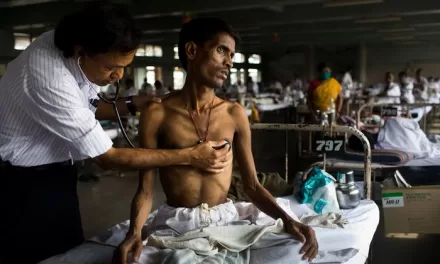
Rural hospitals in the U.S. are increasingly closing their labor and delivery units, leaving communities-particularly in states like Texas-grappling with reduced access to critical maternal healthcare. According to a report by the Center for Healthcare Quality & Payment Reform, 101 rural hospitals nationwide have stopped delivering babies since 2020, including three in Texas. The state now has 93 rural hospitals without obstetrics services, contributing to a maternal health emergency where 47% of Texas counties are classified as “maternity care deserts,” far exceeding the national average.
The Financial Strain Behind Closures
Labor and delivery units are often the first casualties of financial instability in rural hospitals. Staffing these units 24/7 is costly, and low patient volumes in rural areas mean many hospitals operate at a loss. “You’re paying people to sit waiting for births that rarely happen,” said Harold Miller, CEO of the Center for Healthcare Quality & Payment Reform. Closing these units can prevent total hospital shutdowns, but the consequences are dire for patients.
Maternal Health Outcomes Worsen
The closures force pregnant individuals to travel long distances for care, delaying critical interventions during emergencies. Texas already faces stark maternal health challenges: its maternal mortality rate is 34.7 deaths per 100,000 live births, well above the national average of 26.3. The Rural Texas Maternal Health Assembly warns that “rurality itself is a factor in the maternal health crisis,” as travel burdens reduce survival odds for mothers and infants.
Legislative Efforts and Proposed Solutions
Advocates are pushing for systemic reforms. Harold Miller emphasizes the need for federal and state funding to cover standby costs for rural hospitals. In Texas, Rep. Gary VanDeaver’s House Bill 18 aims to stabilize rural hospitals through grants and a new state office focused on rural healthcare finance. The bill passed the Texas House in April and now moves to the Senate.
Telemedicine and Medicaid expansion are also proposed as solutions, though the latter faces political hurdles in Texas. John Henderson, CEO of the Texas Organization of Rural & Community Hospitals, stressed the urgency: “Rural hospitals aren’t going to be less vulnerable in the near term. We need innovative projects now.”
Disclaimer: This article is based on information sourced from Medical Xpress’s coverage of rural hospital closures (https://medicalxpress.com/news/2025-04-rural-america-hospitals-labor-delivery.html), which cites data from the Center for Healthcare Quality & Payment Reform and the Rural Texas Maternal Health Assembly. Original reporting and statements are attributed to the sources listed above.