December 8, 2025
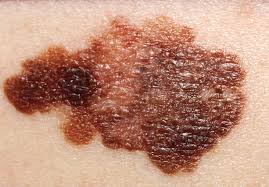
A radical shift in treating advanced skin cancer is offering patients better survival rates with a fraction of the traditional treatment time. New data released this week confirms that giving just two doses of immunotherapy before surgery is significantly more effective than the standard year-long course of drugs administered after tumor removal.
The findings, stemming from the landmark Phase III NADINA trial, suggest that for many patients with stage III melanoma, a six-week “short course” of treatment could effectively replace twelve months of therapy, drastically reducing the burden on patients while improving their odds of remaining cancer-free.
The “Neoadjuvant” Revolution
Historically, the standard of care for resectable stage III melanoma (cancer that has spread to lymph nodes but can still be surgically removed) involved surgery first, followed by one year of “adjuvant” immunotherapy to mop up any remaining microscopic cancer cells. While effective, this approach requires lengthy hospital visits and exposes patients to side effects for a full year.
The new approach reverses this order—a strategy known as neoadjuvant therapy. Patients receive two cycles of a combination immunotherapy (ipilimumab and nivolumab) over six weeks, followed by surgery.
“We are seeing a paradigm shift in real-time,” said Dr. Christian Blank, the lead investigator of the NADINA trial, in a statement accompanying the results. “By activating the immune system while the tumor is still present, we train the body’s defenses to recognize and destroy the cancer more effectively than if we removed the bulk of the disease first.”
Key Findings: Less Is More
The latest updates presented at the 2025 European Society for Medical Oncology (ESMO) Congress paint a compelling picture of efficacy:
-
Survival Benefit: At 24 months, 77.3% of patients who received the two pre-surgical doses remained event-free (meaning no cancer recurrence), compared to 55.7% of those who received standard surgery plus a year of postoperative drugs.
-
Tumor Destruction: Remarkably, nearly 60% of patients in the neoadjuvant group achieved a “Major Pathologic Response” (MPR). This means that when surgeons went to remove the tumor after just two doses, they found mostly dead cancer cells or no active cancer at all.
-
Treatment Cessation: For patients who achieved this deep response, no further treatment was required after surgery—saving them from roughly 46 weeks of additional drug infusions.
“The idea that we can give two infusions and potentially be done with treatment is revolutionary for patients,” notes Dr. Michael Lowe, a surgical oncologist not involved in the study. “It essentially turns a chronic, year-long battle into a focused, six-week intervention with superior results.”
Why It Works
The science behind this “short course” success lies in the presence of the tumor itself. Immunotherapy drugs work by taking the brakes off the immune system. When a large tumor is present (neoadjuvant setting), there are more targets (antigens) for the immune system to learn from. This creates a stronger, more diverse army of T-cells capable of hunting down cancer cells throughout the body.
If the tumor is removed first (adjuvant setting), the immune system has fewer clues to work with, potentially leading to a weaker defense against recurrence.
Implications for Patients
For 45-year-old Mark Davidson, a participant in an early phase of the trial, the difference was life-altering. “I prepared myself for a year of feeling sick and missing work,” Davidson shared. “Instead, I had two treatments, a surgery, and then… life just went back to normal. My scans have been clear for over two years.”
This approach also addresses “scanxiety”—the dread patients feel before check-ups—by offering earlier reassurance. Patients who show a strong response in the pathology report after surgery effectively get an early signal that their long-term prognosis is excellent.
Limitations and Risks
While the results are promising, experts urge caution regarding side effects. The combination of ipilimumab and nivolumab is more potent than the single-drug regimens often used in the adjuvant setting.
-
Toxicity: In the neoadjuvant arm, approximately 30% of patients experienced grade 3 or higher immune-related adverse events (such as liver inflammation or colitis), compared to about 15% in the standard arm.
-
Monitoring: “Because the treatment is more intense, it requires a specialized team to monitor for side effects closely,” explains Dr. Sam Godfrey, a research engagement lead at Cancer Research UK. “However, because the duration is so short, most side effects are manageable and resolve quickly, unlike the chronic low-grade fatigue often seen with year-long therapy.”
Furthermore, this approach is currently applicable to “macroscopic” stage III melanoma—cases where the lymph nodes are palpable or clearly visible on scans. Research is ongoing to see if earlier-stage cancers could benefit from similar strategies.
The Bottom Line
The NADINA trial results solidified in late 2025 represent one of the most significant advances in melanoma care in a decade. By moving immunotherapy to the front of the line, doctors can now offer patients a higher chance of a cure with significantly less time spent in the infusion chair.
“This is not just about better statistics,” Dr. Lowe adds. “It’s about giving people their year back.”
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Primary Study: Blank, C. U., et al. (2025). “Neoadjuvant Nivolumab and Ipilimumab in Resectable Stage III Melanoma: Updated 2-Year Results from the NADINA Trial.” Presented at the European Society for Medical Oncology (ESMO) Congress 2025.