SPARTANBURG, S.C. — In a dramatic escalation of the nation’s most severe measles crisis in over 30 years, South Carolina health officials are bypassing traditional federal deployments in favor of private-sector reinforcements. As of February 24, 2026, the South Carolina Department of Public Health (DPH) has confirmed 979 cases of the highly contagious virus, marking the largest single-state outbreak since 1992.
The surge, centered in the state’s Upstate region, has prompted officials to request at least 12 infectious disease specialists from the nonprofit CDC Foundation. The move to seek external “boots on the ground” for contact tracing and case investigation—rather than relying solely on short-term teams from the Centers for Disease Control and Prevention (CDC)—signals a shift in how states may handle high-stakes public health crises in a post-pandemic political landscape.
A Rapidly Expanding Footprint
The outbreak’s epicenter lies in Spartanburg County, specifically the northwestern corridor including Boiling Springs and Greer. What began as a handful of cases in October 2025 exploded in January 2026.
According to DPH data, the 979 confirmed cases in South Carolina now account for more than 90% of all measles infections nationwide this year. For context, the CDC logged 982 cases across 26 states as of February 19, meaning the Palmetto State is currently the primary battleground for the virus in the U.S.
The Vaccination Gap by the Numbers:
-
Unvaccinated: 913 cases (93%)
-
Fully Vaccinated: 26 cases
-
Partially Vaccinated: 19 cases
-
Unknown Status: 21 cases
To date, at least 21 individuals have been hospitalized. While no fatalities have been reported in South Carolina this year, the sheer volume of cases is straining local resources. The virus has already “spilled over” state lines into North Carolina and Ohio, leading to school-wide quarantines and restricted access to public spaces.
Why Measles Is a “Fire in Dry Brush”
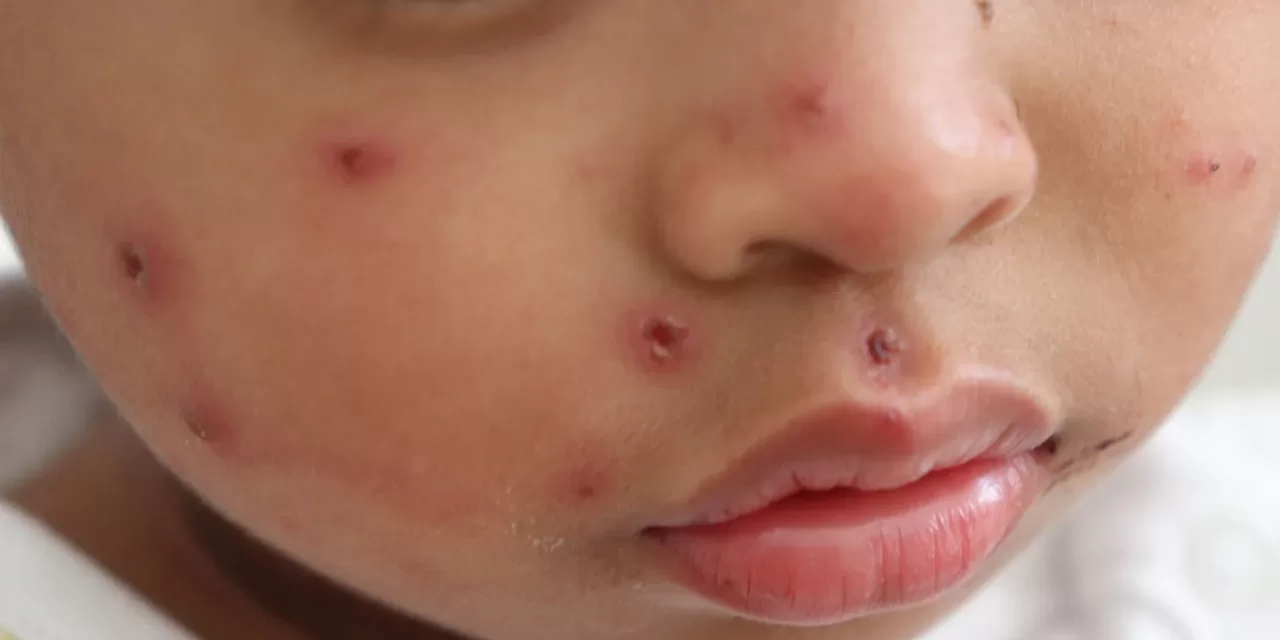
Measles is not just a “childhood rash”; it is one of the most infectious diseases known to science. Caused by a paramyxovirus, it spreads through respiratory droplets that can linger in the air for up to two hours after an infected person has left the room.
“If one person has it, up to 90% of the people close to that person who are not immune will also become infected,” explains Dr. Robin LaCroix, a pediatric infectious disease specialist at Prisma Health. Dr. LaCroix, who is currently managing a significant number of active cases, likens the spread to a spark in dry brush. “Vaccination is the only firewall we have.”
Symptoms typically appear 7 to 14 days after exposure, beginning with a high fever (often exceeding 104°F), cough, coryza (runny nose), and conjunctivitis (red, watery eyes). The hallmark red, blotchy rash usually begins at the hairline and spreads downward. However, the danger lies in the complications: one in five unvaccinated people who get measles will be hospitalized, and some may suffer permanent hearing loss or life-threatening brain swelling (encephalitis).
The Crisis of Confidence: Vaccination Rates Plummet
The primary driver of the current crisis is a sharp decline in Measles, Mumps, and Rubella (MMR) vaccine coverage. While the U.S. declared measles “eliminated” in 2000, that status relies on maintaining a 95% vaccination rate to ensure herd immunity.
In some South Carolina schools, officials report that MMR coverage has dipped to as low as 20%. State Epidemiologist Dr. Linda Bell pointed to post-COVID-19 vaccine hesitancy as a major factor.
“There are areas…where vaccination rates in specific schools dip to as low as 20%,” Dr. Bell noted, emphasizing that while South Carolina has school entry requirements, exemptions have increased.
The decision to seek aid from the CDC Foundation—a nonprofit established by Congress to support the CDC—rather than direct federal personnel, is a notable strategic turn. Former CDC Director Dan Jernigan suggested this route might be “much more politically palatable” in regions where federal intervention is viewed with skepticism, allowing the state to maintain more direct control over the response.
Expert Perspectives: A National Vulnerability
Outside experts warn that the South Carolina outbreak is a “canary in the coal mine” for the rest of the country.
“We feel like we’re really on the brink,” says Dr. John Elkes, an emergency physician at Prisma Health who is not directly involved in the DPH response. “The situation is about to worsen significantly if we cannot close these immunity gaps. We are seeing community spread in grocery stores, gyms, and post offices.”
The World Health Organization and the Pan American Health Organization (PAHO) are closely monitoring the situation. If a single strain of measles circulates within the U.S. for 12 consecutive months, the country could officially lose its “eliminated” status—a major setback for American public health.
Balancing the Narrative: Risks and Realities
While the vaccine is the primary tool for prevention, it is not without its limitations. Approximately 3% of fully vaccinated individuals (those who have received both doses) may still contract measles if exposed, though their symptoms are typically much milder.
Furthermore, public health officials acknowledge that concerns over vaccine side effects, such as rare febrile seizures, have contributed to parental anxiety. However, medical authorities emphasize that the risk of severe complications from a measles infection—such as pneumonia or encephalitis—is hundreds of times higher than the risk of a serious adverse reaction to the vaccine.
What This Means for You: Practical Steps
For the general public, the South Carolina outbreak serves as a reminder to verify immunization records.
-
Check Your Status: Most adults born after 1957 should have documentation of two MMR doses. If you are unsure, a simple blood test (titer) can confirm immunity.
-
Act Quickly After Exposure: If you are unvaccinated and exposed to measles, receiving the MMR vaccine within 72 hours—or immunoglobulin (antibodies) within six days—can often prevent the disease or lessen its severity.
-
Protect the Vulnerable: Infants under 12 months, pregnant women, and the immunocompromised cannot receive the live MMR vaccine. They rely entirely on the “herd immunity” provided by those around them.
As the number of cases in Spartanburg County continues to climb, the message from the medical community remains singular: the tools to stop this outbreak exist, but they must be used.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
South Carolina Department of Public Health. (2026, Feb 24). Measles Outbreak Dashboard: Case Counts and Exposure Locations.