South Carolina health authorities reported a dramatic 99% increase in measles cases, reaching 310 confirmed infections as of January 9, 2026. This spike, concentrated in multiple counties, underscores growing concerns over declining vaccination rates and outbreaks linked to unvaccinated communities. The development highlights the urgent need for renewed public health measures to curb this highly contagious disease.
Outbreak Details and Timeline
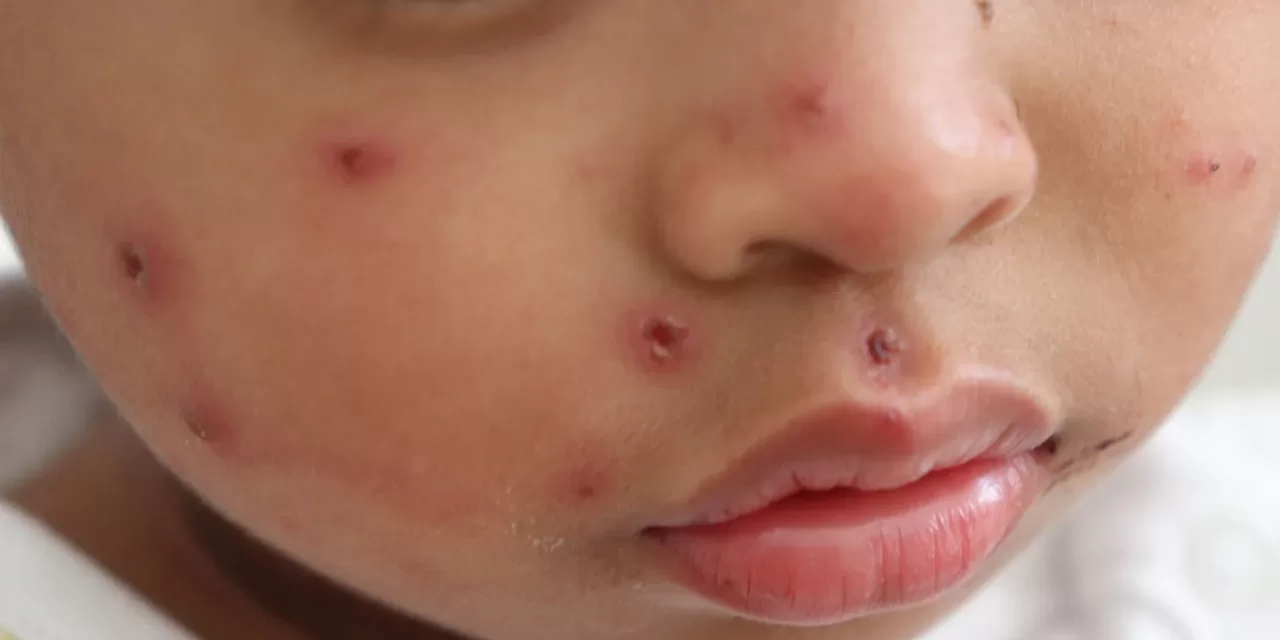
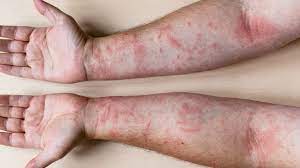
The South Carolina Department of Health and Environmental Control (DHEC) announced the latest figures on January 9, 2026, revealing 310 cases—a sharp rise from earlier reports in late 2025. Most cases stem from community transmission in the Upstate region, including Greenville and Spartanburg counties, with infections spreading through schools, churches, and households. Symptoms typically appear 7-14 days after exposure, including high fever, cough, runny nose, red eyes, and a characteristic rash; complications like pneumonia affect up to 1 in 20 cases, particularly in young children.
Health officials trace the outbreak to an index case in October 2025, likely imported from international travel, amplified by pockets of low vaccination coverage below the 95% herd immunity threshold. DHEC has declared outbreaks in seven counties, administering over 5,000 vaccine doses in response clinics since November.
Key Findings on Spread and Impact
Measles, caused by a paramyxovirus, spreads via airborne droplets and remains one of the world’s most contagious pathogens—up to 18 people can contract it from one infected individual in a susceptible population. In South Carolina, 85% of cases involve unvaccinated children under 18, with hospitalization rates nearing 20%, straining local pediatric wards. Nationally, the CDC reports over 1,200 cases across 30 states by early January 2026, marking the worst year since measles was declared eliminated in 2000.
Vaccination status reveals a stark divide: the MMR vaccine (measles, mumps, rubella) is 97% effective with two doses, yet kindergarten coverage dipped to 92.7% in 2024-2025, per CDC data. Outbreaks disproportionately hit religious or philosophical exemption communities, where exemption rates exceed 5% in affected areas.
Expert Commentary
Dr. Linda Bell, South Carolina’s state epidemiologist, stated, “This surge is preventable tragedy. Measles doesn’t discriminate, but vaccination does protect the vulnerable—infants too young for shots and those with medical contraindications.”
Dr. Paul Offit, director of the Vaccine Education Center at Children’s Hospital of Philadelphia and a pediatrician uninvolved in the outbreak response, emphasized, “Herd immunity isn’t abstract; it’s why we eradicated measles domestically. Dropping below 95% invites resurgence, as seen here. Parents delaying vaccines risk not just their child but the community.” Offit highlighted the vaccine’s 50-year safety record, with serious side effects rarer than 1 in a million doses.
Broader Context and Historical Trends
Measles was declared eliminated in the U.S. in 2000 after widespread MMR vaccination, but global travel and vaccine hesitancy—fueled by debunked 1998 claims linking MMR to autism—have reversed gains. The WHO reports 306,000 global cases in 2024, with deaths rising 79% since 2019 due to pandemic disruptions. In the U.S., 2025 saw clusters in 22 states, often tied to under-vaccinated enclaves.
South Carolina’s outbreak aligns with national trends: Florida reported 96 cases in December 2025, while New York and Ohio saw smaller flares. Federal funding for vaccination campaigns increased by $50 million in 2025, yet misinformation on social media persists, per a 2025 Pew Research study finding 30% of parents cite online sources for vaccine decisions.
Public Health Implications
This outbreak threatens vulnerable groups: immunocompromised patients, pregnant individuals (risking congenital rubella syndrome), and vitamin A-deficient children prone to blindness. Economically, each U.S. case costs $3,000-$17,000 in treatment and contact tracing, per CDC estimates; South Carolina’s response exceeds $2 million already.
For everyday health decisions, officials urge verifying vaccination records—two MMR doses for adults born after 1957—and isolating symptomatic individuals. Free clinics offer catch-up shots, with DHEC partnering with pharmacies for walk-ins. Pregnant people or travelers to endemic areas like India or Yemen should consult providers.
Limitations and Counterarguments
While alarming, officials note no deaths in South Carolina yet, unlike 2015’s California outbreak (1 fatality). Critics of mandates, including some parent groups, argue personal freedom trumps public mandates, citing rare allergic reactions (1 in 40,000). However, courts have upheld school requirements, and studies show exemptions correlate with 35-fold higher outbreak risk (JAMA Pediatrics, 2015).
Ongoing genomic sequencing may pinpoint imported strains, but data lags limit real-time insights. Long-term, addressing hesitancy requires countering misinformation without alienating communities.
Conclusion: Call to Action
South Carolina’s 99% case surge to 310 signals a public health emergency demanding swift vaccination drives and education. With President Trump’s administration pledging support via HHS, containment hinges on community buy-in to restore herd immunity.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
South Carolina Department of Health and Environmental Control (DHEC). “Measles Outbreak Update: 310 Cases Confirmed.” January 9, 2026. https://www.reuters.com/business/healthcare-pharmaceuticals/measles-cases-south-carolina-rise-by-99-310-state-health-department-says-2026-01-09/