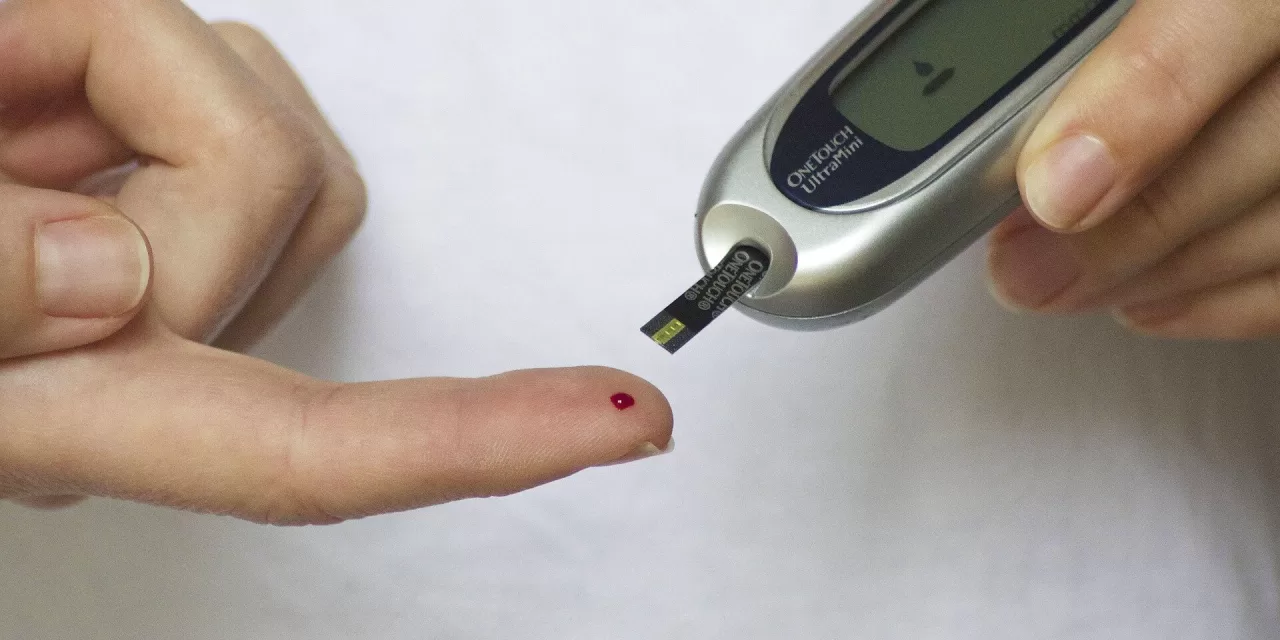
For the 38 million Americans living with diabetes, the daily routine is a relentless marathon of glucose monitoring, carbohydrate counting, and medication adherence. Yet, even when patients follow their regimens to the letter, their blood sugar levels often remain stubbornly high. When this happens, clinical guidelines are clear: it is time to intensify treatment.
But a growing body of evidence suggests that for millions, that next step never comes.
This phenomenon is known as therapeutic inertia (TI)—a clinical stalemate where healthcare providers fail to initiate or intensify therapy when a patient’s goals are not met. Despite decades of pharmacological breakthroughs, therapeutic inertia remains a silent barrier, leaving patients at increased risk for devastating complications like heart disease, kidney failure, and vision loss.
The Data of Stagnation
Therapeutic inertia is not a new concept, but recent data suggests the problem is worsening. According to a landmark study published in early 2025, glycemic control rates in the United States have seen a troubling decline. The research found that overall control rates dropped from 54.3% in 2023 to just 43.5% by the end of the following year.
Perhaps most alarming is the impact on young adults (aged 20-44), where control rates plummeted from 57.4% to a staggering 37.1%.
“Many people don’t realize that each diabetes medication targets a different physiological pathway,” says Barbara Eichorst, MS, RD, Vice President of Health Care Programs at the American Diabetes Association (ADA). “Relying on just one agent may not adequately address the complexity of diabetes management.”
The issue extends beyond blood sugar. A three-year study of 52,750 clinical visits in Chicago, published in 2025, revealed that while 33.8% of older adults had uncontrolled blood pressure, 73.4% of those cases met the definition of therapeutic inertia. Essentially, the high readings were documented, but the treatment plan remained unchanged.
A Tale of Two Perspectives: Why We Stall
The reasons for this “clinical freeze” are multifaceted, involving a complex tug-of-war between provider constraints and patient fears.
The Provider’s Hurdles
Primary Care Physicians (PCPs) are the frontline defenders in diabetes management, yet they are often overextended. Research suggests the average PCP may spend only about one hour per week reading new medical literature. In a standard 20-minute appointment, a doctor must address blood sugar, blood pressure, cholesterol, foot checks, and mental health.
“PCPs are notoriously busy,” explains Michael W. Latreille, MD, of the University of Vermont Medical Center. “It is much easier to ignore an elevated reading, blame it on the circumstances of the day, or ‘kick the can down the road’ when the schedule is packed.”
The Patient’s Emotional Burden
For the patient, the recommendation to add a second or third medication—or to transition to insulin—is often met with a sense of personal failure.
“There is often an emotional component, such as feelings of guilt or fear,” Eichorst notes. “Patients need to understand that diabetes is a progressive disease. Adding another medication is not a setback; it’s a strategic and natural step in managing the pathophysiology of the condition.”
Breaking the Cycle: New Solutions
If the problem is systemic, the solution must be as well. Recent interventional studies are providing a roadmap for “killing the inertia” by using technology and streamlined education.
A 2025 study led by Dr. Latreille at the University of Vermont focused on 43 PCPs across four clinics. The goal was to increase the prescription of life-saving medications like SGLT2 inhibitors and GLP-1 receptor agonists. The intervention hit three specific “pain points”:
-
Accessible Education: Providing prescribing information via podcasts and easy-to-digest printouts.
-
EHR Dashboards: Modifying Electronic Health Records to flag patients who were overdue for care or eligible for treatment changes.
-
Visual Progress: Sending quarterly “report cards” to doctors so they could see their own prescribing trends.
The results were telling: 90% of the participating physicians successfully prescribed the indicated medications, and 81% committed to continuing the practice.
“Providers like to see the numbers move,” says Dr. Latreille. “It makes the fruits of our efforts tangible.”
Public Health Implications
The stakes of therapeutic inertia are high. While patient behavior and medication adherence are often blamed for poor outcomes, some researchers argue that physician-led inertia has a significantly higher impact on long-term disease control.
When a patient sits in an “uncontrolled” state for years, the cumulative damage to the vascular system becomes irreversible—a concept known as metabolic memory. Addressing TI isn’t just about lower numbers today; it’s about preventing a heart attack ten years from now.
Recommendations for Patients
How can patients ensure they aren’t victims of therapeutic inertia? Advocacy is key.
-
Ask “Why?”: If your A1c or blood pressure is above your target goal, ask your doctor: “Why aren’t we changing my medication or dosage today?”
-
Track Your Trends: Use apps or logs to show your doctor that a high reading wasn’t just “white coat syndrome” or a one-time fluke.
-
Reframe the Goal: View medication changes as “upgrading your defense” rather than a sign of personal failure.
As Dr. Latreille shifts his focus to tackling inertia in hypertension management, the message for the medical community is clear: the data is already in the chart. The next step is simply having the courage to take it.
References
- https://www.medscape.com/viewarticle/when-therapeutic-inertia-hits-diabetes-care-2026a1000160
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.