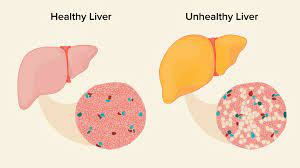
Fatty liver disease (FLD), particularly its non-alcoholic form (NAFLD), has emerged as a silent yet widespread public health concern, now estimated to affect approximately 38% of adults globally. Contrary to the common perception that fatty liver results merely from excess fat accumulation in the organ, emerging expert insights reveal a more complex interplay involving nutritional imbalances and metabolic dysfunctions that underlie disease progression. This evolving understanding calls for a paradigm shift in managing and preventing the condition—a move away from simply restricting dietary fats towards restoring nutritional balance, especially addressing micronutrient deficiencies and managing carbohydrate intake.
Redefining Fatty Liver Disease: Beyond Fat Accumulation
Conventional wisdom often views fatty liver as a straightforward consequence of excessive fat consumption. However, leading functional medicine experts and recent research suggest that the issue is nuanced, with critical roles played by specific nutrients such as copper, vitamin A, and fructose, the sugar naturally present in fruits. Copper and vitamin A participate actively in the liver’s ability to process and shuttle iron safely out of the organ to avoid cellular damage. When these nutrients are deficient, iron accumulates in the liver, causing oxidative stress and cellular injury, which in turn triggers fat deposition. A striking analogy used by Dr. Robert DeBease, a functional medicine specialist, likens iron buildup to a truckload stuck in a warehouse, creating downstream congestion and damage that ultimately impairs liver function.
Fructose metabolism adds another layer of complexity. Unlike glucose, fructose is metabolized primarily in the liver, and excessive intake—especially in the context of existing copper and vitamin A deficits—can overwhelm hepatic processing capacity, exacerbating liver cell injury. This has profound implications given prevalent high-fructose consumption in modern diets. Studies in animal models have demonstrated that copper deficiency combined with fructose intake synergistically worsens liver steatosis and injury, highlighting the multifactorial nature of NAFLD pathogenesis.
Nutritional Strategy: Moving Beyond Fat Restriction
Dr. DeBease advocates a comprehensive dietary approach that prioritizes nutritional adequacy and metabolic support rather than focusing solely on restricting fat intake. Key components include:
-
Eliminating all fruits from the diet to reduce fructose load on the liver
-
Reducing overall carbohydrate intake to moderate metabolic stress
-
Emphasizing quality proteins and healthy fats to support liver repair and function
-
Incorporating nutrient-dense organ meats, such as liver, which are rich in copper and vitamin A
Foods naturally high in copper and vitamin A—such as carrots, sweet potatoes, kale, eggs, and pumpkin—are recommended to enhance iron metabolism and facilitate liver cell regeneration. This approach aligns with a growing body of evidence underscoring the importance of micronutrient sufficiency in NAFLD prevention and management.
Expert Perspectives and Scientific Context
The association between copper deficiency and fatty liver disease is well-supported in scientific literature. Research published in reputable journals demonstrates that copper insufficiency disrupts lipid metabolism and antioxidant defenses, thereby promoting NAFLD progression. Fructose, although naturally found in fruits, can contribute to hepatic lipogenesis and inflammation when consumed in excess, particularly in susceptible individuals with micronutrient imbalances.
Moreover, emerging research identifies “hidden hunger” — micronutrient deficiencies that remain undiagnosed — as a significant yet underexplored aspect of metabolic fatty liver disease. Vitamins A, E, D, C, zinc, selenium, and magnesium are often depleted in NAFLD patients, exacerbating oxidative stress and impairing liver function. Addressing these deficits through diet or supplementation offers promising avenues to halt or even reverse disease progression.
The Liver-Adrenal Axis: Hormonal Implications
Beyond nutrient metabolism, the liver’s role extends to hormonal regulation, particularly through its interaction with the adrenal glands in managing stress via cortisol modulation. A compromised liver strains the adrenal system, potentially leading to widespread physiological dysfunction. Restoring liver health, therefore, may improve hormonal balance and resilience against stress-related disorders, adding a vital dimension to holistic patient care.
Implications for Public Health and Daily Life
For readers concerned about liver health, this evolving understanding emphasizes that managing fatty liver disease involves more than just cutting fats from the diet. It requires a balanced, nutrient-rich dietary pattern that supports the liver’s metabolic functions and prevents micronutrient deficiencies. Practical steps include:
-
Mindful reduction of high-fructose foods, including limiting fruit intake under clinical guidance
-
Moderation of carbohydrate consumption with an emphasis on low glycemic, fiber-rich options
-
Prioritizing nutrient-dense foods rich in copper and vitamin A
-
Considering organ meats, like liver, as beneficial additions to the diet
Balanced reporting also recognizes that traditional dietary recommendations such as the Mediterranean diet, which emphasizes whole grains, fruits, vegetables, and healthy fats, remain effective for many patients. Individualization remains key, as micronutrient needs and metabolic responses vary.
Limitations and Balanced Considerations
While the role of copper, vitamin A, and fructose in fatty liver disease is increasingly recognized, further large-scale clinical studies are needed to establish causality and optimal intervention protocols firmly. Complete elimination of fruits may not be necessary or appropriate for all individuals, and dietary changes should be personalized with healthcare professional input. Additionally, broader lifestyle factors including physical activity, weight management, and avoidance of alcohol are crucial components of comprehensive fatty liver care.
Medical Disclaimer:
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References:
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11186518/
- https://daijiworld.com/news/newsDisplay?newsID=1295884