The CDC has reported a significant rise in endocarditis-related deaths among pregnant and postpartum women in the United States, with mortality rates increasing more than fivefold between 2012 and 2019. This emerging trend highlights a growing public health concern within maternal health, particularly as substance use disorders may be contributing to the rise in cases of infective endocarditis during pregnancy.
Key Findings from CDC Data
Between 2012 and 2019, endocarditis-related deaths accounted for 12.4% of all infection-related pregnancy-related mortalities, making it the second most common infectious cause after sepsis, which accounted for 46.4% of such deaths. The pregnancy-related mortality ratio for endocarditis rose sharply from 0.10 per 100,000 live births in 2012 to 0.56 in 2019, representing a more than fivefold increase. This upward trend occurred despite stable or declining rates for other infection-related causes such as chorioamnionitis and urinary tract infections, which remained below 0.20 throughout the study period.
The data were derived from the CDC’s Pregnancy Mortality Surveillance System (PMSS), which analyzed 5,309 pregnancy-related deaths occurring during or within one year of pregnancy across all U.S. states, the District of Columbia, and New York City. Pregnancy-related deaths were defined as those occurring during or within one year after pregnancy, with causes determined by medically trained epidemiologists through review of death certificates and linked birth or fetal death records. The study excluded years affected by the COVID-19 pandemic to prevent confounding of infection-related mortality patterns.
Demographic and Clinical Patterns
A notable demographic pattern emerged in the data: 79.1% of endocarditis-related pregnancy deaths occurred among non-Hispanic White women. This finding aligns with broader national trends showing rising rates of infective endocarditis among younger adults, particularly those aged 25 to 44, driven in part by substance use disorders. Research indicates that substance use disorder was present in nearly 90% of pregnant and postpartum women diagnosed with infective endocarditis in two U.S. cohorts.
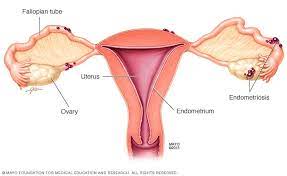
Infective endocarditis (IE) is a serious infection of the heart valves or inner lining of the heart, often caused by bacteria entering the bloodstream—commonly through intravenous drug use, dental procedures, or other sources of bacteremia. During pregnancy, physiological changes such as increased blood volume and cardiac output can exacerbate underlying valvular heart disease, increasing susceptibility to IE and its complications. Studies show that maternal mortality from IE during delivery is extremely high, reaching 17.2% compared to less than 0.01% in women without IE.
Expert Perspectives and Clinical Implications
Medical experts emphasize that the rise in endocarditis-related maternal deaths may be preventable with earlier detection and integrated care. “The reason for the increase in endocarditis-related deaths cannot be determined from this dataset. However, the prevalence of substance use disorder among pregnant and postpartum women with infective endocarditis approached 90% in two U.S. cohorts; this may have contributed to the increased incidence,” the study authors noted. They recommend the involvement of multidisciplinary care teams—including specialists in addiction medicine, cardiology, and infectious diseases—to improve outcomes.
Dr. Mohammad Ahabab Hossain, a cardiovascular researcher at Rutgers New Jersey Medical School, highlighted the broader context of rising cardiovascular-related maternal mortality, which more than doubled between 1999 and 2022. “We’re heading in the wrong direction,” he stated, emphasizing that preventable causes, including heart infections, continue to claim lives due to systemic gaps in care, particularly among vulnerable populations.
Public Health and Preventive Strategies
The CDC findings underscore the need for enhanced screening and intervention strategies, especially for women with known risk factors such as pre-existing heart conditions or substance use disorders. Early recognition of symptoms—such as persistent fever, fatigue, new heart murmurs, or unexplained weight loss—can be critical in diagnosing IE before it leads to severe complications.
Preventive measures include antibiotic prophylaxis for high-risk patients undergoing certain dental or surgical procedures, though guidelines have become more selective in recent years. Equally important is addressing the social determinants of health, including access to addiction treatment, prenatal care, and mental health services, which are essential for reducing maternal mortality.
Limitations and Future Directions
The study has limitations, including potential misclassification of pregnancy-related deaths due to incomplete or inaccurate death records. Additionally, the underlying source of infection leading to sepsis may not always be documented, possibly resulting in underreporting of specific conditions like endocarditis. Future research should focus on longitudinal studies and expanded data from Maternal Mortality Review Committees (MMRCs), which provide more detailed, case-level insights into preventable factors.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.