A wireless retinal implant can restore central vision in patients with advanced age-related macular degeneration (AMD), according to clinical trial results published Oct. 20, 2025, in the New England Journal of Medicine. Advanced atrophic AMD, also known as geographic atrophy (GA), is the leading cause of irreversible blindness in older adults, affecting more than 5 million people worldwide.
The international, multicenter trial was co-led by José-Alain Sahel, Distinguished Professor of Ophthalmology and Eye and Ear Foundation Department of Ophthalmology Professor and Chair, School of Medicine, University of Pittsburgh; Daniel Palanker, professor of ophthalmology, Stanford University; and Frank Holz, professor of ophthalmology, University of Bonn, Germany.
Of the 32 participants who completed 12 months of follow-up, 26 achieved clinically meaningful improvements in visual acuity, and 27 participants reported using the prosthetic vision system tested in the trial at home for reading numbers or words. On average, participants improved by 25 letters—about five lines—on a standard eye chart when using the device. Eighty-one percent of participants gained 10 or more letters.
“It’s the first time that any attempt at vision restoration has achieved such results in a large number of patients,” said Sahel, senior author of the study and director of the UPMC Vision Institute. “More than 80% of the patients were able to read letters and words, and some of them are reading pages in a book. This is really something we couldn’t have dreamt of when we started on this journey, together with Daniel Palanker, 15 years ago.”
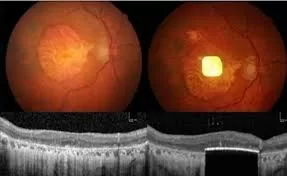
As AMD progresses, the center of vision becomes increasingly blurry due to the irreversible damage to the light-sensing cells in the central part of the retina. In a healthy retina, those cells capture ambient light from the environment and transform it into pulses of electricity, which are then sent to nerve cells lining the back of the eye and, eventually, to the brain through the optic nerve.
The PRIMA system, originally designed by Palanker, replaces these lost photoreceptors with a 2×2 mm flexible wireless implant that converts light into electrical signals to stimulate remaining retinal cells. A camera mounted on specialized glasses captures images and projects them onto the implant using invisible near-infrared light. The implant then converts the light into electrical pulses, restoring the flow of visual information to the brain. Patients can adjust zoom and contrast settings to enhance functional vision.
The PRIMAvera trial enrolled 38 participants aged 60 and older at 17 sites across five European countries: France, Germany, Italy, the Netherlands and the United Kingdom.
After one year of using the system, all procedure-related adverse events had subsided and the majority of participants showed significant improvement in their ability to read letters on the eye chart. One participant improved by as many as 59 letters, or 10 lines.
“I don’t think we’ll ever be able to restore full 20/20 vision with the implant alone, but we are investigating tricks that could further improve people’s quality of life and take them above the threshold for legal blindness,” Sahel said. “One of the main requests we hear from patients is to be able to recognize faces and emotions again, and that’s something we’re working toward.”
Based on these results, the device manufacturer, Science Corporation, has applied for clinical use authorization in Europe. UPMC was the first U.S. center to implant the PRIMA device in 2020 in a study led by Joseph Martel, associate professor of ophthalmology, School of Medicine.
Other authors of the study include investigators at The Adolphe de Rothschild Foundation Hospital and The 15-20 National Eye Hospital, Paris; Moorfields Eye Hospital, London; and University of Rome Tor Vergata, among others.
The study was financed by Science Corporation, Alameda, California (previously Pixium Vision SA, Paris, France).