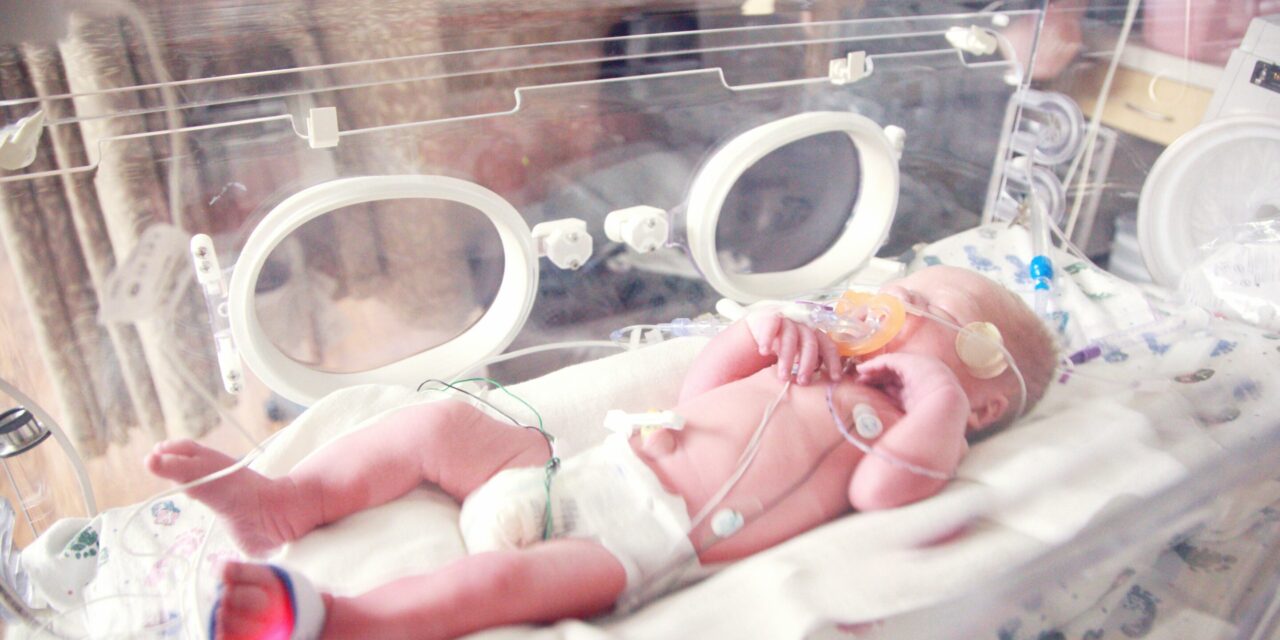
Patients hospitalized with community-acquired pneumonia (CAP) who suffer from severe Vitamin D deficiency face a significantly higher risk of long-term mortality compared to those with adequate levels, according to new research published this month. The study, conducted by researchers at Copenhagen University Hospital and published in Open Forum Infectious Diseases, found that patients with Vitamin D levels below 25 nmol/L were more than three times as likely to die within three to six months of admission than those with sufficient levels. These findings add critical weight to the growing body of evidence suggesting that Vitamin D plays a pivotal role in respiratory immune defense and recovery.
The Silent Risk Factor
Community-acquired pneumonia remains a leading cause of hospitalization and death worldwide, particularly among older adults. While age and comorbidities are well-known risk factors, this new Danish study highlights a potentially modifiable variable: Vitamin D status.
The research team, led by Maria Hein Hegelund of the Department of Pulmonary and Infectious Diseases at Copenhagen University Hospital, analyzed data from 514 patients hospitalized with CAP. They categorized patients’ Vitamin D levels upon admission as sufficient (≥50 nmol/L), insufficient (25 to <50 nmol/L), or deficient (<25 nmol/L).
The results were striking. After adjusting for confounding factors such as age, sex, smoking history, and other health conditions, patients with Vitamin D deficiency had a:
-
3.5-fold increased risk of dying within 90 days of admission (Odds Ratio 3.50).
-
3.3-fold increased risk of dying within 180 days (Odds Ratio 3.27).
Interestingly, the study did not find a significant difference in short-term mortality (in-hospital or 30-day death rates) between the groups. The researchers suggest this may be due to the relatively small number of immediate deaths in the cohort, which limited the statistical power to detect early differences.
Why Vitamin D Matters for Immunity
While often associated with bone health, Vitamin D is increasingly recognized as a potent immunomodulator. “Vitamin D is essential for activating our immune system’s defenses,” explains Dr. Carlos Camargo, a Professor of Emergency Medicine at Harvard Medical School who has extensively studied Vitamin D’s role in respiratory health (not involved in this specific study). “It triggers the production of antimicrobial peptides—natural antibiotics that line our respiratory tract—and helps regulate the inflammatory response to prevent it from becoming destructive.”
This “regulatory” function is crucial in pneumonia. In severe cases, the body’s immune response can go into overdrive—a “cytokine storm”—causing more damage to lung tissue than the infection itself. Vitamin D helps dampen this excessive inflammation while still allowing the immune system to fight the pathogen.
Putting the Findings in Context
The new Danish study aligns with previous research but offers a crucial distinction: the importance of severity. The increased death risk was specifically driven by frank deficiency (<25 nmol/L). Patients with “insufficient” levels (25–50 nmol/L) did not show a statistically significant difference in mortality compared to those with sufficient levels.
This nuance is consistent with meta-analyses led by researchers like Professor Adrian Martineau of Queen Mary University of London, which have previously shown that Vitamin D supplementation is most effective at preventing respiratory infections in people who are profoundly deficient to begin with. “The evidence suggests that the ‘low-hanging fruit’ for public health is correcting severe deficiency,” notes Martineau in previous commentary on the subject. “People with normal levels are unlikely to see a boost from taking more, but for those at the bottom of the range, it can be a lifesaver.”
Implications for Patients and Clinicians
For the general public, particularly during the winter months when sunlight exposure is low, these findings serve as a reminder to monitor Vitamin D intake.
“Our results and those from other studies indicate that maintaining serum 25(OH)D concentrations above 50 nmol/L may be beneficial for reducing mortality risk among both hospitalized and nonhospitalized individuals,” stated lead author Maria Hein Hegelund in the study’s release.
However, experts caution against interpreting this as a call to megadose vitamins indiscriminately. The goal is to reach a “sufficient” level, not an excessive one. Standard recommendations typically involve taking a daily supplement of 10-20 micrograms (400-800 IU) during winter months, though individuals with darker skin or limited sun exposure may require year-round supplementation.
Study Limitations
While the findings are compelling, the study has limitations. It was an observational cohort study, meaning it can prove an association but not a direct cause-and-effect relationship. It is possible that patients with low Vitamin D were frailer in ways the researchers couldn’t fully measure (unmeasured confounders). Additionally, the study noted potential selection bias, as some of the sickest patients declined to participate.1
Despite these caveats, the strength of the association—a tripling of death risk—makes a strong case for ensuring Vitamin D adequacy,2 especially in vulnerable populations.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
Primary Study:
-
Hegelund, M. H., et al. (2025). Vitamin D Deficiency at Hospital Admission With Community-Acquired Pneumonia is Associated With Increased Risk of Mortality: A Prospective Cohort Study. Open Forum Infectious Diseases. DOI: 10.1093/ofid/ofaf706. Published online November 19, 2025.