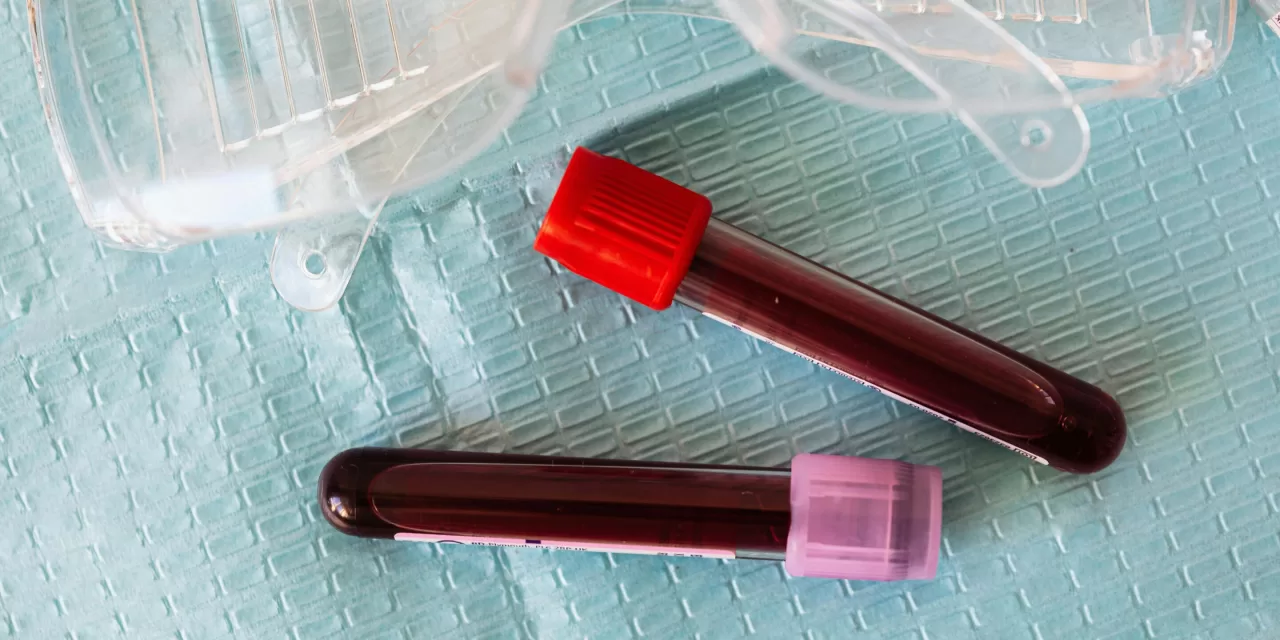
For decades, Indian blood banks have primarily relied on the Enzyme-Linked Immunosorbent Assay (ELISA) to screen donated blood. While ELISA is a robust and globally recognized tool, it has a critical limitation known as the “window period.”
When a person is first infected with a virus like HIV or Hepatitis B, there is a span of days or weeks during which the body has not yet produced enough antibodies or antigens for ELISA to detect. If an infected individual donates blood during this window, the blood may test negative despite carrying the live virus.
Nucleic Acid Testing (NAT) addresses this gap by looking for the genetic material (DNA or RNA) of the virus itself, rather than the body’s immune response.
-
HIV: NAT can reduce the undetectable window by approximately 10–15 days compared to third-generation ELISA.
-
Hepatitis C (HCV): The window can be shortened by several weeks.
-
Hepatitis B (HBV): NAT significantly improves detection of “occult” infections where surface antigens are not present.
The petition argues that for the thousands of patients in India—particularly children with thalassemia who require lifelong, frequent transfusions—current protocols turn a life-saving procedure into a “gamble with death.”
The Human Cost: Thalassemia and the “Safe Blood” Lifeline
India is often referred to as the “Thalassemia capital of the world.” Patients with this inherited blood disorder cannot produce enough healthy hemoglobin and rely on regular blood transfusions to survive.
According to documented cases presented in the PIL and various media reports, several patients have allegedly contracted HIV or Hepatitis after receiving blood from government facilities. “For multi-transfused patients, even a single missed infection can have lifelong, devastating consequences,” notes Dr. Neelam Marwaha, a veteran transfusion medicine expert.
Beyond the physical toll, the financial burden of managing a secondary chronic infection like Hepatitis C—which can lead to cirrhosis or liver cancer—is often insurmountable for families already struggling with the costs of primary care.
Feasibility vs. Fundamental Rights: The Court’s Dilemma
While the medical superiority of NAT is largely undisputed, the Supreme Court has raised pointed questions regarding its practical implementation and economic viability. Chief Justice Kant has requested a detailed “cost audit” and a mapping of existing facilities, expressing concern for economically weaker states.
The Cost-Benefit Debate
The transition to universal NAT screening involves significant hurdles:
-
High Infrastructure Costs: NAT requires specialized equipment, stable electricity, and climate-controlled environments.
-
Recurring Expenses: The reagents and kits used in molecular testing are substantially more expensive than ELISA counterparts.
-
Fragmented System: With over 2,500 licensed blood centers in India, many in rural or underfunded areas, a blanket mandate could lead to the closure of essential local facilities that cannot afford the upgrade.
Potential Solutions Under Review
To balance safety with solvency, health economists have suggested several intermediate strategies:
-
Pooled Testing: Combining samples from multiple donors into a single “pool” for testing. If the pool is negative, all units are cleared. If positive, individual units are then tested. This significantly lowers the per-test cost.
-
Phased Rollout: Prioritizing NAT for high-volume regional centers or specifically for blood destined for high-risk groups like pregnant women and thalassemia patients.
Public Health Implications and Limitations
It is important to note that while NAT is a powerful tool, it is not a “magic bullet.” Public health experts emphasize that blood safety is a multi-layered process.
“NAT is an additional layer of safety, but it does not replace the need for rigorous donor selection and adherence to basic banking standards,” says a spokesperson from a prominent health authority.
If the Court declares safe blood a fundamental right, it could force a massive overhaul of the national blood system, including better “haemovigilance” (monitoring the entire transfusion chain). However, some critics argue that in regions where basic infrastructure is lacking, investing in reliable electricity and trained staff for existing protocols may save more lives than a single advanced test.
What This Means for You
For health-conscious citizens and patients, this case highlights the importance of transparency in healthcare. If you or a loved one requires a transfusion, medical professionals suggest:
-
Asking about screening: Inquire whether the blood has been screened using NAT or ELISA.
-
Voluntary Donation: Encourage healthy friends and family to donate, as “replacement” or “voluntary” donors often carry a lower risk profile than unknown sources.
-
Avoid Delay: Despite the ongoing debate, clinicians stress that if a transfusion is medically necessary for an acute condition, the risk of refusal (e.g., severe anemia or blood loss) is almost always higher than the risk of infection.
The Supreme Court’s eventual ruling will likely be a defining moment for Indian healthcare, determining whether the high cost of technology can be allowed to stand in the way of a patient’s right to the safest possible treatment.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Economic Times. (2026, Feb 25). Supreme Court seeks details on cost, availability of NAT in hospital to prevent transfusion-related infection.