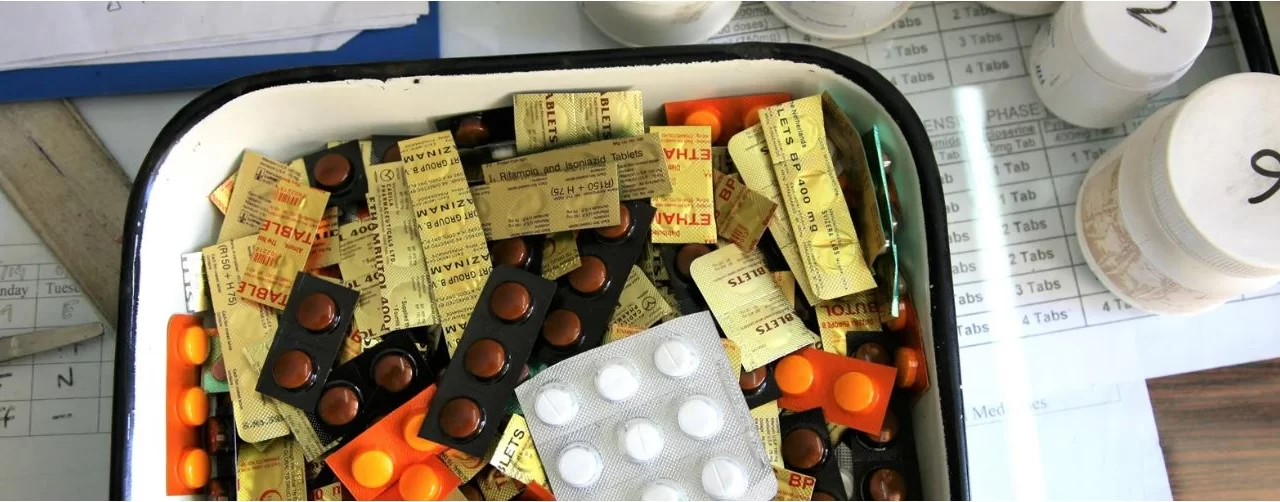
Healthcare providers’ belief that patients expect antibiotics—even when not medically indicated—could be a key driver behind India’s troubling rates of antibiotic overprescription and rising antimicrobial resistance (AMR), according to new research published in the journal Science Advances on September 10, 2025. This evidence-based investigation challenges long-held assumptions about the motivations behind antibiotic use and highlights urgent opportunities for intervention to safeguard future public health.
Unpacking the Study: Who, What, When, Where, Why
A multidisciplinary team from the University of Southern California, Indian Institute of Management Bangalore, and NEERMAN, a Delhi-based research institute, conducted over 2,000 “mystery patient” visits and surveyed more than 2,200 healthcare practitioners—including pharmacists, MBBS doctors, rural clinicians, and traditional medicine providers—across 253 towns in Karnataka and Bihar. Their aim: to understand why antibiotics are so routinely prescribed for pediatric diarrhea, a condition most often caused by viruses rather than bacteria.
Key findings revealed that 70% of practitioners prescribed antibiotics instead of oral rehydration salts (ORS)—the recommended treatment for most cases of childhood diarrhea—despite the absence of evidence for bacterial infection.
What Drives Prescribers? Not Profit or Ignorance
Contrary to popular belief, the study found that overuse wasn’t generally motivated by a lack of clinical knowledge or financial incentives. Instead, many practitioners wrongly assumed that patients would doubt their competence if antibiotics were not prescribed, thinking families expected a tangible—even if unnecessary—treatment. This “perception gap” between practitioner beliefs and patient expectations appears to be a critical factor fueling antibiotic overuse.
However, when patients in the experiment voiced a preference for ORS over antibiotics, the rate of unnecessary antibiotic prescriptions dropped by 20%, highlighting the power of clear communication between patients and providers.
Patients Aren’t Actually Demanding Antibiotics
In a complementary component of the research, 1,189 caregivers were surveyed about their provider preferences. Results showed that patients do not favor practitioners who automatically prescribe antibiotics—in fact, such prescribing did not influence their trust or provider loyalty. This disconnect between perceived and actual patient desires has important implications for strategies aimed at reducing inappropriate prescriptions.
Expert Commentary and Broader Context
Dr. Vinus Taneja, Consultant Department of Internal Medicine, Sir Ganga Ram Hospital—who was not involved in the study—notes, “Antibiotics are invaluable but must only be used when absolutely necessary. Misuse, driven by either patient or provider misconceptions, allows resistance to build up silently. Education for both groups is vital to curb this trend”.
Dr. Kamini Walia, senior scientist at the Indian Council of Medical Research (ICMR), adds, “Every year, we document a rise in antimicrobial resistance rates linked to overconsumption. Most troubling is the increase in use of ‘watch group’ antibiotics, reserved for more severe infections but frequently prescribed unnecessarily”.
Public Health Implications: A Worsening Crisis
India is currently facing one of the world’s worst AMR crises. Recent Indian Centre for Disease Control (NCDC) surveillance shows high antibiotic consumption within tertiary care hospitals, with 71.9% of admitted patients prescribed antibiotics—57% from classes associated with high risks of resistance. Globally, AMR is projected to cause 39 million deaths by 2050 if current trends continue, with India seen as a major hotspot due to over-the-counter sales, rampant self-medication, and inconsistent stewardship programs.
Worryingly, only a small fraction of antibiotic prescriptions in Indian hospitals are written for definite diagnoses—upwards of 94% are empirical, driven by symptoms rather than confirmed infections. Such practices not only foster resistance but lead to “superbug” infections that are harder and more expensive to treat, with significant mortality risk.
Addressing the Problem: Strategies and Challenges
India’s government has taken important steps—such as implementing the National Action Plan on AMR and enforcing stricter Schedule H prescription-only rules—but challenges remain. Over-the-counter sales at pharmacies are still common, particularly in rural areas. Some doctors admit to prescribing antibiotics for “prophylaxis”—to prevent secondary infections—even when not recommended by treatment guidelines.
Public and doctor education holds promise. When both parties understand that most fevers, coughs, colds, and childhood diarrheal illnesses are viral—not bacterial—they can resist unnecessary antibiotic treatment. “Diagnostic tests, vaccination, and following recommended treatments are the best ways to avoid overprescription and resistance,” says Dr. Kapil Borawake, an intensive care specialist.
Potential Limitations and Counterarguments
While the new study leverages robust data from real-world provider encounters and large-scale surveys, limitations include geographic focus on only two states—Karnataka and Bihar—and simulated illness. Prescription patterns may vary in other Indian settings or clinical contexts. Broader issues such as pharmacy regulation, agricultural antibiotic use, and health infrastructure deficits further complicate AMR.
Some practitioners may feel pressured to “play it safe” with antibiotics due to limited diagnostic resources or the fear of missing rare but serious bacterial infections—a challenge acknowledged by many Indian clinicians.
What This Means for Daily Health Decisions
For readers and healthcare consumers in India and beyond, the most important takeaway is to engage in open conversations with healthcare providers. Ask if antibiotics are truly needed for a specific illness, understand the risks of unnecessary use, and follow prescribed courses closely if antibiotics are indeed indicated. For practitioners, the study underscores the need to communicate evidence-based recommendations and avoid succumbing to misplaced assumptions about patient expectations.
Medical Disclaimer
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.