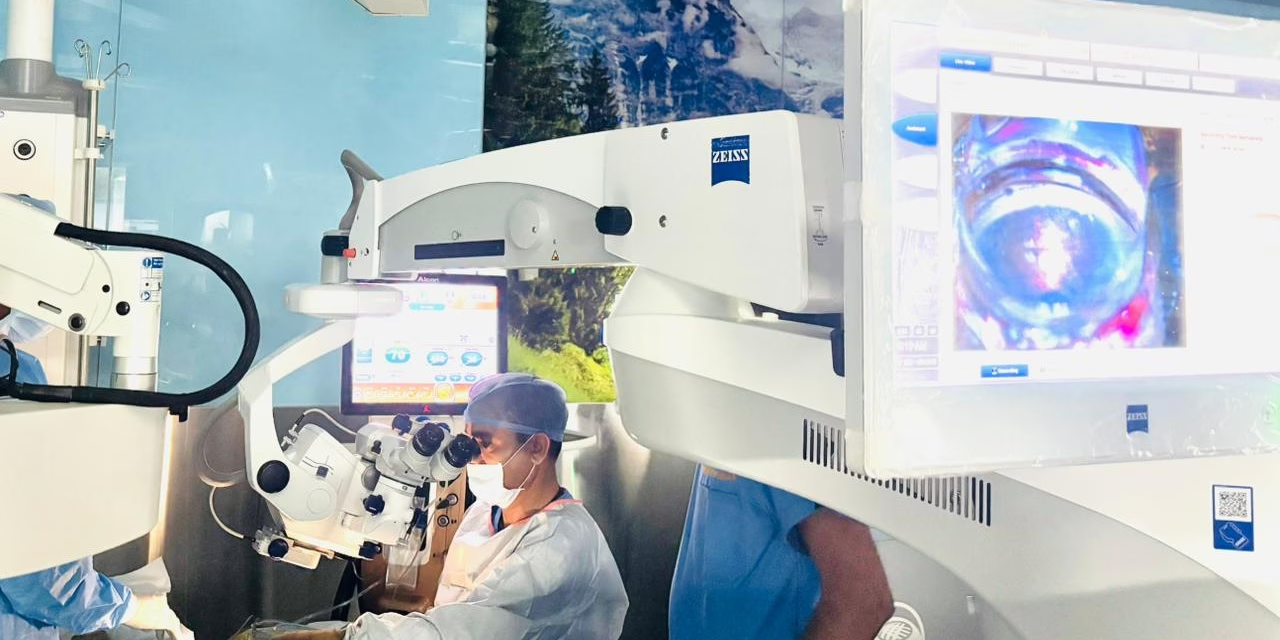
NEW DELHI — In a milestone for ophthalmic surgery, surgeons at the Army Hospital (Research & Referral) in Delhi have successfully performed a world-first procedure combining a specialized glaucoma implant with real-time imaging of the eye’s drainage system.
The procedure, conducted on March 10, 2026, involved the implantation of a Hydrus Microstent guided by intraoperative aqueous angiography during a routine cataract surgery. By using advanced imaging to visualize exactly where fluid exits the eye, the surgical team was able to place the device with unprecedented precision.
The operation was overseen by the Director General Armed Forces Medical Services, Surgeon Vice Admiral Arti Sarin, marking a significant leap in the modernization of medical care within the Indian Defence Forces and the global ophthalmology community.
The Silent Thief and the Need for Precision
Glaucoma is often called the “silent thief of sight” because it frequently has no symptoms until permanent vision loss occurs. It is typically caused by a buildup of fluid (aqueous humor) that increases internal eye pressure, eventually damaging the optic nerve.
For years, the gold standard for treatment was eye drops or invasive “filtering” surgeries. However, the rise of Minimally Invasive Glaucoma Surgery (MIGS) has changed the landscape. These procedures use tiny devices to bypass blockages in the eye’s natural drainage system.
The Challenge of “Blind” Placement
While MIGS devices like the Hydrus Microstent—a hair-thin scaffold made of nitinol—are highly effective, surgeons traditionally place them based on anatomical landmarks. They “guess” the most active drainage areas because the microscopic channels that carry fluid away from the eye are usually invisible to the naked eye during surgery.
“Think of it like trying to clear a city’s drainage system during a storm without a map of the pipes,” says Dr. Aruna Singh, an independent ophthalmologist and glaucoma specialist (not involved in the procedure). “You know the pipes are there, but you don’t know which ones are actually flowing and which are clogged.”
A World First: Aqueous Angiography
What sets the Army Hospital (R&R) procedure apart is the use of aqueous angiography using the Heidelberg Retina Angiograph (HRA).
During the surgery, a biocompatible fluorescent dye is introduced into the eye. The HRA imaging system then captures the flow of this dye in real-time, highlighting the “hot spots”—the specific areas of Schlemm’s canal and collector channels that are most active in draining fluid.
Key Benefits of the Procedure:
-
Targeted Placement: The stent is placed exactly where the eye’s natural drainage is strongest.
-
Reduced Resistance: By bypassing the most obstructed areas, the device maximizes the reduction of intraocular pressure (IOP).
-
Efficiency: Combining the procedure with cataract surgery allows patients to address two major vision issues in a single sitting, often reducing their dependence on daily eye drops.
Expert Commentary and Global Significance
The success of this surgery suggests a shift toward “personalized” glaucoma care. Instead of a one-size-fits-all approach, surgeons can now tailor the surgery to the unique plumbing of an individual’s eye.
“The integration of intraoperative angiography into MIGS is a game-changer,” says Dr. Rajesh Khanna, a senior consultant in Ophthalmic Surgery. “It moves us from ‘anatomical’ surgery to ‘functional’ surgery. We aren’t just putting a device where the canal is; we are putting it where the canal works.”
According to data from the World Health Organization (WHO), glaucoma is the second leading cause of blindness globally. In India, it is estimated that 12 million people are affected, with many remaining undiagnosed. Innovations that increase the success rate of early interventions are critical for public health.
Limitations and Considerations
Despite the excitement surrounding this world-first, medical experts urge a balanced perspective.
-
Cost and Accessibility: The HRA imaging system and the Hydrus Microstent are high-cost technologies. Currently, this level of precision is limited to premier research institutions like Army Hospital (R&R).
-
Learning Curve: Performing angiography inside the eye during an active surgery requires specialized training and a highly coordinated surgical team.
-
Long-term Data: While real-time imaging improves placement, long-term studies will be needed to confirm if angiography-guided placement leads to significantly better 5-year outcomes compared to traditional MIGS.
What This Means for Patients
For those living with glaucoma, this development offers a glimpse into the future of vision preservation. While the technology may take time to become a standard of care in local clinics, it proves that “precision medicine” has arrived in the field of ophthalmology.
Patients currently managing glaucoma with multiple medications should consult their doctors about whether they are candidates for MIGS, especially if they are already scheduled for cataract surgery.
Reference Section
Primary Source:
-
Press Information Bureau (PIB) Delhi. “Global First in Minimally invasive Glaucoma Surgery with aqueous angiography at Army Hospital (R&R), Delhi.” Published March 11, 2026.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.